Case Report: Secondary bilateral parkinsonism and dystonia treated with dronabinol
Abstract
Drug abuse may damage basal ganglia that are essential for planning and execution of movements. We report about the case of a 38-year old patient with ischemic lesions of the basal ganglia presenting with bilateral painful dystonia and parkinsonism caused by polyintoxication. Dronabinol resulted in improvement of pain and gait disturbance, suggesting a novel therapeutic strategy in these challenging patients.
Article type: Case Report
Keywords: dronabinol, secondary parkinsonism, dystonia, intoxication, ischemic stroke
Affiliations: Department of Neurology, Medical University of Warsaw, Warsaw, 02091, Poland; Department of Bioethics, Medical University of Warsaw, Warsaw, 02091, Poland; Division of Neurocritical Care, Department of Neurology, Yale University, New Haven, Connecticut, 06519, USA; District Hospital Kufstein, Kufstein, Austria; Department of Neurology, Medical University of Innsbruck, Innsbruck, Austria
License: Copyright: © 2021 Szejko N et al. CC BY 4.0 This is an open access article distributed under the terms of the Creative Commons Attribution Licence, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Article links: DOI: 10.12688/f1000research.26476.3 | PubMed: 34484695 | PMC: PMC8381340
Relevance: Core topic: mentioned in title and keywords
Full text: PDF (772 KB)
Introduction
Drug abuse is an important health issue, not only affecting the social surrounding of a patient but also the cerebral integrity. Besides a number of different somatic abnormalities provoked by an intoxication, certain drugs may damage areas of the brain, such as basal ganglia or cortex, which are essential for the movement onset and coordination 1– 3 .
In this case report, we present a 38-year-old male patient with a long-lasting history of drug misuse, including the abuse of cocaine, cannabinoids, benzodiazepines, opiates, methadone and amphetamines. As a result of the multi-intoxication induced bilateral ischaemic lesions to the basal ganglia, the patient presented with secondary bilateral dystonia and parkinsonism. It is not certain whether the cause of ischemia could be related to any specific drug or combinations thereof. However, it is clear that primary and secondary movement disorders have different pathophysiology and, therefore, require different treatments 4– 6 . Cocaine and its metabolites are known to cause cerebral vasospasm that could lead to ischemic infarctions in the whole brain 1, 7, 8 or can provoke haemorrhagic stroke 3. Heroin causes ischemia more often in the globus pallidus 9. Amphetamines are known as the second most frequent cause of ischemia after cocaine, especially in younger patients due to their vasoconstrictive effect 10. Although it is not clear whether cannabinoids and its metabolites can cause cerebrovascular events, there is evidence that cannabis can increase the risk for haemorrhagic stroke 11. Opioids may not have a direct toxic impact on the neurons, but ischaemic lesions or necrosis can be triggered by recurrence of drug-induced hypoxia 12.
The aim of this case report is to show the possible use of dronabinol for a multi-intoxicated patient with ischemia of the basal ganglia in order to temper his pain and improve gait.
Case report
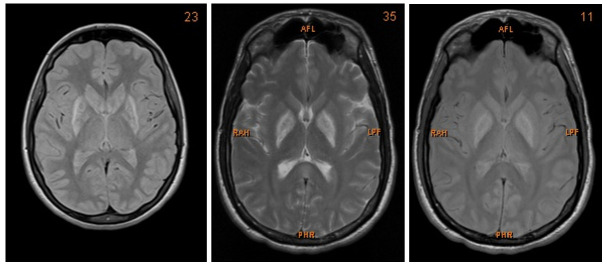
We present a case of a 27-year-old Caucasian man who was admitted to the Intensive Care Unit (ICU) after multi-intoxication. Drug screening on admission identified the following substances: opiates, benzodiazepines, cannabinoids, crack cocaine, methadone and amphetamine. Due to the history of drug abuse he was unemployed. During the first days the patient was in coma, with Glasgow Coma Scale of 5 points. After slow amelioration of his status he presented with severe dysarthria, dysphagia, as well as bilateral parkinsonism and dystonia of his extremities. The neurological examination showed a bilateral positive Babinski sign, global rigidity in all extremities as well as symmetrical hyperreflexia. Furthermore, he suffered from high fever that resolved after treatment with benzodiazepines. Therefore, vegetative symptoms accompanying the patient on admission were interpreted as drug withdrawal syndrome. Both, CT and MRI showed bilateral hypoxemic infarction of the basal ganglia and boundary zone ( Figure 1). Those changes could be the consequence of the mixed intoxication or could be attributed to only one harmful substance, especially crack cocaine or amphetamine. During the hospitalization he developed a tracheobronchitis and respiratory insufficiency due to acute respiratory distress syndrome (ARDS). Moreover, because of severe dysphagia he was nourished via percutaneous endoscopic gastrostomy. Further consequences of his primary condition included post ischemic epilepsy treated with levetiracetam (1000mg). After six months of intensive care, the patient was discharged from the hospital.
During the next five years the patient was treated with levodopa (titrated up to 800mg/day), apomorphine (up to 100 mg/day), selegiline (10mg/day) and baclofen (75mg/day). Further up-titration of levodopa was not possible because of subsequent side effects, such as hallucinations. Due to sleeping problems and agitation he was treated with trazodone (150mg/day) and quetiapine (250mg/day). The substitution dose of buprenorphine 20mg/day was tapered off constantly to keep the patient in a drug naive state. Nonetheless, he showed aggressive behaviour under the influence of alcohol and was admitted to psychiatric ward several times due to delusional disorder and recurrent addictive behaviours. After several months of psychiatric treatment, his addiction and hallucinations resolved. In spite of intense treatment, both parkinsonism as well as dystonia persisted for years and additional symptoms such as generalized pain as well as gait disturbances occurred.
During the examination in our outpatient clinic, 11 years after the hospitalization in the ICU, the patient was still experiencing moderate dysarthria, bilateral dystonia of all extremities, bilateral akinetic-rigid parkinsonism, camptocormia and freezing. In particular, dystonia was limited to dystonic posturing of the fingers and painful dystonia of the toes. Due to those symptoms and increased anxiety as well as painful dystonia as well as unsuccessful treatment with evidence-based agents the patient was treated with dronabinol by his psychiatrist (capsules slowly up titrated to 20mg/day).
After two months of dronabinol treatment, the patient reported subjective improvement of the dystonic pain and a moderate improvement of freezing of gait as well as less falls. We examined the patient at two timepoints: after two months and after six months of dronabinol therapy. Importantly, the medication used at both timepoints remained stable, which excludes confounding contribution of other agents. Results of clinical assessments after two and six months of dronabinol administration are shown in Table 1. The baseline Unified Parkinson’s Disease Rating Scale and Unified Dystonia Rating Scale results cannot be provided as the data were not collected. Although the patient reported the subjective improvement of his symptoms, this was not confirmed in the neurological examination or in the UPDRS and UDRS assessments. Particularly, there was no minimal clinically important differences for UPDRS nor UDRS, although there was an improvement in sleep quality according to ESS. It can therefore be concluded that dronabinol had subjective analgesic and calming effect and, as a consequence, also improved sleep and general performance. Although he self-reported gait amelioration, it is not clear whether the patient exhibited any motor improvement. All in all, all positive effects were subjective and the final conclusion about the effectiveness of dronabinol cannot be reached.
Table 1. : Results of clinical assessments two and six months after therapy with dronabinol.
| Scale | Examination after two months | Examination after six months |
|---|---|---|
| UPDRS I | 0 | 0 |
| UPDRS II | 18 | 14 |
| UPDRS III | 26 | 24 |
| UPDRS IV | 0 | 0 |
| H-Y | 2.5 | 2.5 |
| Schwab and England | 80% | 90% |
| UDRS | 2 | 2 |
| PDSS-2 | 1 | 12 |
| ESS | 1 | 5 |
| BDI | 11 | 10 |
UPDRS, Unified Parkinson’s Disease Rating Scale; H-Y, Modified Hoehn and Yahr Staging; PDSS-2, Parkinson Disease Sleep Scale-2; UDRS, Unified Dystonia Rating Scale; ESS, Epworth Sleepiness Scale; BDI, Beck Depression Inventory.
Discussion
While there is some evidence that cannabis-based medicine (CBM) could improve both motor and non-motor symptoms in Parkinson’s disease (PD) 13, 14, the effectiveness of CBM in secondary parkinsonism as well as dystonia is unknown. Recently, Peball et al. 15 reported the potential efficacy of nabilone for PD patients with disturbing non-motor symptoms, which appears to be driven by positive effects on anxious mood and night-time sleep problems. Moreover, a number of other open label studies and case reports demonstrated efficacy of CBM in treatment of movement disorders 16– 18 . Small randomized trials in Tourette syndrome confirmed efficacy of tetrahydrocannabinol (THC) for tic reduction 19, 20. Therefore, CBM might be a useful therapeutic alternative for therapy resistant patients with movement disorders. However, systematic reviews and meta-analysis in this group of patients demonstrated conflicting results, due to methodological limitations of studies with CBM 21, 22.
In the case of our patient, his condition improved only subjectively, but this was not confirmed with objective neurological testing. Moreover, the use of cannabinoids in this case is controversial as the patient had a positive medical history for cannabis misuse. Additionally, long-term effectiveness should also be investigated with accuracy. Potential psychotic effects could be dangerous, therefore the dosage in our patient was slowly increased. Nevertheless, safety profile of CBM in movement disorders reported in previous studies was favorable, with the most common side effects being sedation, dizziness and sensation of “being high” 21, 22. Also, no baseline assessments, prior to dronabinol administration, were available. Finally, almost all previous reports regarding the application of CBM in movement disorders were limited to primary and not secondary disorders. As mentioned in the introduction, the pathophysiology of both disorders is totally different. In case of our patient the suspected mechanism is suspected to be vasospasm provoked by drug abuse that, in turn, provoked ischemia and, finally, abnormal pattern of movements. Results of international randomized, double-blind controlled trials with CBM in PD might offer more scientific rationales for discussion of potential usefulness of CBM in other movement disorders.
Data availability
All data underlying the results are available as part of the article and no additional source data are required.
Consent
Written informed consent for publication of their clinical details and clinical images was obtained from the patient.
References
- A Büttner. Review: The neuropathology of drug abuse.. Neuropathol Appl Neurobiol., 2011. [DOI | PubMed]
- A Büttner. The neuropathology of drug abuse.. Curr Opin Behav Sci., 2017. [DOI]
- S Martin-Schild, KC Albright, H Hallevi. Intracerebral hemorrhage in cocaine users.. Stroke., 2010. [DOI | PubMed]
- M Kojovic, I Pareés, P Kassavetis. Secondary and primary dystonia: pathophysiological differences.. Brain., 2013. [DOI | PubMed]
- AD Korczyn. Vascular parkinsonism–characteristics, pathogenesis and treatment.. Nat Rev Neurol., 2015. [DOI | PubMed]
- D Belvisi, R Pellicciari, A Fabbrini. Risk factors of Parkinson disease: Simultaneous assessment, interactions, and etiologic subtypes.. Neurology., 2020. [DOI | PubMed]
- SGM Vidal, A Hornik, C Morgan. Cocaine induced hippocampi infarction.. BMJ Case Rep., 2012. [DOI | PubMed]
- CM Farrell, DF Cucu. Cocaine-Related Acute Spinal Cord Infarction.. R I Med J (2013)., 2018. [PubMed]
- N Vila, A Chamorro. Ballistic movements due to ischemic infarcts after intravenous heroin overdose: report of two cases.. Clin Neurol Neurosurg., 1997. [DOI | PubMed]
- JM Lappin, S Darke, M Farrell. Stroke and methamphetamine use in young adults: a review.. J Neurol Neurosurg Psychiatry., 2017. [DOI | PubMed]
- J El Mesbahy, M Chraa, N Louhab. Hemorrhagic stroke after cannabis use in a young man.. Rev Neurol (Paris)., 2017. [DOI | PubMed]
- ST Ryste, BA Engelsen, H Naess. Codeine is associated with poor prognosis in acute stroke.. Brain Behav., 2017. [DOI | PubMed]
- Y Balash, L Bar-Lev Schleider, AD Korczyn. Medical Cannabis in Parkinson Disease: Real-Life Patients’ Experience.. Clin Neuropharmacol., 2017. [DOI | PubMed]
- FF Peres, AC Lima, JEC Hallak. Cannabidiol as a Promising Strategy to Treat and Prevent Movement Disorders?. Front Pharmacol., 2018. [DOI | PubMed]
- M Peball, F Krismer, HG Knaus. Non-Motor Symptoms in Parkinson’s Disease are Reduced by Nabilone.. Ann Neurol., 2020. [DOI | PubMed]
- MM Mascia, D Carmagnini, G Defazio. Cannabinoids and dystonia: an issue yet to be defined.. Neurol Sci., 2020. [DOI | PubMed]
- JH Kindred, K Li, NB Ketelhut. Cannabis use in people with Parkinson’s disease and Multiple Sclerosis: A web-based investigation.. Complement Ther Med., 2017. [DOI | PubMed]
- PF Whiting, RF Wolff, S Deshpande. Cannabinoids for Medical Use: A Systematic Review and Meta-analysis.. JAMA., 2015. [DOI | PubMed]
- KR Müller-Vahl, U Schneider, H Prevedel. Delta 9-tetrahydrocannabinol (THC) is effective in the treatment of tics in Tourette syndrome: a 6-week randomized trial.. J Clin Psychiatry., 2003. [DOI | PubMed]
- KR Müller-Vahl, U Schneider, A Koblenz. Treatment of Tourette’s syndrome with Delta 9-tetrahydrocannabinol (THC): a randomized crossover trial.. Pharmacopsychiatry., 2002. [DOI | PubMed]
- K Lim, YM See, J Lee. A Systematic Review of the Effectiveness of Medical Cannabis for Psychiatric, Movement and Neurodegenerative Disorders.. Clin Psychopharmacol Neurosci., 2017. [DOI | PubMed]
- AM Bougea, C Koros, A Simitsi. Medical cannabis as an alternative therapeutics for Parkinsons’ disease: Systematic review.. Complement Ther Clin Pract., 2020. [DOI | PubMed]
