Designer drugs: mechanism of action and adverse effects
Abstract
Electronic supplementary material:
The online version of this article (10.1007/s00204-020-02693-7) contains supplementary material, which is available to authorized users.
Article type: Review Article
Keywords: Designer drug, New psychoactive substance, Stimulant, Synthetic opioid, Synthetic cannabinoid, Psychedelic
Affiliations: grid.22937.3d0000 0000 9259 8492Center for Physiology and Pharmacology, Institute of Pharmacology, Medical University of Vienna, Währinger Strasse 13a, 1090 Vienna, Austria; grid.5329.d0000 0001 2348 4034Institute of Applied Physics, Vienna University of Technology, Getreidemarkt 9, 1060 Vienna, Austria; grid.410567.1Division of Clinical Pharmacology and Toxicology, University Hospital Basel and University of Basel, Schanzenstrasse 55, 4056 Basel, Switzerland
License: © The Author(s) 2020 CC BY 4.0 Open AccessThis article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
Article links: DOI: 10.1007/s00204-020-02693-7 | PubMed: 32249347 | PMC: PMC7225206
Relevance: Moderate: mentioned 3+ times in text
Full text: PDF (1.7 MB)
Introduction
The term “designer drugs” was originally introduced to describe novel substances that are derived from clandestine alterations of well-known drugs of abuse, preserving or enhancing pharmacologic effects while remaining outside of legal control (Jerrard ref. 1990). The term is currently applied more widely to include substances that originate from industrial or academic research but never receive medical approval. Some substances that are referred to as designer drugs may be medically approved in different countries, thus not fitting the classic definition of a designer drug (Bäckberg et al. ref. 2019; Manchester et al. ref. 2018; Owen et al. ref. 2016; Zawilska and Wojcieszak ref. 2019). The Internet plays a crucial role in the distribution of designer drugs and in the acquisition of information about them (Miliano et al. ref. 2018). The number of available designer drugs is constantly growing, and trends and patterns of use change over time. This poses a challenge to drug-regulatory authorities and can jeopardize public health. Designer drugs can generally be divided into the same categories as traditional drugs of abuse, namely stimulants, sedatives, dissociatives, cannabinoids, and psychedelics. However, in contrast to traditional drugs of abuse, newly emerging drugs can remain undetected by routine drug screening, and information about associated adverse effects is often scarce. Knowledge of the mechanism of action and potential clinical complications of designer drugs is key for healthcare workers who treat intoxicated patients. The present review provides an overview of the main mechanisms of action and adverse effects of currently available designer drugs.
Stimulants
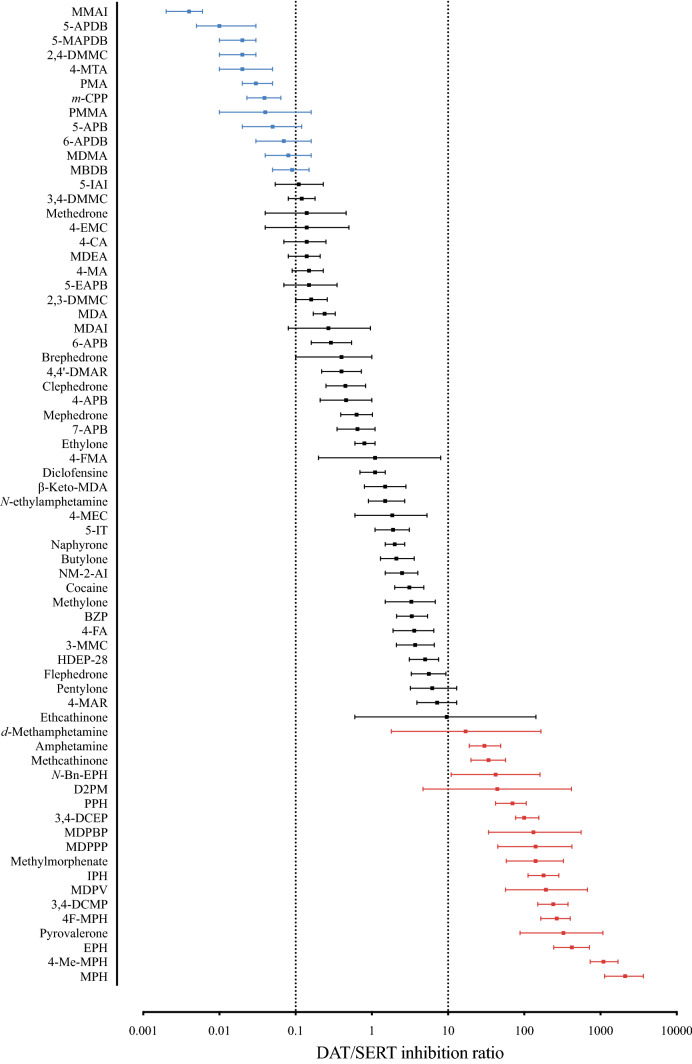
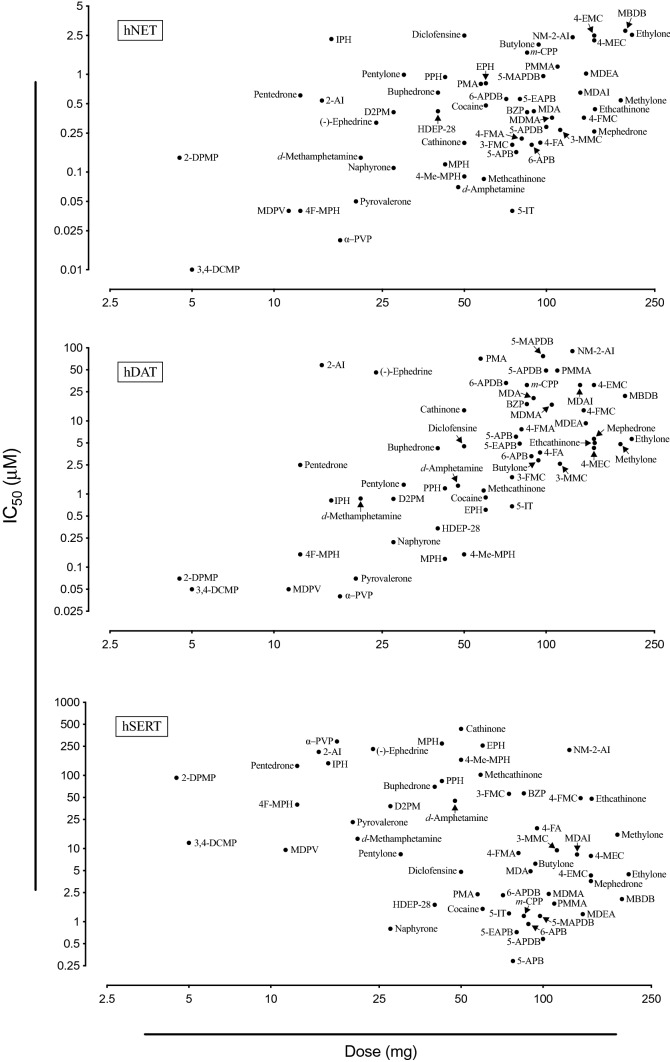
Monoaminergic stimulants, such as amphetamine, 3,4-methylenedioxymethamphetamine (MDMA), and cocaine, are among the most popular drugs of abuse. Other stimulants, such as methylphenidate and dextroamphetamine, are widely prescribed for the treatment of attention-deficit/hyperactivity disorder (ADHD). MDMA is currently being investigated as a prescription drug for the treatment of posttraumatic stress disorder (Amoroso and Workman ref. 2016; Mithoefer et al. ref. 2011, ref. 2016; Sharma and Couture ref. 2014). Stimulants modulate monoaminergic neurotransmission mainly by interacting with norepinephrine, dopamine, and serotonin (5-hydroxytryptamine [5-HT]) transporters (NET, DAT, and SERT, respectively), in addition to interacting with monoaminergic receptors and other targets. At monoamine transporters, monoaminergic stimulants act as either transporter inhibitors or substrates that mediate non-exocytotic monoamine efflux (Fleckenstein et al. ref. 2000; Rothman and Baumann ref. 2003; Sitte and Freissmuth ref. 2015). Different selectivity (Fig. 1) and potency (Fig. 2) at the different transporters result in different pharmacological effects, different clinical potencies (i.e., the dose that is necessary to induce a psychoactive effect), and different abuse liabilities (Aarde and Taffe ref. 2017; Gannon et al. ref. 2018; Javadi-Paydar et al. ref. 2018; Kuhar et al. ref. 1991; Luethi and Liechti ref. 2018; Ritz et al. ref. 1987; Vandewater et al. ref. 2015; Wee et al. ref. 2005; Wee and Woolverton ref. 2006). In rats, substances that are selective for DAT vs. SERT facilitate dose-dependent and abuse-related intracranial self-stimulation, indicating high abuse potential. In contrast, substances that are selective for the SERT vs. DAT depress dose-dependent intracranial self-stimulation (Suyama et al. ref. 2019), indicating a lower risk of abuse. Repeated exposure to substances with similar activity at the DAT and SERT may sustain the expression of DAT-mediated abuse-related effects while developing tolerance to SERT-mediated abuse-limiting effects, thus resulting in a higher abuse potential (Suyama et al. ref. 2019). The number of available designer stimulants is constantly increasing, and their use can cause various physiological complications and mood disturbances, which are discussed in the subsequent sections for the different classes of designer stimulants.
Amphetamines
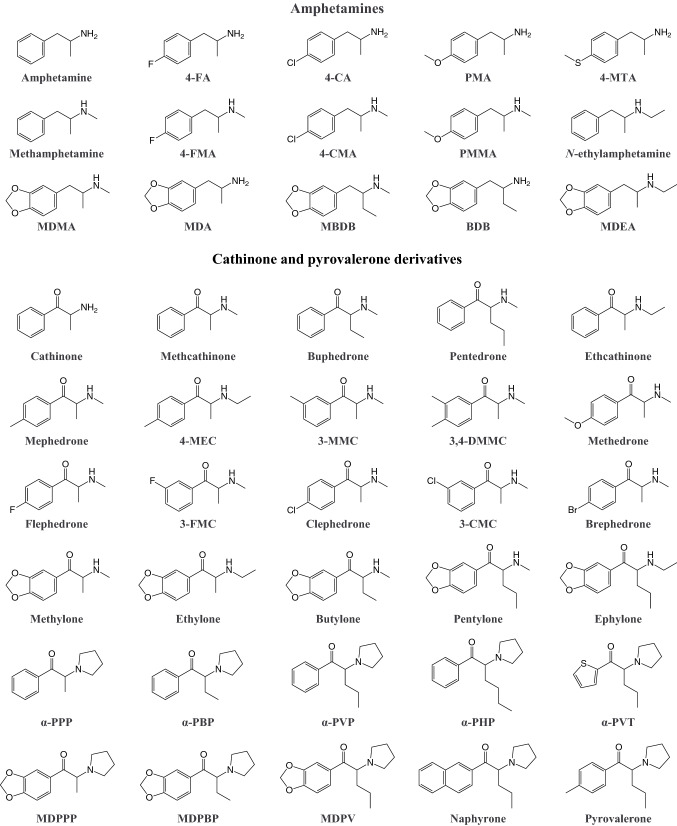
In addition to traditional amphetamines that are used both medically and recreationally, several amphetamine designer drugs without approved medical uses have become available. MDMA is by far the most popular amphetamine designer drug. It was first synthesized by Merck in 1912 as a precursor in a new chemical pathway, but it was not further investigated until many years later (Freudenmann et al. ref. 2006). In the 1980s, MDMA started to be used in psychotherapy and became popular as a recreational drug under the street name “ecstasy,” which led to a ban of MDMA in most countries soon afterward (Freudenmann et al. ref. 2006; Green et al. ref. 2003). MDMA has slowly found its way back into psychotherapy as a promising agent for the treatment of posttraumatic stress disorder (Amoroso and Workman ref. 2016; Mithoefer et al. ref. 2016, ref. 2011). Recently, various other, often ring-substituted amphetamine derivatives (Fig. 3) have gained increasing popularity as designer drugs, many of which were initially legally obtainable.
Mechanism of action of amphetamines
Most amphetamines are substrate-type monoamine releasers (Rothman and Baumann ref. 2003; Simmler et al. ref. 2013, ref. 2014a; Sitte and Freissmuth ref. 2015). In addition to potent effects at the NET, many amphetamines predominantly act at the DAT vs. SERT, resulting in greater reinforcing effects and higher abuse liability (Kuhar et al. ref. 1991; Ritz et al. ref. 1987; Wee et al. ref. 2005; Wee and Woolverton ref. 2006). In contrast, some amphetamines, including MDMA, have more pronounced effects at the SERT vs. DAT, resulting in an entactogenic effect profile and lower abuse liability (Baumann et al. ref. 2000, ref. 2012; Luethi et al. ref. 2019a; Simmler et al. ref. 2013). Para-substitution at the phenyl ring of amphetamines has been shown to shift their pharmacological profile toward more pronounced activity at the SERT vs. DAT (Luethi et al. ref. 2018c, ref. 2019b; Rickli et al. ref. 2015a; Simmler et al. ref. 2014a; Wee et al. ref. 2005). In addition to their interactions with plasma membrane transporters, amphetamines are substrates at vesicular monoamine transporters (VMATs) and inhibit monoamine oxidases (Fleckenstein et al. ref. 2007; Partilla et al. ref. 2006; Sitte and Freissmuth ref. 2015; Volz et al. ref. 2007). Furthermore, amphetamine designer drugs have been reported to interact with various monoaminergic receptors, including serotonergic and adrenergic receptors, and trace amine-associated receptor 1 (TAAR1), which negatively modulates monoaminergic neurotransmission (Di Cara et al. ref. 2011; Rickli et al. ref. 2015a; Simmler et al. ref. 2014a, ref. 2016).
Adverse effects of amphetamines
Numerous studies have reported the adverse effects of amphetamine, lisdexamfetamine, and methamphetamine. Among amphetamine-derived designer drugs, MDMA is the best studied. For traditional amphetamines, mainly sympathomimetic adverse effects (e.g., anxiety, insomnia, headaches, mydriasis, bruxism, dry mouth, hyperthermia, hypertension, tachycardia, chest pain, palpitations, anorexia, nausea, vomiting, and abdominal pain) can be expected for newly emerged amphetamine-derived designer drugs (Carvalho et al. ref. 2012; Derlet et al. ref. 1989; Dolder et al. ref. 2017; Heal et al. ref. 2013; Vizeli and Liechti ref. 2017; Wijers et al. ref. 2017). Hyperthermia is a significant contributor to potentially severe adverse effects of amphetamines, including disseminated intravascular coagulation, renal failure, and rhabdomyolysis (Bingham et al. ref. 1998; Carvalho et al. ref. 2012; Cunningham ref. 1997; Fahal et al. ref. 1992; Ginsberg et al. ref. 1970; Greene et al. ref. 2003; Halachanova et al. ref. 2001; Henry et al. ref. 1992; Kendrick et al. ref. 1977; Richards et al. ref. 1999; Screaton et al. ref. 1992; Vanden Eede et al. 2012). The uncoupling of oxidative phosphorylation in skeletal muscle through the activation of uncoupling protein 3 (UCP-3) and agonism at adrenergic receptors by norepinephrine release has previously been identified as an important contributor to MDMA-induced hyperthermia (Mills et al. ref. 2003, ref. 2004). Many adverse effects are similar for most amphetamines, but the prevalence of some events is higher for certain specific amphetamines. A comparison of the structures and pharmacological profiles of newly emerged amphetamine designer drugs with well-studied amphetamine derivatives helps to shed light on the likelihood of these specific adverse events. Hepatotoxicity is a potentially fatal adverse effect that has been associated with the use of amphetamines, and MDMA is the designer drug that has been most frequently linked to liver injury (Andreu et al. ref. 1998; De Carlis et al. ref. 2001; Ellis et al. ref. 1996; Garbino et al. ref. 2001; Jones et al. ref. 1994; Kamijo et al. ref. 2002). Different mechanisms may contribute to MDMA-induced hepatotoxicity, including monoamine release, hyperthermia, oxidative stress, impairments in the antioxidant response, mitochondrial dysfunction, and the formation of catechol metabolites by demethylenation (Carvalho et al. ref. 2010, ref. 2012). Cardiotoxicity is another potential complication of amphetamine use and largely attributable to sympathomimetic activation and additionally to secondary mechanisms, such as metabolic bioactivation and hyperthermia (Carvalho et al. ref. 2012). The activation of 5-HT2B receptors in cardiovascular tissues may potentially result in cardiac valvulopathy and is thus a concern for drugs that increase plasma 5-HT levels or directly activate 5-HT2B receptors (Elangbam ref. 2010; Elangbam et al. ref. 2008; Huang et al. ref. 2009; Roth ref. 2007). Mild-to-moderate valvular heart disease has been observed in a population of heavy recreational MDMA users, and the 5-HT2B receptor-mediated proliferation of cardiac valvular interstitial cells that was induced by MDMA was demonstrated in vitro (Droogmans et al. ref. 2007; Setola et al. ref. 2003). The MDMA metabolite 4-hydroxy-3-methoxymethamphetamine (HMMA) exhibits higher potency in stimulating vasopressin secretion; together with the excessive intake of hypotonic liquids and hyperthermia, it may cause potentially fatal hyponatremia, especially in female users likely because of effects of estrogen on vasopressin (Campbell and Rosner ref. 2008; Fallon et al. ref. 2002; Farah and Farah ref. 2008; Forsling et al. ref. 2001; Forsling et al. ref. 2002; Ghatol and Kazory ref. 2012; Hartung et al. ref. 2002; Moritz et al. ref. 2013; Rosenson et al. ref. 2007; Simmler et al. ref. 2011; Van Dijken et al. ref. 2013). Monoamine depletion and reactive species contribute to the neurotoxicity of amphetamines (Carvalho et al. ref. 2012). However, despite extensive research, the extent to which different amphetamines are neurotoxic remains largely unknown. Compared with amphetamine, an increase in serotonergic toxicity has been reported for the para-chlorinated derivative 4-chloroamphetamine, likely explained by highly potent serotonergic activity coupled with considerably potent dopaminergic activity (Colado et al. ref. 1993; Fuller ref. 1992; Johnson et al. ref. 1990; Luethi et al. ref. 2019b; Miller et al. ref. 1986). However, unlike other halogenated stimulants, such as 4-fluoroamphetamine, 4-chloroamphetamine never achieved popularity as a designer drug, possibly because of its well-documented neurotoxicity. Nevertheless, the widely used 4-fluoroamphetamine has been associated with various mild-to-moderate adverse effects (e.g., agitation, severe headache, anxiety, confusion, tachypnea, hypertension, tachycardia, chest pain, electrocardiographic abnormalities, and nausea) and severe adverse effects (e.g., coma, convulsions, cerebral hemorrhage, inverted takotsubo cardiomyopathy, myocardial infarction, and fatalities following cardiac arrest) (Hondebrink et al. ref. 2018). A detailed review of amphetamine toxicity, including toxicological pathways that involve the formation of reactive species, the depletion of antioxidants, and microglial activation, was previously published (Carvalho et al. ref. 2012).
Cathinone and pyrovalerone derivatives
Cathinone designer drugs are derivatives of the β-keto-amphetamine cathinone, an alkaloid that is found in the leaves of the Catha edulis plant. The large-scale recreational use of synthetic cathinones is a relatively new phenomenon, although several compounds have been known for a long time. For example, the first synthesis of 4-methylmethcathinone (mephedrone) was published in 1929 (Sanchez ref. 1929). Several other synthetic cathinones have been investigated for their medical potential, mostly as antidepressant or anorectic agents, but only a few were ever marketed because of concerns about abuse (Canning et al. ref. 1979; Cunningham ref. 1963; Dal Cason et al. ref. 1997; Seaton et al. ref. 1961; Soroko et al. ref. 1977; Valente et al. ref. 2014). Pyrovalerone derivatives represent a subgroup of synthetic cathinones based on the structure of pyrovalerone, which was developed in the 1960s as a treatment option for lethargy, fatigue, and obesity (Gardos and Cole ref. 1971). As a result of their initial misleading marketing as “bath salts”, synthetic cathinones are still often referred to by that term (Baumann et al. ref. 2013). Currently, synthetic cathinones (Fig. 3) represent the largest group of designer stimulants that are monitored by the European Monitoring Center for Drugs and Drug Addiction (EMCDDA) (European Monitoring Centre for Drugs and Drug Addiction ref. 2019).
Mechanism of action of cathinone and pyrovalerone derivatives
Similar to other monoaminergic stimulants, the psychoactive effects of synthetic cathinones are primarily mediated by interactions with monoamine transporters. Many cathinones are partially or fully effective substrate-type releasers at one or several monoamine transporters, but some compounds, such as pyrovalerone derivatives, are transporter inhibitors (Baumann et al. ref. 2012; Eshleman et al. ref. 2013, ref. 2017; Luethi et al. ref. 2018c; Mayer et al. ref. 2016,ref. 2019a; Niello et al. ref. 2019; Rickli et al. ref. 2015a; Simmler et al. ref. 2013). Mephedrone has additionally been shown to mediate monoamine release via organic cation transporter 3 (OCT3), indicating that cathinones target both high-affinity and low-affinity/high-capacity transporters (Mayer et al. ref. 2019b). Similar to amphetamines, cathinone designer drugs also interact with several adrenergic and serotonergic receptors (Luethi et al. ref. 2018c; Rickli et al. ref. 2015a; Simmler et al. ref. 2014a). Compared with amphetamines, however, cathinone designer drugs have been shown to interact less potently with TAAR1 and VMAT2 (Eshleman et al. ref. 2013; Simmler et al. ref. 2016). These less potent interactions at TAAR1 may result in a higher risk of cathinone dependence compared with amphetamines.
Adverse effects of cathinone and pyrovalerone derivatives
The use of synthetic cathinones has been associated with mainly sympathomimetic toxicity, which may manifest as agitation, tachycardia, hypertension and less frequently as lower levels of consciousness, hallucinations, hyponatremia, chest pain, palpitations, and nausea (Bäckberg et al. ref. 2015c; Beck et al. ref. 2015, ref. 2016; Borek and Holstege ref. 2012; Boulanger-Gobeil et al. ref. 2012; Franzén et al. ref. 2018; James et al. ref. 2011; Ross et al. ref. 2011, ref. 2012; Umebachi et al. ref. 2016; Wood et al. ref. 2010). Rarely, severe adverse effects (e.g., seizures, significant peripheral organ damage, and rhabdomyolysis) have been reported (Bäckberg et al. ref. 2015c; Beck et al. ref. 2015, ref. 2016; Borek and Holstege ref. 2012; Boulanger-Gobeil et al. ref. 2012; Franzén et al. ref. 2018; Fröhlich et al. ref. 2011; Penders et al. ref. 2012; Ross et al. ref. 2011, ref. 2012). In vitro studies in neuronal, skeletal muscle, and hepatic cells indicated various cytotoxic mechanisms of synthetic cathinones, including mitochondrial dysfunction, glutathione depletion, oxidative stress, and apoptosis pathway activation, which are aggravated under hyperthermic conditions (Dias da Silva et al. ref. 2019; Luethi et al. ref. 2017, ref. 2019b; Valente et al. ref. 2016a, ref. b, ref. 2017a, ref. b; Zhou et al. ref. 2019). Unclear, however, is the extent to which these mechanisms contribute to clinical adverse effects of cathinones relative to sympathomimetic toxicity. Numerous cathinone-related fatalities have been reported (Adamowicz et al. ref. 2014, ref. 2016; Bäckberg et al. ref. 2015c; Barrios et al. ref. 2016; Beck et al. ref. 2016; Busardò et al. ref. 2015; Carbone et al. ref. 2013; DeRoux and Dunn ref. 2017; Eiden et al. ref. 2013; Forrester ref. 2012b; Kesha et al. ref. 2013; Kudo et al. ref. 2015; Lee et al. ref. 2015; Liveri et al. ref. 2016; Majchrzak et al. ref. 2018; Marinetti and Antonides ref. 2013; Maskell et al. ref. 2011a; Nagai et al. ref. 2014; Pearson et al. ref. 2012; Pieprzyca et al. ref. 2018; Potocka-Banas et al. ref. 2017; Schifano et al. ref. 2012; Sellors et al. ref. 2014; Thirakul et al. ref. 2017; Umebachi et al. ref. 2016; Wood et al. ref. 2010; Wright et al. ref. 2013; Wyman et al. ref. 2013; Zaami et al. ref. 2018). Analytically confirmed cases of cathinone-related deaths were mainly attributed to hyperthermia, hypertension, cardiac arrest, and serotonin syndrome (Busardò et al. ref. 2015; Zaami et al. ref. 2018).
Benzofuran and indole derivatives
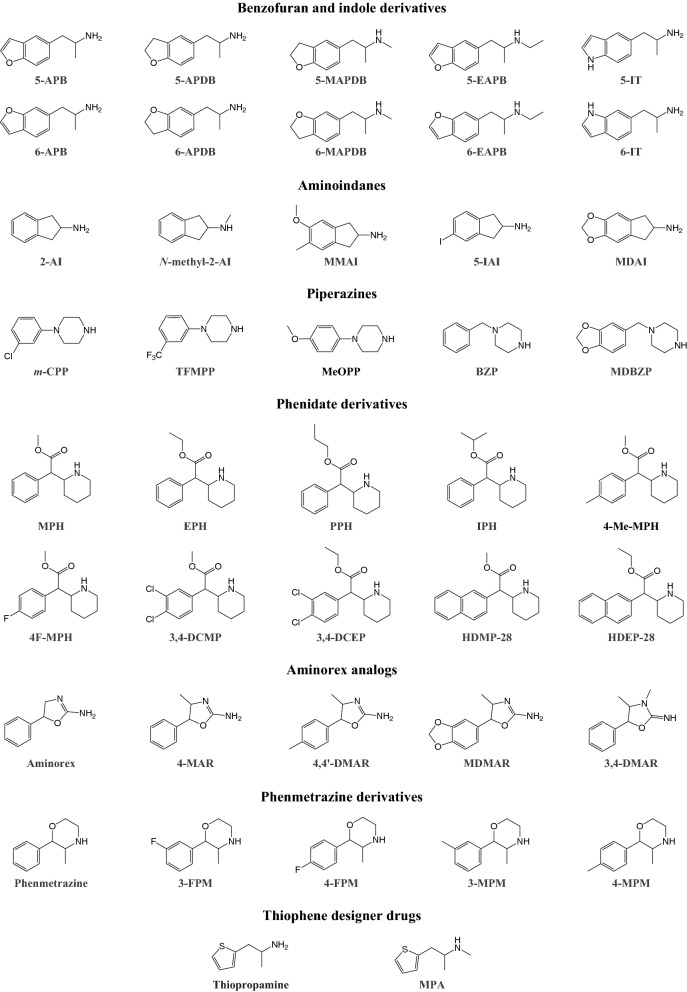
Various analogs of MDMA and its metabolite 3,4-methylenedioxyamphetamine (MDA) have become available as designer drugs, in which a dihydrobenzofuran, benzofuran, or indole group replaces the benzodioxole group (Fig. 4). Some benzofuran designer drugs were originally investigated as part of a study that examined the role of ring oxygen atoms in interactions between MDA and monoamine transporters (Monte et al. ref. 1993). The indole designer drugs 5-(2-aminopropyl)indole (5-IT, 5-API) and 6-(2-aminopropyl)indole (6-IT, 6-API) emerged from industrial research and are positional isomers of the psychedelic tryptamine α-methyltryptamine (αMT) (Hofmann and Troxler ref. 1962).
Mechanism of action of benzofuran and indole derivatives
In addition to norepinephrine uptake inhibition, stimulant benzofuran and dihydrobenzofuran designer drugs have moderate-to-high selectivity in inhibiting 5-HT vs. dopamine uptake, often with substrate activity at the transporters (Monte et al. ref. 1993; Rickli et al. ref. 2015b). Furthermore, affinity at adrenergic, serotonergic, and histaminergic receptors, partial agonism at 5-HT2A receptors, and partial to full agonism at 5-HT2B receptors have been reported for these designer drugs (Dawson et al. ref. 2014; Iversen et al. ref. 2013; Rickli et al. ref. 2015b). The indoles 5-IT and 6-IT are potent substrates at the NET, DAT, and SERT in rat synaptosomes (Marusich et al. ref. 2016). The position of the alkylamine side chain is determining of DAT vs. SERT selectivity, with 5-IT having significantly (eightfold) more potent monoamine-releasing actions at the DAT vs. SERT in rat synaptosomes, whereas 6-IT is eightfold more selective for the SERT (Marusich et al. ref. 2016). In human transporter-transfected cells, 5-IT has been shown to be a very potent inhibiter of norepinephrine uptake, but it did not significantly induce norepinephrine efflux at a single high concentration. However, it had substrate activity at the DAT and SERT (Luethi et al. ref. 2018c). Additionally, 5-IT has affinity for adrenergic and serotonergic receptors and partially activates 5-HT2A and 5-HT2B receptors, which may result in additional perceptual psychedelic-like effects at high doses (Luethi et al. ref. 2018c). Furthermore, 5-IT is an inhibitor of human monoamine oxidase (MAO)-A (Herraiz and Brandt ref. 2014).
Adverse effects of benzofuran and indole derivatives
Benzofuran designer drugs may cause agitation, insomnia, headache, drowsiness, dry mouth, dry eyes, bruxism, hyperthermia, tachycardia, palpitations, nausea, diarrhea, hot flashes, clonus of the hands and feet, and psychological symptoms, including visual and auditory hallucinations, depression, anxiety, panic attacks, paranoia, and psychosis (Jebadurai et al. ref. 2013; Nugteren-van Lonkhuyzen et al. ref. 2015). A case of drug-induced psychosis with symptoms of self-harm, paranoia, and suicidal thoughts but unremarkable physical examination was reported with the analytically confirmed presence of 6-(2-aminopropyl)benzofuran (6-APB) in combination with metabolites of a synthetic cannabinoid and tetrahydrocannabinol (Chan et al. ref. 2013). In addition to fatal intoxications that involve benzofurans combined with other designer drugs (Adamowicz et al. ref. 2014; Elliott and Evans ref. 2014), benzofuran toxicity was implicated as the cause of death in an accidental intoxication, in which 5-APB and presumptively a smaller amount of 5-(2-Aminopropyl)-2,3-dihydrobenzofuran (5-APDB) were detected as sole compounds in addition to alcohol (McIntyre et al. ref. 2015a). Autopsy revealed white foam in the trachea, marked congestion and edema of the lungs, and congestive splenomegaly (McIntyre et al. ref. 2015a). Benzofurans induce oxidative stress, disrupt mitochondrial function, and activate apoptosis cascades in vitro, but the in vivo relevance of these sequelae remain unclear (Roque Bravo et al. ref. 2019). 5-IT has been linked to various sympathomimetic adverse effects, including extreme agitation, anxiety, confusion, insomnia, restlessness, hallucinations, seizures, tremors, dilated pupils without light reaction, hyperthermia, sweating, hypertension, tachycardia, arrhythmias, renal failure, myoclonus, muscle rigidity, rhabdomyolysis, and in some cases, serotonergic toxicity (Bäckberg et al. ref. 2014; Coppola and Mondola ref. 2013b; Katselou et al. ref. 2015). Furthermore, 5-IT was involved in several intoxication cases with a fatal outcome within a time span of only a few months (Katselou et al. ref. 2015; Kronstrand et al. ref. 2013; Seetohul and Pounder ref. 2013). Many of 5-IT-associated deaths have been attributed to cardiac arrest, to which 5-HT2B receptor activation by 5-IT may have contributed (Katselou et al. ref. 2015; Luethi et al. ref. 2018c; Seetohul and Pounder ref. 2013). In most of the fatal and non-fatal intoxication cases, additional substances have been detected. In some cases, the users reported to be unaware that they took 5-IT, because the products were mislabeled as 6-APB (Bäckberg et al. ref. 2014; Kronstrand et al. ref. 2013; Seetohul and Pounder ref. 2013). Although the reported doses of 5-IT and 6-APB are similar, they differ in their selectivity for the dopaminergic vs. serotonergic system (Luethi et al. ref. 2018c; Luethi and Liechti ref. 2018; Rickli et al. ref. 2015b). The extent to which mislabeling played a role in 5-IT intoxication remains unclear.
Aminoindanes
Aminoindane designer drugs (Fig. 4) have become widely available when first-generation designer stimulants, including mephedrone, were finally placed under legal control (Pinterova et al. ref. 2017; Sainsbury et al. ref. 2011). Aminoindanes are conformationally restricted analogs of amphetamine that were originally investigated as bronchodilatory, analgesic, and anti-Parkinson agents, and subsequently as drugs with psychotherapeutic value (Pinterova et al. ref. 2017; Solomons and Sam ref. 1973). Some aminoindane designer drugs have been reported to be entactogens with lower serotonergic neurotoxicity relative to non-aminoindane entactogens (Johnson et al. ref. 1990; Nichols et al. ref. 1991). The desired psychoactive effects of aminoindane designer drugs include euphoria, the mild distortion of vision, time, and space, a greater intensity of perceptions and colors, empathy, and arousal (Coppola and Mondola ref. 2013a; Corkery et al. ref. 2013).
Mechanism of action of aminoindanes
Similar to amphetamines, aminoindane designer drugs are monoamine transporter substrates, with relevant affinity for adrenergic, dopaminergic, and serotonergic receptors (Iversen et al. ref. 2013; Luethi et al. ref. 2018c; Simmler et al. ref. 2014b). Ring-substituted aminoindanes, such as 5,6-methylenedioxy-2-aminoindane (MDAI), 5-iodoaminoindane (5-IAI), and 5-methoxy-6-methyl-2-aminoindane (MMAI), are selective for the SERT vs. DAT (Luethi et al. ref. 2018c; Simmler et al. ref. 2014b). Potent actions of MDAI and 5-IAI on the NET result in an in vitro pharmacological profile that is similar to MDMA, suggesting similar entactogenic effects (Simmler et al. ref. 2014b). MMAI acts as a selective 5-HT releaser with less pronounced effects on the NET, indicating that its effects are different from typical entactogens, such as MDMA (Luethi et al. ref. 2018c). According to in vitro studies, the non-ring-substituted aminoindanes 2-aminoindane (2-AI) and N-methyl-2-AI are selective norepinephrine releasers and devoid of pharmacologically relevant DAT or SERT interactions (Luethi et al. ref. 2018c; Simmler et al. ref. 2014b).
Adverse effects of aminoindanes
Self-reported undesirable effects of aminoindane designer drugs include agitation, anxiety, panic attacks, headache, insomnia, hallucinations, and tachycardia (Coppola and Mondola ref. 2013a). Three fatal cases were reported with confirmed MDAI intake, and serotonin syndrome could have been a factor that contributed to death (Corkery et al. ref. 2013). The likelihood of the serotonergic toxicity of aminoindanes in humans has not been investigated, but signs of serotonin syndrome were reported for a high dose of MDAI in rats (Palenicek et al. ref. 2016).
Piperazines
Piperazine designer drugs (Fig. 4) have been widely sold as legal party pills or powders and appeared as pure substances or adulterants in pills that are sold as “ecstasy” because of their somewhat MDMA-like pharmacological profile, alone or combined (Baumann et al. ref. 2005; Bossong et al. ref. 2010; Lin et al. ref. 2011; Sheridan et al. ref. 2007; Wood et al. ref. 2008). Various therapeutic drugs have a piperazine moiety, and some piperazine designer drugs have a history of medical use. For example, 1-benzylpiperazine (BZP) has been investigated as an antihelmintic agent and antidepressant, and meta-chlorophenylpiperazine (m-CPP) is an active metabolite of different antidepressants (Arbo et al. ref. 2012; Schep et al. ref. 2011). Other frequently used piperazine designer drugs include trifluoromethylphenylpiperazine (TFMPP), 1-(3,4-methylenedioxybenzyl)piperazine (MDBZP), and 4-methoxyphenylpiperazine (MeOPP).
Mechanism of action of piperazines
Piperazine designer drugs exert mixed effects at monoamine transporters. TFMPP and m-CPP are selective 5-HT vs. dopamine reuptake inhibitors (DAT/SERT ratio < 0.05), and m-CPP also inhibits norepinephrine uptake with potency that is similar to the inhibition of 5-HT uptake (Simmler et al. ref. 2014b). Both substances bind to several serotonergic, adrenergic, dopaminergic, and histaminergic receptors with submicromolar or low micromolar affinity (Simmler et al. ref. 2014b). In contrast, BZP is a selective NET inhibitor with relatively weak inhibition of dopamine and 5-HT uptake, without any potent affinity at monoamine receptors (Simmler et al. ref. 2014b). BZP was also shown to be a DAT substrate in rat synaptosomes and human DAT-transfected cells, and m-CPP was reported to elicit 5-HT efflux in human SERT-transfected cells (Baumann et al. ref. 2005; Simmler et al. ref. 2014b). TFMPP mediated 5-HT efflux in rat synaptosomes but not in transfected cells at a single high concentration of 100 μM (Baumann et al. ref. 2005; Simmler et al. ref. 2014b). A combination of TFMPP and BZP was reported to closely mimic the effects of MDMA in rats (Baumann et al. ref. 2005).
Adverse effects of piperazines
Adverse effects of piperazine designer drugs are mostly sympathomimetic, including agitation, insomnia, headaches, dizziness, dilated pupils, hyperthermia, tachycardia, nausea, urine retention, and inducible clonus (Arbo et al. ref. 2012; Gee et al. ref. 2005, ref. 2008, ref. 2010; Katz et al. ref. 2016a; Kovaleva et al. ref. 2008; Schep et al. ref. 2011; Wilkins et al. ref. 2008; Wood et al. ref. 2008). In addition to sympathomimetic toxicity, dissociative symptoms, visual and auditory hallucinations, and psychological symptoms (e.g., short temper, confusion, anxiety, depression, and paranoia) have been associated with the use of piperazine designer drugs (Gee et al. ref. 2008; Kovaleva et al. ref. 2008; Schep et al. ref. 2011; Wilkins et al. ref. 2008; Wood et al. ref. 2008). Furthermore, toxic seizures were frequently observed in patients who were admitted to the emergency department after the use of BZP-containing party pills. Although there seems to be a trend toward higher concentrations being more frequently associated with seizures, they may also occur at low doses (Gee et al. ref. 2005, ref. 2008). Other severe adverse effects of BZP include hyponatremia, severe combined metabolic and respiratory acidosis, hepatic injury, renal failure, disseminated intravascular coagulation, and rhabdomyolysis (Gee et al. ref. 2010; Katz et al. ref. 2016a). A case of severe hyperthermia with resultant multi-organ failure and a case of hyponatremia that led to fatal brain edema were reported for the concomitant use of piperazine designer drugs and MDMA (Balmelli et al. ref. 2001; Gee et al. ref. 2010). The contribution of these individual compounds to the observed clinical manifestations remains unclear, but piperazines and MDMA may elicit additive or synergistic toxicity. In vitro, piperazine designer drugs have been reported to upregulate key enzymes of cholesterol biosynthesis, induce oxidative stress, disrupt mitochondrial function, and activate apoptosis pathways, all of which may potentially contribute to clinical toxicity (Arbo et al. ref. 2016a, ref. b; Dias da Silva et al. ref. 2017; Dias-da-Silva et al. ref. 2015; Majrashi et al. ref. 2018).
Phenidate derivatives
Derivatives of the piperidine prescription drug methylphenidate have appeared as designer drugs (Fig. 4), with substitutions at the phenyl ring and different lengths of the carbon side chain (Luethi et al. ref. 2018b). Similar to methylphenidate, phenidate derivatives may be used to induce euphoria or as cognitive enhancers (Ho et al. ref. 2015; Lüthi and Liechti ref. 2019). Various methylphenidate-based designer drugs originated from drug development efforts and later appeared on the recreational drug market as pure compounds or in the form of branded products (Bailey et al. ref. 2015; Deutsch et al. ref. 1996; Ho et al. ref. 2015; Markowitz et al. ref. 2013; Misra et al. ref. 2010). When insufflated, the pharmacological and subjective-effect profile of methylphenidate is similar to cocaine, and phenidate derivatives may, therefore, be used as substitutes for cocaine (Vogel et al. ref. 2016).
Mechanism of action of phenidate derivatives
Similar to methylphenidate, methylphenidate-based designer drugs act as potent NET and DAT inhibitors that are devoid of substrate activity (Luethi et al. ref. 2018b; Simmler et al. ref. 2014b). Some less potent interactions with the SERT and adrenergic and serotonergic receptors have been reported but are not likely to play a relevant role in the psychoactive actions of most phenidate derivatives (Luethi et al. ref. 2018b).
Adverse effects of phenidate derivatives
Adverse effects of phenidate derivatives are similar to amphetamines and include agitation, anxiety, hypertension, tachycardia, and palpitations (Bailey et al. ref. 2015). Because of their relatively slow onset of action when taken orally, the nasal insufflation or injection of phenidate derivatives is common, especially in heavy users. Nasal pain and septum perforations after insufflation and infections after intravenous injection may occur (Ho et al. ref. 2015; Lafferty et al. ref. 2016; Parks et al. ref. 2015). The rapid onset of action after nasal or intravenous use, combined with the marked DAT vs. SERT selectivity of phenidate derivatives, has been linked to a higher risk of addiction (Luethi et al. ref. 2018b). In several cases, phenidate derivatives have been analytically confirmed post-mortem, in which ethylphenidate is the most frequently detected compound (Krueger et al. ref. 2014; Maskell et al. ref. 2016; Parks et al. ref. 2015; Shoff et al. ref. 2019). Many decedents had a history of heroin use, and intravenous injection was a common route of administration. In addition to phenidate derivatives, other drugs, including benzodiazepines and opioids, have been detected in most fatal cases (Krueger et al. ref. 2014; Maskell et al. ref. 2016; Parks et al. ref. 2015).
Aminorex analogs
Various analogs of the anorectic agent aminorex have become available as designer drugs (Fig. 4). Aminorex was first marketed as an over-the-counter appetite suppressant in parts of Europe in the 1960s, but it was withdrawn a few years later because of an epidemic of chronic pulmonary hypertension that was associated with many fatalities (Maier et al. ref. 2018a). Aminorex analogs that have found their way onto the designer drug market include 4-methylaminorex (4-MAR) and 4,4′-dimethylaminorex (4,4′-DMAR), the reported effects of which include euphoria, mental and physical stimulation, sociability, empathy, arousal, and changes in visual perception (European Monitoring Centre for Drugs and Drug Addiction ref. 2015; Glanville et al. ref. 2015; Loi et al. ref. 2017). A comprehensive review of the history of aminorex use and the emergence of its designer drug analogs was recently published (Maier et al. ref. 2018a).
Mechanism of action of aminorex analogs
In human transporter-transfected cells, 4,4′-DMAR is a potent inhibitor of norepinephrine, dopamine, and 5-HT reuptake. 4-MAR has similarly potent dopamine and norepinephrine reuptake properties as 4,4′-DMAR, but 5-HT uptake inhibition is less pronounced compared with its para-methylated counterpart (Maier et al. ref. 2018b; Rickli et al. ref. 2019). Aminorex and its derivative 4-MAR mediate norepinephrine and dopamine efflux in rat synaptosomes, with weak substrate activity at the SERT (Brandt et al. ref. 2014; Rothman et al. ref. 2001). 4,4′-DMAR and 3′,4′-methylenedioxy-4-methylaminorex (MDMAR) induce norepinephrine, dopamine, and 5-HT efflux in rat synaptosomes (Brandt et al. ref. 2014; McLaughlin et al. ref. 2015). Dynamic superfusion experiments revealed the substrate activity of 4,4′-DMAR at human monoamine transporters (Maier et al. ref. 2018b). In human transporter-transfected cells that were preloaded with monoamines and exposed to drugs at a single high concentration (100 μM), only dopamine efflux was observed for 4,4′-DMAR, and dopamine and 5-HT efflux was observed for 4-MAR (Rickli et al. ref. 2019). In addition to interactions with plasmalemmal transporters, 4,4′-DMAR has been shown to inhibit human VMAT2-mediated dopamine uptake (Maier et al. ref. 2018b). In addition to their primary effects on transporters, minor interactions with serotonergic 5-HT2C and adrenergic α2A receptors have been described for 4-MAR, and low affinity at 5-HT2A and 5-HT2C receptors has been described for 4,4′-DMAR (Maier et al. ref. 2018b; Rickli et al. ref. 2019).
Adverse effects of aminorex analogs
Adverse effects of aminorex designer drugs that have been reported by users on various Internet discussion platforms include agitation, dysphoria, insomnia, amnesia, panic attacks, psychosis, hallucinations, facial spasms, dilated pupils, foaming at the mouth, dry mouth, jaw clenching, elevations of body temperature, sweating, elevations of heart rate, nausea, and restless legs (Glanville et al. ref. 2015; Loi et al. ref. 2017; Maier et al. ref. 2018a). Pulmonary hypertension (i.e., the adverse effect that led to the removal of aminorex from the market) has been associated with the recreational use of 4-MAR (Gaine et al. ref. 2000). Designer drug analogs of aminorex have been analytically confirmed in several drug-related deaths (Cosbey et al. ref. 2014; Davis and Brewster ref. 1988; European Monitoring Centre for Drugs and Drug Addiction ref. 2015). Although other substances were present in most fatal cases, 4,4′-DMAR was mentioned to be the cause of death or to have played a contributory role in several of these fatalities (European Monitoring Centre for Drugs and Drug Addiction ref. 2015). Brain edema, seizures, hyperthermia, respiratory and cardiac arrest, and internal bleeding were all listed as adverse events or autopsy findings that were associated with the use of 4,4′-DMAR (European Monitoring Centre for Drugs and Drug Addiction ref. 2015).
Phenmetrazine derivatives
Phenmetrazine is a reinforcing stimulant, which was previously used as an appetite suppressant before it was eventually withdrawn from the market (Chait et al. ref. 1987). Phenmetrazine-derived designer drugs (Fig. 4) represent a relatively understudied class of drugs, among which 3-fluorophenmetrazine (3-FPM) use appears to be the most widespread.
Mechanism of action of phenmetrazine derivatives
Like the parent compound, ring-fluorinated derivatives of phenmetrazine are substrates at the NET and DAT, with minor substrate activity at the SERT (Mayer et al. ref. 2018; Rothman et al. ref. 2002). Ring-methylated phenmetrazine derivatives were reported to have greater potency at the SERT, in addition to activity at the NET and DAT (McLaughlin et al. ref. 2018). Para-substituted compounds were shown to have the greatest serotonergic effects among the phenmetrazine derivatives, similar to ring-substituted amphetamine and cathinone designer drugs (Luethi et al. ref. 2019b; Rickli et al. ref. 2015a).
Adverse effects of phenmetrazine derivatives
Based on their mechanism of action, phenmetrazine designer drugs are expected to elicit stimulatory toxicity that is similar to amphetamines. A series of non-fatal intoxications that involved 3-FPM were reported within the Swedish STRIDA project, mostly with sympathomimetic adverse effects (Bäckberg et al. ref. 2016). However, polydrug intoxication prevented attribution of the observed effects to 3-FPM, underscored by the fact that the clinical features included some oppositional effects (e.g., both miotic and dilated pupils and both hypertension and hypotension) (Bäckberg et al. ref. 2016). Nevertheless, the authors of this case series suggested that 3-FPM is a harmful compound, as one-third of patients presented severe adverse events (Bäckberg et al. ref. 2016). In addition to other polydrug intoxications that involve 3-FPM (Benesch and Iqbal ref. 2018; Ellefsen et al. ref. 2017), a case of severe kidney injury and limb ischemia that were associated with intravenous 3-FPM use was reported (Fawzy et al. ref. 2017). The authors of the latter case report hypothesized that the intravenous use of 3-FPM resulted in severe vasoconstriction, possibly with concomitant infection, and caused widespread ischemia (Fawzy et al. ref. 2017).
Thiophene designer drugs
Various analogs of amphetamines and cathinones with a thiophene group that replaces the phenyl ring have appeared as designer drugs (Fig. 4). Some of the thiophene designer drugs were first described in the 1940s and elicited effects that were reported to be comparable to their phenyl ring analogs (Alles and Feigen ref. 1941; Blicke and Burckhalter ref. 1942). To date, most pharmacological studies and toxicological reports involve methiopropamine (MPA), the thiophene analog of methamphetamine.
Mechanism of action of thiophene designer drugs
MPA is a quasi-equipotent inhibitor of norepinephrine and dopamine uptake and was reported to interact with various serotonergic, adrenergic, dopaminergic, N-methyl-d-aspartate (NMDA), and sigma-1 receptors (Iversen et al. ref. 2013).
Adverse effects of thiophene designer drugs
MPA use has been associated with significant acute toxicity and psychotic, cardiovascular, and gastrointestinal symptoms, including agitation, anxiety, confusion, a lower level of consciousness, insomnia, visual hallucinations, elevations of creatine kinase, tachycardia, palpitations, chest tightness, nausea, and vomiting (Daveluy et al. ref. 2016; Lee et al. ref. 2014; White et al. ref. 2019). However, for most intoxication cases, the use of multiple substances was reported, and the extent to which MPA contributed to the reported adverse effects remains unclear. A death from isolated MPA use was described, in which cardiac arrhythmia that induced cardiovascular collapse was named as the probable cause of death (Anne et al. ref. 2015). Dopaminergic neurodegeneration and myocardial, renal, and gastrointestinal damage were observed in mice that were exposed to MPA (Foti et al. ref. 2019; Nguyen et al. ref. 2019).
Miscellaneous stimulants
Several designer drugs have appeared that do not belong to any classes that are discussed in the previous sections. Any substance that interacts with monoamine transporters may potentially be sold as a stimulant designer drug, even if it is not or only remotely chemically related to the widely used stimulant classes. One example of such a substance is the potent NET, DAT, and SERT blocker diclofensine, a tetrahydroisoquinoline derivative that was originally developed as an antidepressant (Luethi et al. ref. 2018a).
Sedatives
Synthetic opioids
While being essential for pain treatment, the non-medical use of opioids has been a public health threat for centuries and includes the recreational use of illegal substances, the abuse of prescription medications, and drug adulteration with non-pharmaceutical opioids (Armenian et al. ref. 2018b). Opioids induce euphoria, anxiolysis, feelings of relaxation, and drowsiness (Suzuki and El-Haddad ref. 2017). Repeated use leads to the development of dependence. In recent years, the growing prevalence of non-pharmaceutical fentanyl, highly potent designer fentanyls, and other novel synthetic opioids (Fig. 5) has critically contributed to the opioid crisis, particularly in the United States (Daniulaityte et al. ref. 2017; Denton et al. ref. 2008; Lucyk and Nelson ref. 2017; Peterson et al. ref. 2016; Rudd et al. ref. 2016; Scholl et al. ref. 2018; Seth et al. ref. 2018). Notably, fentanyl-type substances are often detected in fatalities that are presumably associated with intravenous heroin use (Gladden et al. ref. 2019). The higher potency of fentanyl and its analogs compared with classic heroin results in a higher risk of overdose, particularly when they are mistaken for heroin. Fentanyl itself was first synthesized in 1960 and has become essential and widely used for intraoperative analgesia and in the form of transdermal patches for the management of chronic pain (Stanley ref. 2014). Following its medical approval, reports of fentanyl misuse among clinicians and subsequently patients began to emerge, and several fentanyl analogs appeared on the illicit market (Armenian et al. ref. 2018b; Suzuki and El-Haddad ref. 2017). In Europe’s drug market, 49 new synthetic opioids were detected between 2009 and 2018, 34 of which are fentanyl derivatives (European Monitoring Centre for Drugs and Drug Addiction ref. 2019).
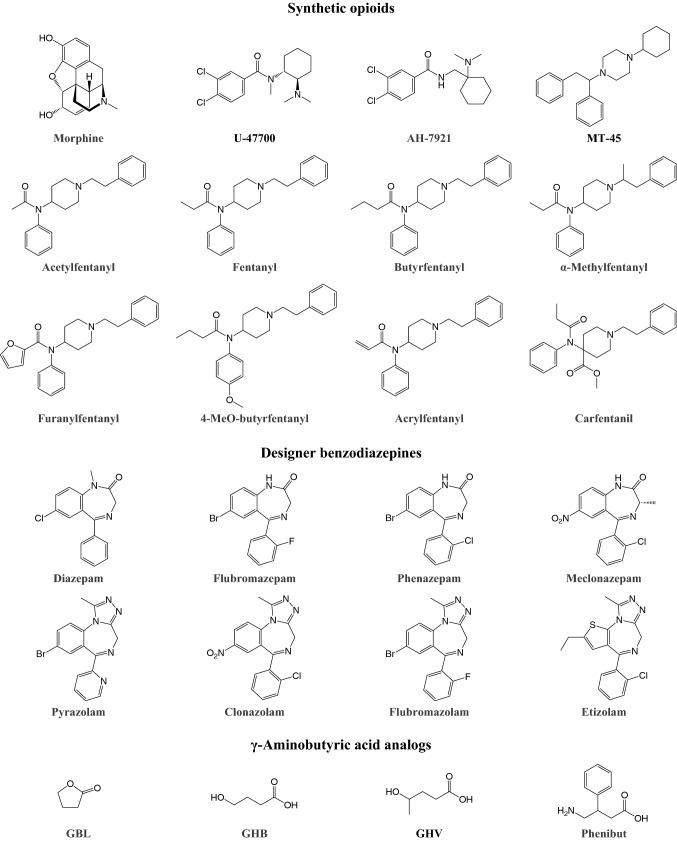
Mechanism of action of synthetic opioids
Novel fentanyl analogs and other synthetic opioids interact with G protein-coupled opioid receptors in the brain and spinal cord as partial to full agonists at μ-, δ-, and κ-opioid receptor subtypes, with selectivity for the μ-opioid receptor (Armenian et al. ref. 2018b; Baumann et al. ref. 2018; Codd et al. ref. 1995; Maguire et al. ref. 1992; Prekupec et al. ref. 2017). Multiple lines of evidence indicate that agonism at μ-opioid receptors drives the main pharmacological effects of opioids, including euphoria, analgesia, respiratory depression, and the development of dependence (Charbogne et al. ref. 2014; Kieffer ref. 1999). A detailed overview of signaling mechanisms and behavioral effects of opioid receptor activation is provided elsewhere (Al-Hasani and Bruchas ref. 2011). In vitro pharmacological profiling appears to be only a limited predictor of the clinical potency of opioids (Baumann et al. ref. 2018). However, rodent tail flick tests suggest mostly distinctively greater potencies of novel synthetic opioids compared with morphine (Armenian et al. ref. 2018b). For example, the potency of fentanyl is reported to be 50- to 200-fold higher than morphine, and the potency of carfentanil is reported to be approximately 10,000 times higher than morphine (Armenian et al. ref. 2018b; Concheiro et al. ref. 2018; Suzuki and El-Haddad ref. 2017). Several prescription opioids inhibit the NET and SERT and interact with 5-HT2 receptors (Codd et al. ref. 1995; Rickli et al. ref. 2018). Fentanyl has affinity for 5-HT1A and 5-HT2A receptors but is devoid of relevant monoamine transporter interactions (Barann et al. ref. 2015; Rickli et al. ref. 2018). No data are currently available on monoamine transporter interactions of designer opioids.
Adverse effects of synthetic opioids
Adverse effects of novel synthetic opioids include typical symptoms of opioid overdose, such as dizziness, a lower level of consciousness, miosis, central nervous system depression, respiratory depression, pulmonary edema, hypoxia, bradycardia, pruritus, nausea, vomiting, constipation, and also such symptoms as agitation, hypertension, and tachycardia (Armenian et al. ref. 2017, ref. 2018b; Bäckberg et al. ref. 2015b; Domanski et al. ref. 2017; Helander et al. ref. 2014, ref. 2016, ref. 2017a; Jones et al. ref. 2017; Müller et al. ref. 2019; Schneir et al. ref. 2017; Siddiqi et al. ref. 2015; Wilde et al. ref. 2020). Pulmonary edema, acute lung injury, diffuse alveolar hemorrhage, renal insufficiency, and rhabdomyolysis were also reported in patients who presented with designer opioid intoxication (Cole et al. ref. 2015; Helander et al. ref. 2016, ref. 2017a). The synthetic opioid 1-cyclohexyl-4-(1,2-diphenylethyl)piperazine (MT-45) has been associated with bilateral hearing loss and hearing disturbances, with likely irreversible and pronounced sensorineural hearing impairment in one case (Helander et al. ref. 2014). Furthermore, acute skin and hair symptoms followed by severe delayed eye complications were reported in patients with confirmed MT-45 use; cataract surgery was required in two of these patients (Helander et al. ref. 2017b). Remaining unclear, however, is whether the aforementioned complications are solely attributable to MT-45 toxicity. Serotonergic toxicity is one adverse effect that needs to be considered for opioid designer drugs when combined with other serotonergic agents (Baldo ref. 2018; Rickli et al. ref. 2018). Similar to traditional opioids, withdrawal from designer opioids may result in physiological and psychological distress (Siddiqi et al. ref. 2015). Numerous fatalities have been attributed to either designer opioids alone or designer opioids combined with other psychoactive substances (Coopman et al. ref. 2016a, ref. b; Cunningham et al. ref. 2016; Dussy et al. ref. 2016; Dwyer et al. ref. 2018; Elliott et al. ref. 2016; Fels et al. ref. 2017, ref. 2019; Fort et al. ref. 2016; Garneau et al. ref. 2019; Gillespie et al. ref. 1982; Guerrieri et al. ref. 2017; Helander et al. ref. 2017a; Karinen et al. ref. 2014; Koch et al. ref. 2018; Kriikku et al. ref. 2019; Kronstrand et al. ref. 2014; Krotulski et al. ref. 2018; Martucci et al. ref. 2018; McIntyre et al. ref. 2015b, ref. 2016, ref. 2017; Mohr et al. ref. 2016; Nash et al. ref. 2019; Ojanperä et al. ref. 2006; Papsun et al. ref. 2016; Partridge et al. ref. 2018; Poklis et al. ref. 2016; Richeval et al. ref. 2019; Ruan et al. ref. 2016; Sofalvi et al. ref. 2017; Staeheli et al. ref. 2016; Swanson et al. ref. 2017; Takase et al. ref. 2016; Vorce et al. ref. 2014; Yonemitsu et al. ref. 2016). Frisoni and colleagues recently published an overview of opioid-related fatalities that were attributed to synthetic opioids (Frisoni et al. ref. 2018). In addition to central nervous system and respiratory depression, chest wall rigidity after intravenous use could be a cause of death in synthetic opioid overdose cases (Burns et al. ref. 2016). The competitive μ-opioid receptor antagonist naloxone rapidly reverses central and peripheral effects of opioids and is thus an effective antidote for opioid toxicity (Armenian et al. ref. 2018b). The initial care of patients who are intoxicated with designer opioids should focus on airway protection and maintaining breathing and circulation (Armenian et al. ref. 2018b). Naloxone should be administered as soon as possible (Armenian et al. ref. 2018b; Kim and Nelson ref. 2015).
Designer benzodiazepines
In 1960, chlordiazepoxide became the first of several medically approved benzodiazepines that today represent a widely prescribed class of drugs for the treatment of psychiatric and neurological conditions, particularly insomnia and anxiety disorders (Longo and Johnson ref. 2000; Sternbach ref. 1979). Benzodiazepine abuse is frequent. The main reasons for such abuse are to facilitate sleep, cope with stress, ease effects of stimulants, self-treat withdrawal symptoms, and get high (Kapil et al. ref. 2014; Vogel et al. ref. 2013; Zawilska and Wojcieszak ref. 2019). Benzodiazepines have limited potential as euphoriants when administered alone. When taken in combination with opioids, however, benzodiazepines appear to enhance the euphoric effects of opioid use (Jones et al. ref. 2012). Since 2007, several benzodiazepine designer drugs (Fig. 5) have become available, some of which are precursors or metabolites of prescription benzodiazepines and are approved for medical use in other countries (Bäckberg et al. ref. 2019; Manchester et al. ref. 2018). Effects of designer benzodiazepines reported on internet forums resemble those of prescription benzodiazepines (El Balkhi et al. ref. 2020). Chronological overviews of the appearance of benzodiazepine designer drugs on the recreational drug market were recently published (Manchester et al. ref. 2018; Moosmann and Auwärter ref. 2018).
Mechanism of action of designer benzodiazepines
The mechanism of action of most benzodiazepine designer drugs currently remains understudied. In silico experiments suggest that they mediate their effects through interactions at γ-aminobutyric acid-A (GABAA) receptors such as prescription benzodiazepines (Waters et al. ref. 2018). GABAA receptors are ion channels that consist of pentamers of different subunit compositions, responding to the inhibitory neurotransmitter GABA. Benzodiazepines enhance the effects of GABA as positive allosteric modulators by binding to a receptor site that is different from the binding site of GABA (Manchester et al. ref. 2018; Moosmann and Auwärter ref. 2018).
Adverse effects of designer benzodiazepines
Despite their depressive actions on central nervous system function and respiration, the isolated use of benzodiazepines is rarely fatal. However, in reported intoxication cases, designer benzodiazepines have mostly been detected in combination with other psychoactive substances, such as stimulants or depressants (Bäckberg et al. ref. 2019). The concurrent use of benzodiazepines and other depressants, such as opioids and alcohol, may produce prolonged and potentially fatal respiratory depression (Jones et al. ref. 2012; Zawilska and Wojcieszak ref. 2019). Reported adverse effects of isolated benzodiazepine designer drugs are typical for a sedative-hypnotic toxidrome but may include atypical symptoms in some cases, such as agitation, hyperthermia, and tachycardia (Bäckberg et al. ref. 2019; Carpenter et al. ref. 2019; Zawilska and Wojcieszak ref. 2019). The recent review by Zawilska and Wojcieszak mentioned the following adverse effects of designer benzodiazepines: fatigue, impairment of thinking, confusion, dizziness, drowsiness, lethargy, amnesia, blurred vision, slurred speech, palpitations, and muscle weakness, as well as auditory and visual hallucinations, delirium, seizures, deep sleep, and coma at high doses (Zawilska and Wojcieszak ref. 2019). The chronic use of designer benzodiazepines may also lead to the development of tolerance and dependence (Zawilska and Wojcieszak ref. 2019). Withdrawal symptoms, such as anxiety, panic attacks, restlessness, insomnia, seizures, and life-threatening convulsions, may follow the abrupt cessation of chronic designer benzodiazepines use (Andersson and Kjellgren ref. 2017; Zawilska and Wojcieszak ref. 2019). Designer benzodiazepines have been reported to contribute to numerous deaths (Bailey et al. ref. 2010; Crichton et al. ref. 2015; Domingo et al. ref. 2017; Karinen et al. ref. 2014; Koch et al. ref. 2018; Liveri et al. ref. 2016; Maskell et al. ref. 2011b; Papsun et al. ref. 2016; Partridge et al. ref. 2018; Shearer et al. ref. 2015; Tanaka et al. ref. 2011a, ref. b). In a few cases, the cause of death was solely attributed to the designer benzodiazepine phenazepam (Crichton et al. ref. 2015; Shearer et al. ref. 2015) or etizolam (Carpenter et al. ref. 2019). A more detailed summary of benzodiazepine-related fatalities was recently published (Zawilska and Wojcieszak ref. 2019).
γ-Aminobutyric acid analogs
γ–Hydroxybutyrate (GHB) is a short-chain fatty acid analog of the inhibitory neurotransmitter GABA. It has become popular among drug users because of its ability to induce feelings of euphoria and relaxation, reduce social anxiety, and increase sexual drive (Brennan and Van Hout ref. 2014; Brown et al. ref. 2011). Although it is an endogenous compound and its sodium salt is approved as a prescription drug against narcolepsy, GHB and its metabolic precursors (e.g., γ-butyrolactone [GBL] and 1,4-butanediol [1,4-BD]) are often referred to as designer drugs because of their widespread illicit production in clandestine laboratories (Brennan and Van Hout ref. 2014; Fuller et al. ref. 2004). Other structural analogs of GABA that have become available as designer drugs (Fig. 5) include the 4-methyl-substituted GHB derivative γ–hydroxyvaleric acid (GHV) and 4-amino-3-phenyl-butyric acid (phenibut) (Carter et al. ref. 2005; Owen et al. ref. 2016).
Mechanism of action of GABA analogs
Metabotropic G protein-coupled GABAB receptors are the primary targets of designer drug analogs of GABA (Brennan and Van Hout ref. 2014; Carai et al. ref. 2001; Lapin ref. 2001). Other postulated mechanisms of action include high-affinity binding to receptor sites that are distinct from the GABAB receptor (i.e., GHB receptors), binding to specific GABAA receptor subtypes, and monoaminergic modulation (Bay et al. ref. 2014; Carter et al. ref. 2009; Crunelli et al. ref. 2006; Lapin ref. 2001; Wood et al. ref. 2011).
Adverse effects of GABA analogs
Comprehensive reviews of the potential clinical complications of the use of GHB and its metabolic precursors are provided elsewhere (Busardò and Jones ref. 2015; Schep et al. ref. 2012). The subjective benefits of GHB and its analogs outweigh adverse events only over a narrow range of doses. Adverse events include a lower level of consciousness, hypothermia, respiratory depression, aspiration, bradycardia, gastrointestinal upset, and nonsedative adverse effects, such as agitation, seizures, and myoclonus (Busardò and Jones ref. 2015; Isoardi et al. ref. 2020; Liakoni et al. ref. 2016; McCabe et al. ref. 2019; Schep et al. ref. 2012; Zvosec and Smith ref. 2005). These adverse effects typically have a relatively short duration and are usually managed with supportive care (Busardò and Jones ref. 2015; Schep et al. ref. 2012; Wood et al. ref. 2011). GABAB and monocarboxylate transporter inhibitors have been proposed as potential treatment options for GHB-induced respiratory depression (Morse et al. ref. 2012). GHB and its analogs are associated with the rapid development of tolerance. Abrupt cessation after regular use may trigger a potentially life-threatening withdrawal syndrome that can manifest as agitation, anxiety, confusion, disorientation, paranoia, aggression, insomnia, auditory and visual hallucinations, tremors, sweating, hypertension, and tachycardia (Busardò and Jones ref. 2015; Owen et al. ref. 2016; Schep et al. ref. 2012; Wood et al. ref. 2011). Benzodiazepines appear to be the treatment of choice for withdrawal from GHB and its analogs (Busardò and Jones ref. 2015; Schep et al. ref. 2012; Wood et al. ref. 2011). Zvosec and colleagues reported a series of 226 GHB-associated deaths, 213 of which were attributed to cardiorespiratory arrest and 13 of which were attributed to fatal accidents (Zvosec et al. ref. 2011). In approximately one-third of these fatal cases, GHB was the sole toxicant detected (Zvosec et al. ref. 2011). Similar findings were reported by Corkery and colleagues, who reported a series of 159 GHB and GBL-associated fatalities (Corkery et al. ref. 2015). The co-ingestion of opioids increases the depressant toxicity of GHB, and stimulant intake does not appear to prevent GHB toxicity (Knudsen et al. ref. 2010).
Dissociatives
Arylcyclohexylamine and diarylethylamine designer drugs
Dissociative agents are appreciated in medicine because of their unique pharmacological effects. These pharmacological effects, however, are also popular among recreational drug users. The dissociative anesthetic ketamine produces analgesia without cardiovascular or respiratory depression at doses that produce anesthesia, a feature that is not shared by other common anesthetics (Li and Vlisides ref. 2016). Furthermore, ketamine induces rapid and sustained antidepressant actions at a single sub-anesthetic dose and has become a widely abused recreational drug because of its dissociative effects, including sensory and tactile distortions, euphoria, and depersonalization (Li and Vlisides ref. 2016; Zanos and Gould ref. 2018). Ketamine was first synthesized in 1962 as a short-acting anesthetic with lower potency in producing emergence delirium compared with the structurally similar phencyclidine (PCP). PCP was developed before ketamine as a promising dissociative anesthetic, but its use in humans and animals was discontinued because of its unfavorable side effects (Domino ref. 1980). Various similar substances have been clinically investigated. Dissociatives began to appear on the illicit drug market in the late 1960s (Morris and Wallach ref. 2014). Today, several dissociative designer drugs (Fig. 6) are available, mostly arylcyclohexylamines (e.g., ketamine and PCP) and diarylethylamines. Morris, Wallach, and Brandt previously published comprehensive overviews of the history, availability, and use of several arylcyclohexylamine and diarylethylamine designer drugs and other dissociative agents (Morris and Wallach ref. 2014; Wallach and Brandt ref. 2018a, ref. b).
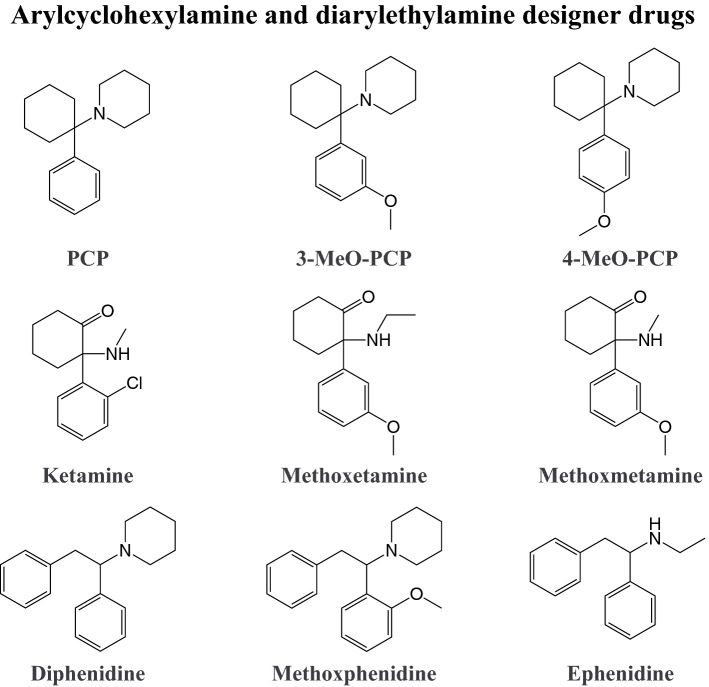
Mechanism of action of arylcyclohexylamine and diarylethylamine designer drugs
Similar to ketamine and PCP, dissociative arylcyclohexylamine and diarylethylamine designer drugs act as relatively selective noncompetitive antagonists at ionotropic glutamatergic NMDA receptors. Their NMDA receptor affinity is strongly correlated with their clinical potency in inducing dissociative effects in vivo (Anis et al. ref. 1983; Morris and Wallach ref. 2014; Wallach et al. ref. 2016). Some dissociative designer drugs also moderately inhibit the reuptake of norepinephrine and dopamine, whereas others have appreciable affinity for the SERT (Luethi et al. ref. 2018a; Roth et al. ref. 2013; Wallach et al. ref. 2016). Binding affinity at various receptors, including α adrenergic, serotonergic, histaminergic, cholinergic, opioidergic, and sigma receptors, has been reported for arylcyclohexylamines and diarylethylamines (Luethi et al. ref. 2018a; Roth et al. ref. 2013; Wallach et al. ref. 2016). Summarized, NMDA receptor antagonism mainly mediates the dissociative effects of arylcyclohexylamines and diarylethylamines, and interactions with other pharmacological targets may modify the activity of different compounds.
Adverse effects of arylcyclohexylamine and diarylethylamine designer drugs
Adverse effects of dissociative arylcyclohexylamine and diarylethylamine designer drugs resemble adverse effects of traditional dissociatives, including agitation, confusion, disorientation, dissociation, hallucinations, amnesia, nystagmus, slurred speech, diaphoresis, hypertension, tachycardia, renal deficiency, nausea, ataxia, and muscle rigidity (Bäckberg et al. ref. 2015a; Dunlop et al. ref. 2019; Gerace et al. ref. 2017; Helander et al. ref. 2015; Hofer et al. ref. 2012, ref. 2014; Johansson et al. ref. 2017; Shields et al. ref. 2012; Thornton et al. ref. 2017; Ward et al. ref. 2011; Wood et al. ref. 2012; Zawilska ref. 2014; Zidkova et al. ref. 2017). In severe cases, dissociative designer drugs may potentially cause neurological impairment, manifested as cerebellar toxicity (Shields et al. ref. 2012) or rhabdomyolysis (Bäckberg et al. ref. 2015a; Lam et al. ref. 2016). Severe adverse effects associated with inhalation of the designer drug methoxetamine include seizures, hyponatremia, and sinus bradycardia (Imbert et al. ref. 2014). Regular ketamine use has been associated with potentially irreversible bladder dysfunction and subsequent renal impairment (Chu et al. ref. 2007; Tsai et al. ref. 2009). Animal studies suggest that this may also be a consequence of regular methoxetamine use (Dargan et al. ref. 2014; Wang et al. ref. 2017). In a survey of methoxetamine users, approximately one-fourth reported urinary symptoms (Lawn et al. ref. 2016). The prevalence of urinary symptoms was related to the frequency of methoxetamine use during the previous month, but prior ketamine use could have also contributed to these symptoms (Lawn et al. ref. 2016). Other dissociative designer drugs may also cause such severe urinary tract dysfunction, but detailed research has not been conducted. Additionally, the acute and chronic use of dissociative designer drugs potentially elicits wide-ranging effects on memory systems, similar to ketamine (Morgan and Curran ref. 2006). Dissociative designer drugs have been involved in numerous fatal intoxications, mostly in combination with other designer drugs, including stimulants, opioids, cannabinoids, and psychedelics (Adamowicz and Zuba ref. 2015; Bakota et al. ref. 2016; Chiappini et al. ref. 2015; De Jong et al. ref. 2019; Elliott et al. ref. 2015; Johansson et al. ref. 2017; Krotulski et al. ref. 2018; Kudo et al. ref. 2015; Kusano et al. ref. 2018; McIntyre et al. ref. 2015c; Mitchell-Mata et al. ref. 2017; Wiergowski et al. ref. 2014; Wikström et al. ref. 2013). Wallach and Brandt previously published a detailed overview of the clinical toxicology of individual PCP analogs (Wallach and Brandt ref. 2018b) and diarylethylamine- and ketamine-based designer drugs (Wallach and Brandt ref. 2018a).
Synthetic cannabinoids
The endocannabinoid system is involved in various physiological functions, including cognition, behavior, memory, motor control, pain sensation, appetite, cardiovascular parameters, gastrointestinal motility, and immunoregulation (Le Boisselier et al. ref. 2017). The term “cannabinoid” refers to a class of compounds that are produced by Cannabis sativa and Cannabis indica, and endogenous and exogenous ligands that interact with G protein-coupled cannabinoid type 1 (CB1) and CB2 receptors (Banister and Connor ref. 2018; Le Boisselier et al. ref. 2017). CB1 receptors are mainly expressed in the brain and modulate neurotransmitter signaling, whereas CB2 receptors are abundant in immune tissues (Banister and Connor ref. 2018; Le Boisselier et al. ref. 2017). The first synthetic cannabinoids were developed in the second half of the twentieth century to study human endocannabinoid receptor systems (Banister and Connor ref. 2018; Le Boisselier et al. ref. 2017; Trecki et al. ref. 2015). Today, synthetic cannabinoids (Fig. 7) represent the largest and most structurally diverse class of designer drugs, and some of these compounds are similar to phyto- and endocannabinoids (Banister and Connor ref. 2018; Trecki et al. ref. 2015). Synthetic cannabinoids are often referred to as “Spice,” based on the first branded synthetic cannabinoid product. They are commonly applied to dried herbs that mimic cannabis (Banister and Connor ref. 2018; Le Boisselier et al. ref. 2017; Trecki et al. ref. 2015). Desired effects of synthetic cannabinoids include relaxation, euphoria, and disinhibition, thus not significantly differing from desired effects of Δ9-tetrahydrocannabinol (Δ9-THC), the main psychoactive constituent of cannabis (Le Boisselier et al. ref. 2017). However, compared with cannabis, synthetic cannabinoids have a less desirable effect profile and are associated with more severe adverse events that sometimes can result in death (Trecki et al. ref. 2015; Winstock and Barratt ref. 2013).
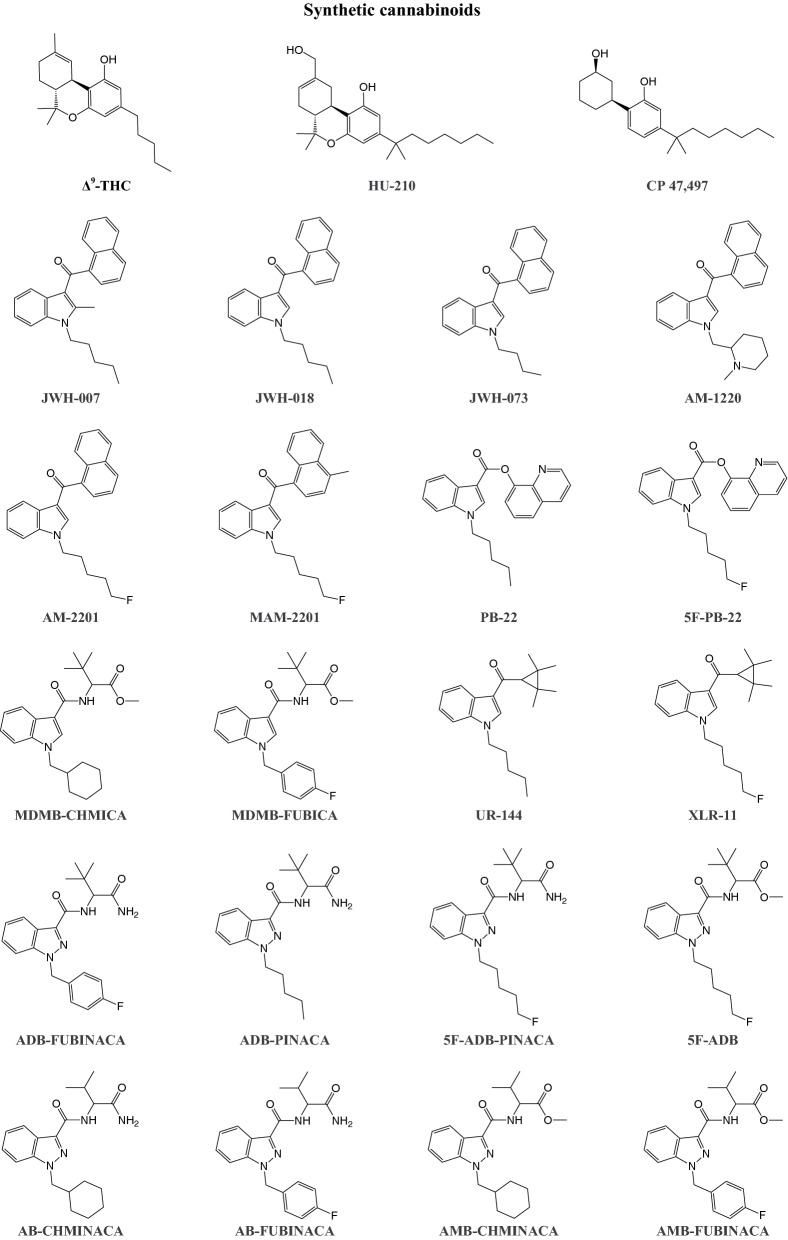
Mechanism of action of synthetic cannabinoids
Various synthetic cannabinoids have been reported to bind to CB1 and CB2 receptors with higher efficacy at both receptors compared with Δ9-THC (Banister et al. ref. 2015a, ref. b, ref. 2016, ref. 2019; Gamage et al. ref. 2018; Sachdev et al. ref. 2019). Biased signaling at cannabinoid receptors or the disruption of mitochondrial homeostasis may play a role in the difference between clinical effects of Δ9-THC and synthetic cannabinoids, but research in this area is still in its infancy (Finlay et al. ref. 2019; Silva et al. ref. 2018, ref. 2019). CB1 receptors are involved in multiple mechanisms that lead to the suppression of synaptic transmission. Compared with CB2 receptor expression, the predominance of CB1 receptors in the central nervous system indicates that they mainly mediate the psychoactive effects of synthetic cannabinoids (Atwood et al. ref. 2010; Castillo et al. ref. 2012; Kano et al. ref. 2009; Le Boisselier et al. ref. 2017). This assumption is strengthened by studies that reported that CB1 receptor antagonism but not CB2 receptor antagonism inhibits the synthetic cannabinoid-induced lowering of heart rate and body temperature in rodents (Banister et al. ref. 2015a, ref. 2019a). In vitro studies showed that various metabolites of synthetic cannabinoids retain some cannabimimetic activity, indicating that they could contribute to the pharmacological effects of the drugs (Longworth et al. ref. 2017). In contrast, some substances that are promoted as cannabinoid designer drugs have only low in vitro affinity for cannabinoid receptors and fail to exert significant cannabinoid activity in vivo, thus calling into question their classification as synthetic cannabinoids (Banister et al. ref. 2019b). Only a few synthetic cannabinoids have been studied to date with regard to their interactions with non-cannabinoid targets, with low or no affinity for most major neurotransmitter receptors (Wiley et al. ref. 2016). This suggests that different effects of synthetic cannabinoids compared with Δ9-THC are mainly related to greater potency and efficacy at CB1 receptors, but possible effects on non-cannabinoid receptors and different signaling pathways that have not yet been discovered cannot be ruled out (Finlay et al. ref. 2019; Wiley et al. ref. 2016). Furthermore, pharmacokinetic differences may contribute to these differences.
Adverse effects of synthetic cannabinoids
The most common adverse effects of synthetic cannabinoids include agitation, drowsiness, dizziness, confusion, hallucinations, hypertension, tachycardia, chest pain, nausea, and vomiting, which typically have a short duration and require only symptomatic or supportive treatment (Forrester ref. 2012a; Forrester et al. ref. 2011, ref. 2012; Hoyte et al. ref. 2012; Law et al. ref. 2015; Tait et al. ref. 2016). Nevertheless, compared with cannabis, complications that are associated with synthetic cannabinoid use are more frequent and in some cases, more severe (Alipour et al. ref. 2019; Bäckberg et al. ref. 2017; Mensen et al. ref. 2019; Tait et al. ref. 2016; Trecki et al. ref. 2015). Various severe adverse events that are associated with synthetic cannabinoids have been reported. However, many of these cases were attributed to synthetic cannabinoid use based solely on statements by patients or witnesses, without analytical confirmation of the identity and amount of substances in bodily fluids or remaining drug products. Severe clinical complications that have been reported to be associated with synthetic cannabinoid use include convulsions and seizures (Adamowicz et al. ref. 2017; Bäckberg et al. ref. 2017; Bebarta et al. ref. 2012; De Havenon et al. ref. 2011; Gugelmann et al. ref. 2014; Harris and Brown ref. 2013; Hermanns-Clausen et al. ref. 2013a, ref. b; Hoyte et al. ref. 2012; Lapoint et al. ref. 2011; McQuade et al. ref. 2013; Pant et al. ref. 2012; Schep et al. ref. 2015; Schneir and Baumbacher ref. 2012; Tofighi and Lee ref. 2012), status epileptics (Babi et al. ref. 2017), catatonia (Khan et al. ref. 2016; Leibu et al. ref. 2013; Smith and Roberts ref. 2014), delirium (Armenian et al. ref. 2018a; Armstrong et al. ref. 2019; Bäckberg et al. ref. 2017; Schwartz et al. ref. 2015; Tyndall et al. ref. 2015), ischemic stroke (Bernson-Leung et al. ref. 2014; Faroqui et al. ref. 2018; Freeman et al. ref. 2013; Moeller et al. ref. 2017; Raheemullah and Laurence ref. 2016; Takematsu et al. ref. 2014; Wolff and Jouanjus ref. 2017), intracranial hemorrhage (Aydin and Bakar ref. 2019; Rose et al. ref. 2015), pulmonary embolism (Raheemullah and Laurence ref. 2016; Yirgin et al. ref. 2018), pneumonia and pulmonary infiltrates (Alhadi et al. ref. 2013; Alon and Saint-Fleur ref. 2017; Berkowitz et al. ref. 2015; Chinnadurai et al. ref. 2016; Öcal et al. ref. 2016), respiratory depression (Alon and Saint-Fleur ref. 2017; Jinwala and Gupta ref. 2012), supraventricular and ventricular arrhythmias (Davis and Boddington ref. 2015; Ibrahim et al. ref. 2014; Ozturk et al. ref. 2019; Young et al. ref. 2012), myocardial ischemia and infarction (Clark et al. ref. 2015; Hamilton et al. ref. 2017; Hirapara and Aggarwal ref. 2015; McIlroy et al. ref. 2016; McKeever et al. ref. 2015; Mehta et al. ref. 2017; Mills et al. ref. 2018; Mir et al. ref. 2011; Ozturk et al. ref. 2019; Shah et al. ref. 2016; Sherpa et al. ref. 2015; Tse et al. ref. 2014), takotsubo cardiomyopathy (Mohammed ref. 2019), liver injury (Shahbaz et al. ref. 2018), acute kidney injury (Argamany et al. ref. 2016; Armstrong et al. ref. 2019; Bhanushali et al. ref. 2013; Buser et al. ref. 2014; El Zahran et al. ref. 2019; Gudsoorkar and Perez ref. 2015; Kamel and Thajudeen ref. 2015; Katz et al. ref. 2016b; Kazory and Aiyer ref. 2013; Srisung et al. ref. 2015; Thornton et al. ref. 2013; Zarifi and Vyas ref. 2017; Zhao et al. ref. 2015), hyperemesis syndrome (Argamany et al. ref. 2016; Bick et al. ref. 2014; Hopkins and Gilchrist ref. 2013; Ukaigwe et al. ref. 2014), and rhabdomyolysis (Adedinsewo et al. ref. 2016; Argamany et al. ref. 2016; Armstrong et al. ref. 2019; Durand et al. ref. 2015; El Zahran et al. ref. 2019; Katz et al. ref. 2016b; Sherpa et al. ref. 2015; Sweeney et al. ref. 2016; Zhao et al. ref. 2015). Furthermore, various psychiatric adverse effects have been reported, including paranoia, psychosis, and ideations of self-harm and suicide (Akram et al. ref. 2019; Altintas et al. ref. 2016; Bassir Nia et al. ref. 2019; Benford and Caplan ref. 2011; Berry-Caban et al. ref. 2013; Bonaccorso et al. ref. 2018; Darke et al. ref. 2019; Deng et al. ref. 2018; Derungs et al. ref. 2013; Durand et al. ref. 2015; Every-Palmer ref. 2010; Glue et al. ref. 2013; Hermanns-Clausen et al. ref. 2013b; Hobbs et al. ref. 2018; Hurst et al. ref. 2011; Kraemer et al. ref. 2019; Martinotti et al. ref. 2017; Meijer et al. ref. 2014; Mensen et al. ref. 2019; Müller et al. ref. 2010; Oliveira et al. ref. 2017; Oluwabusi et al. ref. 2012; Papanti et al. ref. 2013; Patton et al. ref. 2013; Peglow et al. ref. 2012; Roberto et al. ref. 2016; Skryabin and Vinnikova ref. 2019; Sweet et al. ref. 2017; Thomas et al. ref. 2012; Van Amsterdam et al. ref. 2015; Van der Veer and Friday ref. 2011; Welter et al. ref. 2017; Yeruva et al. ref. 2019). The sudden discontinuation of synthetic cannabinoid use in regular
Psychedelics
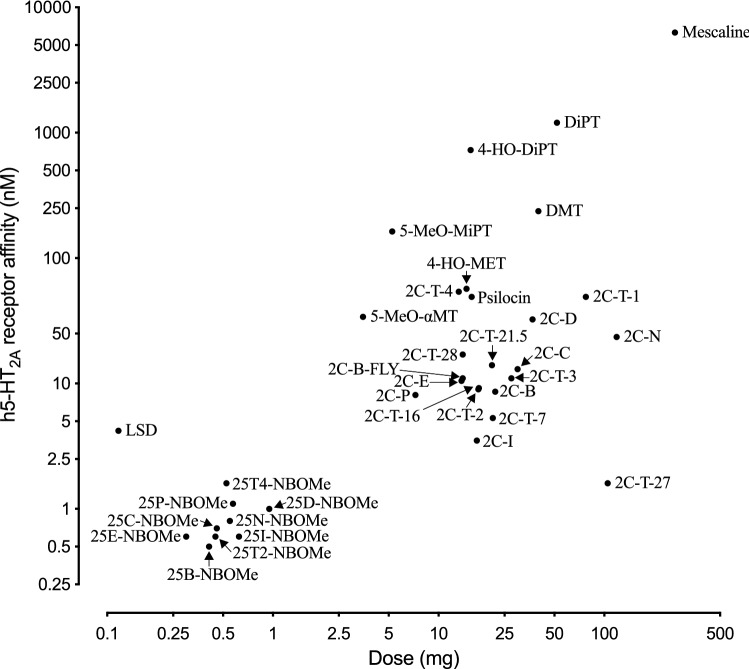
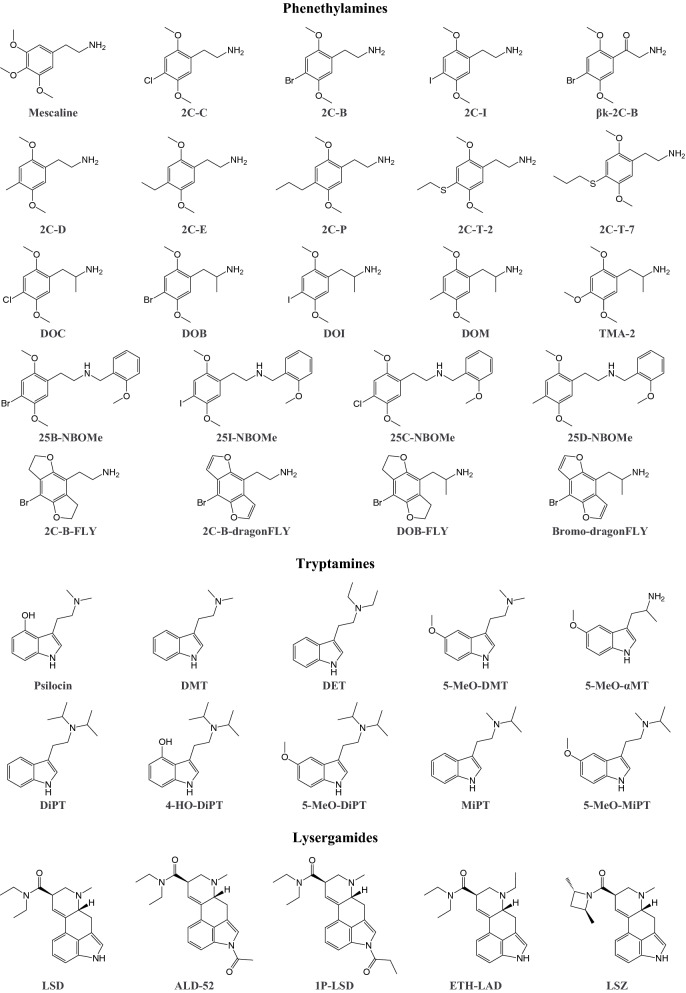
Serotonergic psychedelics induce alterations of perception and cognitive states in users (Nichols ref. 2004, ref. 2016). Traditional psychedelics, such as the phenethylamine 3,4,5-trimethoxyphenethylamine (mescaline), the tryptamines N,N-dimethyltryptamine (DMT) and psilocybin, and the ergot alkaloid lysergic acid diethylamide (LSD), have a history of being used for religious purposes, as therapeutic agents, and as illicit black market drugs. Although psychedelics interact with various pharmacological targets, their psychedelic effects are mainly mediated by 5-HT2A receptor agonism (Geyer and Vollenweider ref. 2008; Kraehenmann et al. ref. 2017; Madsen et al. ref. 2019; Nichols ref. 2004, ref. 2016; Preller et al. ref. 2018; Vollenweider et al. ref. 1998). Affinity for 5-HT2A and 5-HT2C receptors is correlated with the amount of drug that induces psychedelic effects in humans (Fig. 8) (Luethi and Liechti ref. 2018). Designer drug analogs of all the traditional psychedelic drugs are available, some of which were originally developed by industry or university laboratories but have eventually found their way onto the illicit drug market.
Phenethylamines
Derivatives of mescaline comprise a large amount of psychedelic designer drugs (Fig. 9). The most widespread phenethylamine psychedelics are 2,5-dimethoxyphenethylamines, which bear a small lipophilic substituent at the 4-position (referred to as 2C series because they bear two carbon atoms between the benzene ring and amino group), and their slightly more potent α-methyl (amphetamine) analogs (Shulgin and Shulgin ref. 1995). Psychedelic phenethylamine derivatives are mostly but not exclusively chemically modified at the phenyl ring. The introduction of an N-benzylmethoxy (“NBOMe”) group has been shown to increase the potency of the resulting derivatives (Eshleman et al. ref. 2018; Halberstadt ref. 2017; Heim ref. 2004; Rickli et al. ref. 2015c). The incorporation of 2′- and 5′-methoxy groups into rigid rings resulted in tetrahydrobenzodifuran and benzodifuran analogs that have been sold as designer drugs. These tetrahydrobenzodifuran and benzodifuran designer drugs are referred to as “FLY” and “dragonFLY” analogs, respectively, because of the shape of their chemical structure (Halberstadt et al. ref. 2019; Trachsel et al. ref. 2013). In one of the few clinical studies of a designer drug, 4-bromo-2,5-dimethoxyphenylethylamine (2C-B) was shown to induce euphoria, well-being, and changes in perception, and to have mild stimulant properties (González et al. ref. 2015). 2C-B may thus be classified as a psychedelic with entactogenic properties, an effect profile that is similar to various other phenethylamine psychedelics (Shulgin and Shulgin ref. 1995).
Mechanism of action of phenethylamines
Similar to other psychedelics, substituted phenethylamines mainly interact with serotonergic receptors, with the highest affinity for 5-HT2A receptors (Eshleman et al. ref. 2018; Kolaczynska et al. ref. 2019; Luethi et al. ref. 2018d; Rickli et al. ref. 2015c). NBOMe derivatives have higher affinity for 5-HT2A and 5-HT2C receptors and lower affinity for 5-HT1A receptors compared with their 2C analogs (Rickli et al. ref. 2015c). At 5-HT2A receptors, 2C and NBOMe derivatives were shown to be partial or full agonists, depending on the functional in vitro assay (Eshleman et al. ref. 2014, ref. 2018; Jensen et al. ref. 2017; Kolaczynska et al. ref. 2019; Luethi et al. ref. 2018d, ref. 2019c; Moya et al. ref. 2007; Rickli et al. ref. 2015c). NBOMe derivatives and most 2C derivatives have been shown to be partial agonists at 5-HT2B receptors (Eshleman et al. ref. 2018; Jensen et al. ref. 2017; Kolaczynska et al. ref. 2019; Luethi et al. ref. 2018d; Rickli et al. ref. 2015c). At 5-HT2C receptors, 2C derivatives were shown to be partial or full agonists (Eshleman et al. ref. 2014; Moya et al. ref. 2007), and NBOMe derivatives were shown to be full agonists (Eshleman et al. ref. 2018; Jensen et al. ref. 2017). Consistent with the in vitro findings, psychedelic phenethylamines were shown to induce 5-HT2A-dependent behaviors in vivo, such as wet dog shakes, back muscle contractions, and a head twitch response (Elmore et al. ref. 2018; Fantegrossi et al. ref. 2005; Halberstadt et al. ref. 2020; Halberstadt and Geyer ref. 2014). In addition to interactions with serotonergic receptors, phenethylamine psychedelics have been shown to interact with other monoaminergic targets, including adrenergic, dopaminergic, and histaminergic receptors, monoamine transporters, and MAOs (Eshleman et al. ref. 2018; Kolaczynska et al. ref. 2019; Luethi et al. ref. 2018d; Noble et al. ref. 2018; Rickli et al. ref. 2015c; Wagmann et al. ref. 2019a). However, most of these interactions are weak compared with the potent interactions with serotonergic receptors. Therefore, they most likely have little or no pharmacological relevance to the actions of phenethylamine psychedelics. Rodent studies have suggested reinforcing effects for NBOMe derivatives that involve the dopaminergic system (Custodio et al. ref. 2019; Seo et al. ref. 2019). The NBOMe derivative 4-iodo-2,5-dimethoxy-N-(2-methoxybenzyl)phenethylamine (25I-NBOMe) was shown to increase extracellular dopamine, 5-HT, and glutamate levels in the rat frontal cortex (Herian et al. ref. 2019), but unknown are the ways in which these findings translate to humans.
Adverse effects of phenethylamines
Most of the frequently reported adverse effects of phenethylamine psychedelics are shared by psychedelics of other chemical classes, including agitation, hallucinations, drowsiness, confusion, mydriasis, aggression, hyperthermia, hypertension, and tachycardia (Dean et al. ref. 2013; Forrester ref. 2013, ref. 2014; Hermanns-Clausen et al. ref. 2017; Hill et al. ref. 2013; Iwersen-Bergmann et al. ref. 2019; Rose et al. ref. 2013; Srisuma et al. ref. 2015; Stellpflug et al. ref. 2014; Stoller et al. ref. 2017; Tang et al. ref. 2014; Topeff et al. ref. 2011; Wood et al. ref. 2015). Moreover, severe adverse effects have been linked to the use of psychedelic phenethylamines, including acute psychosis, seizures, coma, cerebral edema, long-lasting severe neurological impairment, serotonin syndrome, prolonged respiratory failure, renal failure, multi-organ failure, metabolic acidosis, and rhabdomyolysis (Bosak et al. ref. 2013; Grautoff and Kähler ref. 2014; Halberstadt ref. 2017; Huang and Bai ref. 2011; Miyajima et al. ref. 2008; Srisuma et al. ref. 2015; Tang et al. ref. 2014; Wood et al. ref. 2009). Furthermore, 1-(4-bromofuro[2,3-f][1]benzofuran-8-yl)propan-2-amine (Bromo-dragonFLY) has been associated with potent vasoconstriction, ischemia, and tissue necrosis in patients, which may be caused by the activation of serotonergic and adrenergic receptors combined with metabolic stability and long-lasting effects (Hill and Thomas ref. 2011; Noble et al. ref. 2018; Thorlacius et al. ref. 2008; Wood et al. ref. 2009). A remarkable case of mass intoxication with 4-ethyl-2,5-dimethoxyphenethylamine (2C-E) and Bromo-dragonFLY among 29 attendees of an esoteric weekend seminar was reported (Iwersen-Bergmann et al. ref. 2019). Upon the arrival of paramedics, some of the seminar attendees were rolling on the ground and screaming, and others were unconscious or unresponsive. Several attendees exhibited severe delusions and physical symptoms, including generalized seizures, pain, respiratory distress, and tachycardia (Iwersen-Bergmann et al. ref. 2019). In some severe cases, the use of psychedelic phenethylamines has even resulted in death (Curtis et al. ref. 2003; Kueppers and Cooke ref. 2015; Poklis et al. ref. 2014; Shanks et al. ref. 2015a; Topeff et al. ref. 2011; Walterscheid et al. ref. 2014). Adverse effects of different phenethylamine designer drugs are mostly comparable. However, a higher incidence of hallucinations, delusions, and single-episode seizures has been observed for NBOMe derivatives compared with 2C derivatives (Srisuma et al. ref. 2015). This may be explained by the higher potency of NBOMe derivatives compared with most other phenethylamine psychedelics (Braden et al. ref. 2006; Elmore et al. ref. 2018; Halberstadt and Geyer ref. 2014; Rickli et al. ref. 2015c). Several reports have linked severe intoxication to substituted phenethylamines, but the lack of analytical confirmation of the drug prevents the direct attribution of adverse effects to phenethylamines. For example, a 43-year-old woman was reported to have developed severe headaches, progressive encephalopathy, and quadraparesis within 48 h after taking a liquid form of 2C-B that was synthesized according to a manual on the Internet (Ambrose et al. ref. 2010). However, the patient’s urine tested positive for cannabinoids only, and a sample of the ingested drug could not be obtained for analysis (Ambrose et al. ref. 2010). Similarly, a patient presented to an emergency department with hallucinations and agitation that progressed to status epilepticus after using of 4-chloro-2,5-dimethoxyamphetamine (DOC). In addition to the analytically confirmed presence of DOC, however, the toxicology screen was positive for cannabinoids and opioids, thus hampering the attribution of seizure development to DOC (Burish et al. ref. 2015). Additionally, several fatalities from 2C derivative use have been reported in the media, but the accuracy of this information cannot be verified (Dean et al. ref. 2013).
Tryptamines
The core structure of tryptamine designer drugs contains an indole ring that is connected to an amino group by an ethyl side chain, a structural feature that is shared by 5-HT. DMT as an ingredient in the psychoactive brew ayahuasca and psilocybin that is contained in Psilocybe spp. mushrooms have been used in sociocultural and ritual contexts since ancient times. They have recently regained interest for their therapeutic use (Araújo et al. ref. 2015; Carhart-Harris et al. ref. 2018; Muttoni et al. ref. 2019; Palhano-Fontes et al. ref. 2019; Roseman et al. ref. 2017). In addition to naturally occurring compounds, psychedelic properties of various synthetic tryptamines (Fig. 9) have been described (Shulgin and Shulgin ref. 1997).
Mechanism of action of tryptamines
Similar to other psychedelics, 5-HT2A receptor agonism plays a key role in mediating the psychedelic effects of naturally occurring and synthetic tryptamine psychedelics (Fantegrossi et al. ref. 2008; Halberstadt ref. 2016; Madsen et al. ref. 2019; Vollenweider et al. ref. 1998). Although mediating opposing functional effects on 5-HT2A receptors, the concurrent activation of 5-HT1A receptors has been suggested to contribute to the qualitative effects of tryptamine psychedelics, distinguishing them from phenethylamine psychedelics (Fantegrossi et al. ref. 2008; Halberstadt and Geyer ref. 2011; Nichols ref. 2004, ref. 2016; Winter et al. ref. 2000). Most traditional and novel tryptamine psychedelics bind to 5-HT1A and 5-HT2A receptors with similar affinity. Some tryptamines are slightly more selective for one or the other receptor subtype (Rickli et al. ref. 2016). However, various tryptamine psychedelics have been reported to be inactive at the 5-HT1A receptor in functional assays at relevant concentrations (EC50 > 10 μM) or act as mostly partial agonists with significantly lower potency compared with 5-HT2A receptors, at which tryptamine psychedelics act as moderate to full agonists (Blough et al. ref. 2014; Rickli et al. ref. 2016). At 5-HT2B receptors, traditional and novel tryptamine psychedelics have very heterogeneous profiles, with different potencies and efficacies. For example, 5-methoxy-α-methyltryptamine (5-MeO-αMT) is a potent 5-HT2B receptor full agonist with an EC50 in the low nanomolar range, whereas psilocin and 4-hydroxy-N-methyl-N-ethyltryptamine (4-HO-MET) are inactive at the 5-HT2B receptor (EC50 > 20 μM) (Rickli et al. ref. 2016). Tryptamine designer drugs have been shown to bind to 5-HT2C receptors but with slightly lower affinity compared with 5-HT2A receptors (Rickli et al. ref. 2016). In addition to their primary effects at serotonergic receptors, tryptamines have been shown to bind to various targets in vitro, including adrenergic, dopaminergic, and histaminergic receptors (Klein et al. ref. 2018; Rickli et al. ref. 2016). Furthermore, unlike phenethylamine or lysergamide psychedelics, many tryptamine psychedelics interact with monoamine transporters at pharmacologically relevant concentrations. In addition to some interactions with the DAT and NET for some compounds, tryptamines have the most potent transporter interactions at the SERT (Blough et al. ref. 2014; Cozzi et al. ref. 2009; Rickli et al. ref. 2016). DMT and other tryptamine psychedelics have been reported to elicit 5-HT efflux, suggesting that they are transporter substrates (Blough et al. ref. 2014; Cozzi et al. ref. 2009; Rickli et al. ref. 2016). In contrast, other tryptamine psychedelics, including psilocin, act as transporter inhibitors that are devoid of substrate activity (Rickli et al. ref. 2016). In addition to interactions with transmembrane monoamine transporters, substrate activity at the VMAT has been described for tryptamine psychedelics (Cozzi et al. ref. 2009). Tryptamines are prone to metabolism by MAOs, and MAO inhibitors counteract extensive degradation of tryptamines after oral use (Halberstadt et al. ref. 2012; Ott ref. 1999, ref. 2001; Riba et al. ref. 2015).
Adverse effects of tryptamines
Similar to other psychedelics, tryptamine psychedelics alter perception and can induce psychological disturbances in users, including acute psychosis (Meatherall and Sharma ref. 2003; Nichols ref. 2004, ref. 2016; Shulgin and Shulgin ref. 1997; Taljemark and Johansson ref. 2012). Adverse effects of tryptamine designer drugs include restlessness, disorientation, clouding of consciousness, confusion, hallucinations, amnesia, catalepsy, mydriasis, tachypnea, hypertension, and tachycardia (Alatrash et al. ref. 2006; Itokawa et al. ref. 2007; Jovel et al. ref. 2014; Muller ref. 2004; Smolinske et al. ref. 2005). 5-Methoxy-N,N-diisopropyltryptamine (5-MeO-DiPT) use has been associated with hallucinogen-persisting perception disorder and was proposed to play a role in the development of prolonged delusions (Fuse-Nagase and Nishikawa ref. 2013; Ikeda et al. ref. 2005). In severe cases, the use of tryptamine designer drugs has resulted in acute renal failure and rhabdomyolysis (Alatrash et al. ref. 2006; Jovel et al. ref. 2014). Furthermore, several fatalities after the use of tryptamine designer drugs have been reported (Boland et al. ref. 2005; Sklerov et al. ref. 2005; Tanaka et al. ref. 2006).
Lysergamides
Several derivatives of LSD have been described in the scientific literature, and such derivatives are increasingly emerging as designer drugs (Fig. 9) (Brandt et al. ref. 2016, ref. 2017a, ref. b, ref. 2018, ref. 2019; Shulgin and Shulgin ref. 1997; Troxler and Hofmann ref. 1957). The LSD-derived designer drugs 1-acetyl-LSD (ALD-52), 1-propionyl-LSD (1P-LSD), and 1-butyryl-LSD (1B-LSD) have been shown to be metabolized to LSD in vitro and are thus considered precursors of LSD with very similar effects (Wagmann et al. ref. 2019b). Whereas self-reported effects of some LSD analogs are similar to LSD but with slightly weaker or less pleasurable effects, other LSD analogs have been reported to be distinctively less potent or significantly differ from LSD in terms of effects (Coney et al. ref. 2017; Shulgin and Shulgin ref. 1997).
Mechanism of action of lysergamides
Several LSD-derived designer drugs induce a head twitch response in mice, and pretreatment with a selective 5-HT2A receptor antagonist abolished the 1P-LSD-induced head twitch response (Brandt et al. 2017a; Brandt et al. 2016). This indicates that, similar to LSD, 5-HT2A receptor activation mediates the behavioral effects of LSD analogs (Kraehenmann et al. ref. 2017; Liechti ref. 2017; Preller et al. ref. 2017, ref. 2018). Additionally, 5-HT1A receptor activation likely contributes to the qualitative effects of lysergamide designer drugs similarly to LSD and tryptamine psychedelics (Fantegrossi et al. ref. 2008; Halberstadt and Geyer ref. 2011; Nichols ref. 2004, ref. 2016; Rickli et al. ref. 2016; Winter et al. ref. 2000). In addition to differences in affinity, LSD-derived designer drugs may activate 5-HT2A receptors with lower relative potency compared with LSD, but more research is needed to test this hypothesis (Brandt et al. 2017a). Furthermore, unclear are the ways in which the behavioral effects of lysergamide designer drugs in animals translate to humans.
Adverse effects of lysergamides
Little is known about the adverse effects of lysergamide designer drugs. One case of a 17-year-old male who developed anxiety, hallucinations, restlessness, elevations of blood pressure, palpitations, and tachycardia after ingesting 1P-LSD was reported (Grumann et al. ref. 2019). 1P-LSD was confirmed as an ingredient of the ingested blotter paper but could not be detected in urine or serum samples, despite being sufficiently stable in these matrices. However, LSD was detected in both samples, thus strengthening the assumption that 1P-LSD is readily metabolized to LSD in humans (Grumann et al. ref. 2019). The patient reported that he recently used the stimulant phenmetrazine derivative 3-FPM. The low serum concentrations of 3-FPM that were detected at the time of hospital admission are, however, not expected to result in acute effects (Grumann et al. ref. 2019). The symptoms of this 1P-LSD intoxication case are consistent with reported adverse effects of LSD, which is known to potentially cause psychological disturbances and moderately increase body temperature, blood pressure, and heart rate (Dolder et al. ref. 2016; Schmid et al. ref. 2015). Acute physiological adverse effects of LSD include difficulty concentrating, imbalance, feelings of exhaustion, dizziness, headache, dry mouth, lack of appetite, and nausea (Dolder et al. ref. 2016; Schmid et al. ref. 2015). Nichols and Grob recently reviewed the risk of LSD toxicity in users, which they concluded was very low (Nichols and Grob ref. 2018). The few cases of fatality that were attributed to LSD toxicity were either associated with massive overdoses or physical restraint, or they were potentially caused by drugs that remained undetected in the toxicological analysis (Nichols and Grob ref. 2018). Currently, no evidence suggests that any of the currently available lysergamide designer drugs are significantly more toxic than LSD.
Performance-enhancing designer drugs
Designer doping agents have become increasingly popular outside of the professional athletic community and include anabolic steroids, peptide hormones, growth factor mimetics, and hormone and metabolic modulators (Joseph and Parr ref. 2015; Poplawska and Blazewicz ref. 2019; Rahnema et al. ref. 2015; Weber et al. ref. 2017). Such substances are mainly used for performance and image enhancement, exerting effects through several different mechanisms within the hormone system (Graham et al. ref. 2009; Kicman ref. 2008). Adverse effects that are associated with performance-enhancing designer drugs include secondary hypogonadism, gynecomastia, infertility, hypertension, ischemic stroke, cardiotoxicity, hepatotoxicity, and renal failure (Rahnema et al. ref. 2015). In addition to substances that are taken to enhance athletic performance and appearance, designer drugs that are taken to enhance sexual performance, such as phosphodiesterase-5 inhibitors with no known safety profile, have also appeared. These substances may potentially induce visual disturbances or severe drug–drug interactions (Venhuis et al. ref. 2008).
Miscellaneous risks associated with designer drug use
In addition to adverse effects that are associated with specific classes of designer drugs, some general risks are essentially the same as for traditional drugs of abuse. For example, quality assurance is not guaranteed for clandestine designer drugs. A lack of information about purity, mislabeling, pharmaceutical impurities, and hazardous cutting agents can pose a risk for drug users. A series of patients who presented to a hospital with coagulopathy and bleeding diathesis that were related to long-acting anticoagulant rodenticide adulterants of synthetic cannabinoids exemplifies their potentially fatal consequences (Devgun et al. ref. 2019; Kelkar et al. ref. 2018). Potentially severe drug–drug interactions are a risk when more than one substance is used, including prescription medications (Contrucci et al. ref. 2020; Inan et al. ref. 2020). Byproducts and impurities can pose such risks as septum perforation when insufflated or necrotic ulcers and infections when injected (Lafferty et al. ref. 2016; Parks et al. ref. 2015). Hallucinogen-persisting perception disorder has been associated with psychedelics, cannabinoids, and psychostimulants, manifesting in prolonged or reoccurring perceptual symptoms (Ikeda et al. ref. 2005; Orsolini et al. ref. 2017; Skryabin et al. ref. 2019). The neurological and psychological changes that are associated with designer drugs can impair safe driving, and driving under the influence can severely jeopardize traffic safety (Adamowicz and Lechowicz ref. 2015; Maas et al. ref. 2015; Musshoff et al. ref. 2014).
Concluding remarks
Designer drugs are often used in combination with other substances, thus hindering precise evaluations of the degree of involvement of individual substances to clinical toxicity in patients. Furthermore, designer drugs may remain undetected by routine drug screenings. Nevertheless, the pharmacological and toxicological profiles of most designer drug classes are similar to their related traditional drugs of abuse. Stimulants primarily act as substrates or inhibitors of monoamine transporters. Intoxication with stimulants mostly manifests as sympathomimetic adverse effects, the treatment of which is mainly supportive. Benzodiazepines may be given to control agitation, hypertension, and convulsions. Certain stimulants, including MDMA, have a marked serotonergic profile. Their associated adverse effects, such as serotonin syndrome, can be potentially severe clinical complications. Agonism at μ-opioid receptors mediates the main pharmacological effects of opioids, and GABAA and GABAB receptors drive the effects of designer benzodiazepines and GHB analogs, respectively. Sedatives, including synthetic opioids and GHB analogs, pose a risk of cardiorespiratory arrest, especially when they are used in combination with other depressants, such as alcohol and benzodiazepines. Initial patient care should focus on protecting the airways and maintaining breathing and circulation. Naloxone is an effective antidote to opioid toxicity. Dissociative designer drugs act as NMDA receptor antagonists and induce adverse effects that are similar to the dissociative anesthetics ketamine and PCP. Compared with Δ9-THC, synthetic cannabinoids act as more potent and effective agonists of CB1 and CB2 receptors, but the predominance of CB1 receptors in the central nervous system suggests that they mainly mediate the psychoactive effects. Compared with cannabis, effects of synthetic cannabinoids are less desirable, and adverse effects are more severe. Serotonergic psychedelics alter perception and cognition mainly through 5-HT2A receptor agonism. In addition to psychological disturbances, psychedelics may induce physical adverse effects, which are usually short-lived. Rarely, designer drug use can lead to severe psychiatric and physical complications and even death. Single-drug use and more precise knowledge of substance identity, potency, and purity can reduce the risks of designer drug use.
Supplementary Materials
References
- SM Aarde, MA Taffe. Predicting the abuse liability of entactogen-class, new and emerging psychoactive substances via preclinical models of drug self-administration. Curr Top Behav Neurosci, 2017. [DOI | PubMed]
- P Adamowicz. Fatal intoxication with synthetic cannabinoid MDMB-CHMICA. Forensic Sci Int, 2016. [DOI | PubMed]
- P Adamowicz, W Lechowicz. The influence of synthetic cannabinoid UR-144 on human psychomotor performance–a case report demonstrating road traffic risks. Traffic Inj Prev, 2015. [DOI | PubMed]
- P Adamowicz, D Zuba. Fatal intoxication with methoxetamine. J Forensic Sci, 2015. [DOI | PubMed]
- P Adamowicz, D Zuba, B Byrska. Fatal intoxication with 3-methyl-N-methylcathinone (3-MMC) and 5-(2-aminopropyl)benzofuran (5-APB). Forensic Sci Int, 2014. [DOI | PubMed]
- P Adamowicz, J Gieron, D Gil, W Lechowicz, A Skulska, B Tokarczyk. 3-Methylmethcathinone-interpretation of blood concentrations based on analysis of 95 cases. J Anal Toxicol, 2016. [DOI | PubMed]
- P Adamowicz, J Gieron, D Gil, W Lechowicz, A Skulska, B Tokarczyk. The effects of synthetic cannabinoid UR-144 on the human body—a review of 39 cases. Forensic Sci Int, 2017. [DOI | PubMed]
- P Adamowicz, E Meissner, M Maslanka. Fatal intoxication with new synthetic cannabinoids AMB-FUBINACA and EMB-FUBINACA. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- DA Adedinsewo, O Odewole, T Todd. Acute rhabdomyolysis following synthetic cannabinoid ingestion. N Am J Med Sci, 2016. [DOI | PubMed]
- H Akram, C Mokrysz, HV Curran. What are the psychological effects of using synthetic cannabinoids? A systematic review. J Psychopharmacol, 2019. [DOI | PubMed]
- G Alatrash, NS Majhail, JC Pile. Rhabdomyolysis after ingestion of "foxy", a hallucinogenic tryptamine derivative. Mayo Clin Proc, 2006. [DOI | PubMed]
- S Alhadi, A Tiwari, R Vohra, R Gerona, J Acharya, K Bilello. High times, low sats: diffuse pulmonary infiltrates associated with chronic synthetic cannabinoid use. J Med Toxicol, 2013. [DOI | PubMed]
- R Al-Hasani, MR Bruchas. Molecular mechanisms of opioid receptor-dependent signaling and behavior. Anesthesiology, 2011. [DOI | PubMed]
- A Alipour, PB Patel, Z Shabbir, S Gabrielson. Review of the many faces of synthetic cannabinoid toxicities. Ment Health Clin, 2019. [DOI | PubMed]
- GA Alles, GA Feigen. Comparative physiological actions of phenyl-, thienyl- and furylisopropylamines. J Pharmacol Exp Ther, 1941
- A Al-Matrouk, M Alqallaf, A AlShemmeri, H BoJbarah. Identification of synthetic cannabinoids that were seized, consumed, or associated with deaths in Kuwait in 2018 using GC–MS and LC–MS–MS analysis. Forensic Sci Int, 2019. [DOI | PubMed]
- MH Alon, MO Saint-Fleur. Synthetic cannabinoid induced acute respiratory depression: case series and literature review. Respir Med Case Rep, 2017. [DOI | PubMed]
- M Altintas, L Inanc, GA Oruc, S Arpacioglu, H Gulec. Clinical characteristics of synthetic cannabinoid-induced psychosis in relation to schizophrenia: a single-center cross-sectional analysis of concurrently hospitalized patients. Neuropsychiatr Dis Treat, 2016. [DOI | PubMed]
- JB Ambrose, HD Bennett, HS Lee, SA Josephson. Cerebral vasculopathy after 4-bromo-2,5-dimethoxyphenethylamine ingestion. Neurologist, 2010. [DOI | PubMed]
- T Amoroso, M Workman. Treating posttraumatic stress disorder with MDMA-assisted psychotherapy: a preliminary meta-analysis and comparison to prolonged exposure therapy. J Psychopharmacol, 2016. [DOI | PubMed]
- M Andersson, A Kjellgren. The slippery slope of flubromazolam: experiences of a novel psychoactive benzodiazepine as discussed on a Swedish online forum. Nord Stud Alcohol Drugs, 2017. [DOI]
- V Andreu, A Mas, M Bruguera, JM Salmerón, V Moreno, S Nogué, J Rodés. Ecstasy: a common cause of severe acute hepatotoxicity. J Hepatol, 1998. [DOI | PubMed]
- V Angerer, S Jacobi, F Franz, V Auwärter, J Pietsch. Three fatalities associated with the synthetic cannabinoids 5F-ADB, 5F-PB-22, and AB-CHMINACA. Forensic Sci Int, 2017. [DOI | PubMed]
- NA Anis, SC Berry, NR Burton, D Lodge. The dissociative anaesthetics, ketamine and phencyclidine, selectively reduce excitation of central mammalian neurones by N-methyl-aspartate. Br J Pharmacol, 1983. [DOI | PubMed]
- S Anne, R Tse, AD Cala. A fatal case of isolated methiopropamine (1-(thiophen-2-yl)-2-methylaminopropane) toxicity: a case report. Am J Forensic Med Pathol, 2015. [DOI | PubMed]
- AM Araújo, F Carvalho, MDL Bastos, P Guedes De Pinho, M Carvalho. The hallucinogenic world of tryptamines: an updated review. Arch Toxicol, 2015. [DOI | PubMed]
- MD Arbo, ML Bastos, HF Carmo. Piperazine compounds as drugs of abuse. Drug Alcohol Depend, 2012. [DOI | PubMed]
- MD Arbo, S Melega, R Stöber, M Schug, E Rempel, J Rahnenführer, P Godoy, R Reif, C Cadenas, BM De Lourdes, H Carmo, JG Hengstler. Hepatotoxicity of piperazine designer drugs: up-regulation of key enzymes of cholesterol and lipid biosynthesis. Arch Toxicol, 2016. [DOI | PubMed]
- MD Arbo, R Silva, DJ Barbosa, D Dias da Silva, SP Silva, JP Teixeira, ML Bastos, H Carmo. In vitro neurotoxicity evaluation of piperazine designer drugs in differentiated human neuroblastoma SH-SY5Y cells. J Appl Toxicol, 2016. [DOI | PubMed]
- JR Argamany, KR Reveles, B Duhon. Synthetic cannabinoid hyperemesis resulting in rhabdomyolysis and acute renal failure. Am J Emerg Med, 2016. [DOI]
- P Armenian, A Olson, A Anaya, A Kurtz, R Ruegner, RR Gerona. Fentanyl and a novel synthetic opioid U-47700 masquerading as street "Norco" in Central California: a case report. Ann Emerg Med, 2017. [DOI | PubMed]
- P Armenian, M Darracq, J Gevorkyan, S Clark, B Kaye, NP Brandehoff. Intoxication from the novel synthetic cannabinoids AB-PINACA and ADB-PINACA: a case series and review of the literature. Neuropharmacology, 2018. [DOI | PubMed]
- P Armenian, KT Vo, J Barr-Walker, KL Lynch. Fentanyl, fentanyl analogs and novel synthetic opioids: a comprehensive review. Neuropharmacology, 2018. [DOI | PubMed]
- F Armstrong, MT McCurdy, MS Heavner. Synthetic cannabinoid-associated multiple organ failure: case series and literature review. Pharmacotherapy, 2019. [DOI | PubMed]
- BK Atwood, J Huffman, A Straiker, K Mackie. JWH018, a common constituent of ‘Spice’ herbal blends, is a potent and efficacious cannabinoid CB receptor agonist. Br J Pharmacol, 2010. [DOI | PubMed]
- G Aydin, B Bakar. Delayed intracerebral hemorrhage after synthetic cannabis (Bonsai) abuse; case report and literature review. Bull Emerg Trauma, 2019. [DOI | PubMed]
- MA Babi, CP Robinson, CB Maciel. A spicy status: synthetic cannabinoid (spice) use and new-onset refractory status epilepticus–a case report and review of the literature. SAGE Open Med Case Rep, 2017. [DOI]
- M Bäckberg, O Beck, P Hulten, J Rosengren-Holmberg, A Helander. Intoxications of the new psychoactive substance 5-(2-aminopropyl)indole (5-IT): a case series from the Swedish STRIDA project. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- M Bäckberg, O Beck, A Helander. Phencyclidine analog use in Sweden–intoxication cases involving 3-MeO-PCP and 4-MeO-PCP from the STRIDA project. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- M Bäckberg, O Beck, KH Jonsson, A Helander. Opioid intoxications involving butyrfentanyl, 4-fluorobutyrfentanyl, and fentanyl from the Swedish STRIDA project. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- M Bäckberg, E Lindeman, O Beck, A Helander. Characteristics of analytically confirmed 3-MMC-related intoxications from the Swedish STRIDA project. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- M Bäckberg, J Westerbergh, O Beck, A Helander. Adverse events related to the new psychoactive substance 3-fluorophenmetrazine—results from the Swedish STRIDA project. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- M Bäckberg, L Tworek, O Beck, A Helander. Analytically confirmed intoxications involving MDMB-CHMICA from the STRIDA project. J Med Toxicol, 2017. [DOI | PubMed]
- M Bäckberg, M Pettersson Bergstrand, O Beck, A Helander. Occurrence and time course of NPS benzodiazepines in Sweden–results from intoxication cases in the STRIDA project. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- K Bailey, L Richards-Waugh, D Clay, M Gebhardt, H Mahmoud, JC Kraner. Fatality involving the ingestion of phenazepam and poppy seed tea. J Anal Toxicol, 2010. [DOI | PubMed]
- GP Bailey, JH Ho, S Hudson, A Dines, JR Archer, PI Dargan, DM Wood. Nopaine no gain: recreational ethylphenidate toxicity. Clin Toxicol, 2015. [DOI]
- E Bakota, C Arndt, AA Romoser, SK Wilson. Fatal intoxication involving 3-MeO–PCP: a case report and validated method. J Anal Toxicol, 2016. [DOI | PubMed]
- BA Baldo. Opioid analgesic drugs and serotonin toxicity (syndrome): mechanisms, animal models, and links to clinical effects. Arch Toxicol, 2018. [DOI | PubMed]
- C Balmelli, H Kupferschmidt, K Rentsch, M Schneemann. Tödliches Hirnödem nach Einnahme von Ecstasy und Benzylpiperazin. Dtsch Med Wochenschr, 2001. [DOI | PubMed]
- SD Banister, M Connor. The chemistry and pharmacology of synthetic cannabinoid receptor agonists as new psychoactive substances: origins. Handb Exp Pharmacol, 2018. [DOI | PubMed]
- SD Banister, M Moir, J Stuart, RC Kevin, KE Wood, M Longworth, SM Wilkinson, C Beinat, AS Buchanan, M Glass, M Connor, IS McGregor, M Kassiou. Pharmacology of indole and indazole synthetic cannabinoid designer drugs AB-FUBINACA, ADB-FUBINACA, AB-PINACA, ADB-PINACA, 5F-AB-PINACA, 5F-ADB-PINACA, ADBICA, and 5F-ADBICA. ACS Chem Neurosci, 2015. [DOI | PubMed]
- SD Banister, J Stuart, RC Kevin, A Edington, M Longworth, SM Wilkinson, C Beinat, AS Buchanan, DE Hibbs, M Glass, M Connor, IS McGregor, M Kassiou. Effects of bioisosteric fluorine in synthetic cannabinoid designer drugs JWH-018, AM-2201, UR-144, XLR-11, PB-22, 5F-PB-22, APICA, and STS-135. ACS Chem Neurosci, 2015. [DOI | PubMed]
- SD Banister, M Longworth, R Kevin, S Sachdev, M Santiago, J Stuart, JB Mack, M Glass, IS McGregor, M Connor, M Kassiou. Pharmacology of valinate and tert-leucinate synthetic cannabinoids 5F-AMBICA, 5F-AMB, 5F-ADB, AMB-FUBINACA, MDMB-FUBINACA, MDMB-CHMICA, and their analogues. ACS Chem Neurosci, 2016. [DOI | PubMed]
- SD Banister, A Adams, RC Kevin, C Macdonald, M Glass, R Boyd, M Connor, IS McGregor, CM Havel, SJ Bright, MV Vilamala, CG Lladanosa, MJ Barratt, RR Gerona. Synthesis and pharmacology of new psychoactive substance 5F-CUMYL-P7AICA, a scaffold-hopping analog of synthetic cannabinoid receptor agonists 5F-CUMYL-PICA and 5F-CUMYL-PINACA. Drug Test Anal, 2019. [DOI | PubMed]
- SD Banister, RC Kevin, L Martin, A Adams, C Macdonald, JJ Manning, R Boyd, M Cunningham, MY Stevens, IS McGregor, M Glass, M Connor, RR Gerona. The chemistry and pharmacology of putative synthetic cannabinoid receptor agonist (SCRA) new psychoactive substances (NPS) 5F-PY-PICA, 5F-PY-PINACA, and their analogs. Drug Test Anal, 2019. [DOI | PubMed]
- M Barann, UM Stamer, M Lyutenska, F Stuber, H Bonisch, B Urban. Effects of opioids on human serotonin transporters. Naunyn Schmiedeberg’s Arch Pharmacol, 2015. [DOI | PubMed]
- L Barrios, H Grison-Hernando, D Boels, R Bouquie, C Monteil-Ganiere, R Clement. Death following ingestion of methylone. Int J Legal Med, 2016. [DOI | PubMed]
- A Bassir Nia, CL Mann, S Spriggs, DR DeFrancisco, S Carbonaro, L Parvez, II Galynker, CA Perkel, YL Hurd. The relevance of sex in the association of synthetic cannabinoid use with psychosis and agitation in an inpatient population. J Clin Psychiatry, 2019. [DOI]
- MH Baumann, MA Ayestas, CM Dersch, A Brockington, KC Rice, RB Rothman. Effects of phentermine and fenfluramine on extracellular dopamine and serotonin in rat nucleus accumbens: therapeutic implications. Synapse, 2000. [DOI | PubMed]
- MH Baumann, RD Clark, AG Budzynski, JS Partilla, BE Blough, RB Rothman. N-substituted piperazines abused by humans mimic the molecular mechanism of 3,4-methylenedioxymethamphetamine (MDMA, or ‘Ecstasy’). Neuropsychopharmacology, 2005. [DOI | PubMed]
- MH Baumann, MA Ayestas, JS Partilla, JR Sink, AT Shulgin, PF Daley, SD Brandt, RB Rothman, AE Ruoho, NV Cozzi. The designer methcathinone analogs, mephedrone and methylone, are substrates for monoamine transporters in brain tissue. Neuropsychopharmacology, 2012. [DOI | PubMed]
- MH Baumann, JS Partilla, KR Lehner. Psychoactive "bath salts": not so soothing. Eur J Pharmacol, 2013. [DOI | PubMed]
- MH Baumann, S Majumdar, V Le Rouzic, A Hunkele, R Uprety, XP Huang, J Xu, BL Roth, YX Pan, GW Pasternak. Pharmacological characterization of novel synthetic opioids (NSO) found in the recreational drug marketplace. Neuropharmacology, 2018. [DOI | PubMed]
- T Bay, LF Eghorn, AB Klein, P Wellendorph. GHB receptor targets in the CNS: focus on high-affinity binding sites. Biochem Pharmacol, 2014. [DOI | PubMed]
- VS Bebarta, S Ramirez, SM Varney. Complication of spice use in a deployed combat setting-seizure while on duty. Am J Addict, 2012. [DOI | PubMed]
- O Beck, L Franzén, M Bäckberg, P Signell, A Helander. Intoxications involving MDPV in Sweden during 2010–2014: results from the STRIDA project. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- O Beck, L Franzén, M Bäckberg, P Signell, A Helander. Toxicity evaluation of α-pyrrolidinovalerophenone (α-PVP): results from intoxication cases within the STRIDA project. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- G Behonick, KG Shanks, DJ Firchau, G Mathur, CF Lynch, M Nashelsky, DJ Jaskierny, C Meroueh. Four postmortem case reports with quantitative detection of the synthetic cannabinoid, 5F-PB-22. J Anal Toxicol, 2014. [DOI | PubMed]
- MGK Benesch, SJ Iqbal. Novel psychoactive substances: overdose of 3-fluorophenmetrazine (3-FPM) and etizolam in a 33-year-old man. BMJ Case Rep, 2018. [DOI | PubMed]
- DM Benford, JP Caplan. Psychiatric sequelae of Spice, K2, and synthetic cannabinoid receptor agonists. Psychosomatics, 2011. [DOI | PubMed]
- EA Berkowitz, TS Henry, S Veeraraghavan, GW Staton, AA Gal. Pulmonary effects of synthetic marijuana: chest radiography and CT findings. AJR Am J Roentgenol, 2015. [DOI | PubMed]
- ME Bernson-Leung, LY Leung, S Kumar. Synthetic cannabis and acute ischemic stroke. J Stroke Cerebrovasc Dis, 2014. [DOI | PubMed]
- CS Berry-Caban, J Ee, V Ingram, CE Berry, EH Kim. Synthetic cannabinoid overdose in a 20-year-old male US soldier. Subst Abus, 2013. [DOI | PubMed]
- GK Bhanushali, G Jain, H Fatima, LJ Leisch, D Thornley-Brown. AKI associated with synthetic cannabinoids: a case series. Clin J Am Soc Nephrol, 2013. [DOI | PubMed]
- BL Bick, JH Szostek, TF Mangan. Synthetic cannabinoid leading to cannabinoid hyperemesis syndrome. Mayo Clin Proc, 2014. [DOI | PubMed]
- C Bingham, M Beaman, AJ Nicholls, PP Anthony. Necrotizing renal vasculopathy resulting in chronic renal failure after ingestion of methamphetamine and 3,4-methylenedioxymethamphetamine (‘ecstasy’). Nephrol Dial Transplant, 1998. [DOI | PubMed]
- FF Blicke, JH Burckhalter. α-Thienylaminoalkanes. J Am Chem Soc, 1942. [DOI]
- BE Blough, A Landavazo, AM Decker, JS Partilla, MH Baumann, RB Rothman. Interaction of psychoactive tryptamines with biogenic amine transporters and serotonin receptor subtypes. Psychopharmacology, 2014. [DOI | PubMed]
- DM Boland, W Andollo, GW Hime, WL Hearn. Fatality due to acute α-methyltryptamine intoxication. J Anal Toxicol, 2005. [DOI | PubMed]
- DM Boland, LJ Reidy, JM Seither, JM Radtke, EO Lew. Forty-three fatalities involving the synthetic cannabinoid, 5-fluoro-ADB: forensic pathology and toxicology implications. J Forensic Sci, 2019. [DOI | PubMed]
- S Bonaccorso, A Metastasio, A Ricciardi, N Stewart, L Jamal, NU Rujully, C Theleritis, S Ferracuti, G Ducci, F Schifano. Synthetic cannabinoid use in a case series of patients with psychosis presenting to acute psychiatric settings: clinical presentation and management issues. Brain Sci, 2018. [DOI]
- HA Borek, CP Holstege. Hyperthermia and multiorgan failure after abuse of “bath salts” containing 3,4-methylenedioxypyrovalerone. Ann Emerg Med, 2012. [DOI | PubMed]
- A Bosak, F LoVecchio, M Levine. Recurrent seizures and serotonin syndrome following "2C-I" ingestion. J Med Toxicol, 2013. [DOI | PubMed]
- MG Bossong, TM Brunt, JP Van Dijk, SM Rigter, J Hoek, HM Goldschmidt, RJ Niesink. mCPP: an undesired addition to the ecstasy market. J Psychopharmacol, 2010. [DOI | PubMed]
- C Boulanger-Gobeil, M St-Onge, M Laliberte, PL Auger. Seizures and hyponatremia related to ethcathinone and methylone poisoning. J Med Toxicol, 2012. [DOI | PubMed]
- MR Braden, JC Parrish, JC Naylor, DE Nichols. Molecular interaction of serotonin 5-HT2A receptor residues Phe 339(6.51) and Phe340(6.52) with superpotent N-benzyl phenethylamine agonists. Mol Pharmacol, 2006. [DOI | PubMed]
- SD Brandt, MH Baumann, JS Partilla, PV Kavanagh, JD Power, B Talbot, B Twamley, O Mahony, J O’Brien, SP Elliott, RP Archer, J Patrick, K Singh, NM Dempster, SH Cosbey. Characterization of a novel and potentially lethal designer drug (±)-cis-para-methyl-4-methylaminorex (4,4′-DMAR, or ‘Serotoni’). Drug Test Anal, 2014. [DOI | PubMed]
- SD Brandt, PV Kavanagh, F Westphal, A Stratford, SP Elliott, K Hoang, J Wallach, AL Halberstadt. Return of the lysergamides. Part I: Analytical and behavioural characterization of 1-propionyl-d-lysergic acid diethylamide (1P-LSD). Drug Test Anal, 2016. [DOI | PubMed]
- SD Brandt, PV Kavanagh, F Westphal, SP Elliott, J Wallach, T Colestock, TE Burrow, SJ Chapman, A Stratford, DE Nichols, AL Halberstadt. Return of the lysergamides. Part II: Analytical and behavioural characterization of N6-allyl-6-norlysergic acid diethylamide (AL-LAD) and (2ʹS,4ʹS)-lysergic acid 2,4-dimethylazetidide (LSZ). Drug Test Anal, 2017. [DOI | PubMed]
- SD Brandt, PV Kavanagh, F Westphal, SP Elliott, J Wallach, A Stratford, DE Nichols, AL Halberstadt. Return of the lysergamides. Part III: Analytical characterization of N6-ethyl-6-norlysergic acid diethylamide (ETH-LAD) and 1-propionyl ETH-LAD (1P-ETH-LAD). Drug Test Anal, 2017. [DOI | PubMed]
- SD Brandt, PV Kavanagh, B Twamley, F Westphal, SP Elliott, J Wallach, A Stratford, LM Klein, JD McCorvy, DE Nichols, AL Halberstadt. Return of the lysergamides. Part IV: Analytical and pharmacological characterization of lysergic acid morpholide (LSM-775). Drug Test Anal, 2018. [DOI | PubMed]
- SD Brandt, PV Kavanagh, F Westphal, A Stratford, SP Elliott, G Dowling, J Wallach, AL Halberstadt. Return of the lysergamides. Part V: Analytical and behavioural characterization of 1-butanoyl-d-lysergic acid diethylamide (1B-LSD). Drug Test Anal, 2019. [DOI | PubMed]
- R Brennan, MC Van Hout. Gamma-hydroxybutyrate (GHB): a scoping review of pharmacology, toxicology, motives for use, and user groups. J Psychoactive Drugs, 2014. [DOI | PubMed]
- PC Brown, J Alfonso, ME Dunn. Gamma hydroxybutyrate use: exploring the influence of outcome expectancies through memory modeling. Am J Addict, 2011. [DOI | PubMed]
- MJ Burish, KL Thoren, M Madou, S Toossi, M Shah. Hallucinogens causing seizures? A case report of the synthetic amphetamine 2,5-dimethoxy-4-chloroamphetamine. Neurohospitalist, 2015. [DOI | PubMed]
- G Burns, RT DeRienz, DD Baker, M Casavant, HA Spiller. Could chest wall rigidity be a factor in rapid death from illicit fentanyl abuse?. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- FP Busardò, AW Jones. GHB pharmacology and toxicology: acute intoxication, concentrations in blood and urine in forensic cases and treatment of the withdrawal syndrome. Curr Neuropharmacol, 2015. [DOI | PubMed]
- FP Busardò, C Kyriakou, S Napoletano, E Marinelli, S Zaami. Mephedrone related fatalities: a review. Eur Rev Med Pharmacol Sci, 2015. [PubMed]
- GL Buser, RR Gerona, BZ Horowitz, KP Vian, ML Troxell, RG Hendrickson, DC Houghton, D Rozansky, SW Su, RF Leman. Acute kidney injury associated with smoking synthetic cannabinoid. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- GA Campbell, MH Rosner. The agony of ecstasy: MDMA (3,4-methylenedioxymethamphetamine) and the kidney. Clin J Am Soc Nephrol, 2008. [DOI | PubMed]
- H Canning, D Goff, MJ Leach, AA Miller, JE Tateson, PL Wheatley. The involvement of dopamine in the central actions of bupropion, a new antidepressant [proceedings]. Br J Pharmacol, 1979. [PubMed]
- MA Carai, G Colombo, G Brunetti, S Melis, S Serra, G Vacca, S Mastinu, AM Pistuddi, C Solinas, G Cignarella, G Minardi, GL Gessa. Role of GABAB receptors in the sedative/hypnotic effect of γ-hydroxybutyric acid. Eur J Pharmacol, 2001. [DOI | PubMed]
- PN Carbone, DL Carbone, SD Carstairs, SA Luzi. Sudden cardiac death associated with methylone use. Am J Forensic Med Pathol, 2013. [DOI | PubMed]
- RL Carhart-Harris, M Bolstridge, CMJ Day, J Rucker, R Watts, DE Erritzoe, M Kaelen, B Giribaldi, M Bloomfield, S Pilling, JA Rickard, B Forbes, A Feilding, D Taylor, HV Curran, DJ Nutt. Psilocybin with psychological support for treatment-resistant depression: six-month follow-up. Psychopharmacology, 2018. [DOI | PubMed]
- JE Carpenter, BP Murray, C Dunkley, ZN Kazzi, MH Gittinger. Designer benzodiazepines: a report of exposures recorded in the National Poison Data System, 2014–2017. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- LP Carter, W Chen, H Wu, AK Mehta, RJ Hernandez, MK Ticku, A Coop, W Koek, CP France. Comparison of the behavioral effects of gamma-hydroxybutyric acid (GHB) and its 4-methyl-substituted analog, gamma-hydroxyvaleric acid (GHV). Drug Alcohol Depend, 2005. [DOI | PubMed]
- LP Carter, W Koek, CP France. Behavioral analyses of GHB: receptor mechanisms. Pharmacol Ther, 2009. [DOI | PubMed]
- M Carvalho, H Pontes, F Remiao, ML Bastos, F Carvalho. Mechanisms underlying the hepatotoxic effects of ecstasy. Curr Pharm Biotechnol, 2010. [DOI | PubMed]
- M Carvalho, H Carmo, VM Costa, JP Capela, H Pontes, F Remião, F Carvalho, B MeL. Toxicity of amphetamines: an update. Arch Toxicol, 2012. [DOI | PubMed]
- PE Castillo, TJ Younts, AE Chavez, Y Hashimotodani. Endocannabinoid signaling and synaptic function. Neuron, 2012. [DOI | PubMed]
- LD Chait, EH Uhlenhuth, CE Johanson. Reinforcing and subjective effects of several anorectics in normal human volunteers. J Pharmacol Exp Ther, 1987. [PubMed]
- WL Chan, DM Wood, S Hudson, PI Dargan. Acute psychosis associated with recreational use of benzofuran 6-(2-aminopropyl)benzofuran (6-APB) and cannabis. J Med Toxicol, 2013. [DOI | PubMed]
- P Charbogne, BL Kieffer, K Befort. 15 years of genetic approaches in vivo for addiction research: opioid receptor and peptide gene knockout in mouse models of drug abuse. Neuropharmacology, 2014. [DOI | PubMed]
- S Chiappini, H Claridge, JM Corkery, C Goodair, B Loi, F Schifano. Methoxetamine-related deaths in the UK: an overview. Hum Psychopharmacol, 2015. [DOI | PubMed]
- T Chinnadurai, S Shrestha, R Ayinla. A curious case of inhalation fever caused by synthetic cannabinoid. Am J Case Rep, 2016. [DOI | PubMed]
- PS Chu, SC Kwok, KM Lam, TY Chu, SW Chan, CW Man, WK Ma, KL Chui, MK Yiu, YC Chan, ML Tse, FL Lau. ‘Street ketamine’-associated bladder dysfunction: a report of ten cases. Hong Kong Med J, 2007. [PubMed]
- BC Clark, J Georgekutty, CI Berul. Myocardial ischemia secondary to synthetic cannabinoid (K2) use in pediatric patients. J Pediatr, 2015. [DOI | PubMed]
- EE Codd, RP Shank, JJ Schupsky, RB Raffa. Serotonin and norepinephrine uptake inhibiting activity of centrally acting analgesics: structural determinants and role in antinociception. J Pharmacol Exp Ther, 1995. [PubMed]
- MI Colado, TK Murray, AR Green. 5-HT loss in rat brain following 3,4-methylenedioxymethamphetamine (MDMA), p-chloroamphetamine and fenfluramine administration and effects of chlormethiazole and dizocilpine. Br J Pharmacol, 1993. [DOI | PubMed]
- JB Cole, JF Dunbar, SA McIntire, WE Regelmann, TM Slusher. Butyrfentanyl overdose resulting in diffuse alveolar hemorrhage. Pediatrics, 2015. [DOI | PubMed]
- M Concheiro, R Chesser, J Pardi, G Cooper. Postmortem toxicology of new synthetic opioids. Front Pharmacol, 2018. [DOI | PubMed]
- LD Coney, LJ Maier, JA Ferris, AR Winstock, MJ Barratt. Genie in a blotter: a comparative study of LSD and LSD analogues’ effects and user profile. Hum Psychopharmacol, 2017. [DOI]
- RR Contrucci, TM Brunt, F Inan, EJF Franssen, L Hondebrink. Synthetic cathinones and their potential interactions with prescription drugs. Ther Drug Monit, 2020. [DOI | PubMed]
- V Coopman, P Blanckaert, G Van Parys, S Van Calenbergh, J Cordonnier. A case of acute intoxication due to combined use of fentanyl and 3,4-dichloro-N-[2-(dimethylamino)cyclohexyl]-N-methylbenzamide (U-47700). Forensic Sci Int, 2016. [DOI | PubMed]
- V Coopman, J Cordonnier, M De Leeuw, V Cirimele. Ocfentanil overdose fatality in the recreational drug scene. Forensic Sci Int, 2016. [DOI | PubMed]
- M Coppola, R Mondola. 5-Iodo-2-aminoindan (5-IAI): chemistry, pharmacology, and toxicology of a research chemical producing MDMA-like effects. Toxicol Lett, 2013. [DOI | PubMed]
- M Coppola, R Mondola. A new stimulant of abuse: 5-(2-aminopropyl)indole. Am J Psychiatry, 2013. [DOI | PubMed]
- JM Corkery, S Elliott, F Schifano, O Corazza, AH Ghodse. MDAI (5,6-methylenedioxy-2-aminoindane; 6,7-dihydro-5H-cyclopenta[f][1,3]benzodioxol-6-amine; ‘sparkle’; ‘mindy’) toxicity: a brief overview and update. Hum Psychopharmacol, 2013. [DOI | PubMed]
- JM Corkery, B Loi, H Claridge, C Goodair, O Corazza, S Elliott, F Schifano. Gamma hydroxybutyrate (GHB), gamma butyrolactone (GBL) and 1,4-butanediol (1,4-BD; BDO): a literature review with a focus on UK fatalities related to non-medical use. Neurosci Biobehav Rev, 2015. [DOI | PubMed]
- S Cosbey, S Kirk, M McNaul, L Peters, B Prentice, A Quinn, SP Elliott, SD Brandt, RP Archer. Multiple fatalities involving a new designer drug: para-methyl-4-methylaminorex. J Anal Toxicol, 2014. [DOI | PubMed]
- NV Cozzi, A Gopalakrishnan, LL Anderson, JT Feih, AT Shulgin, PF Daley, AE Ruoho. Dimethyltryptamine and other hallucinogenic tryptamines exhibit substrate behavior at the serotonin uptake transporter and the vesicle monoamine transporter. J Neural Transm (Vienna), 2009. [DOI | PubMed]
- ML Crichton, CF Shenton, G Drummond, LJ Beer, LN Seetohul, PD Maskell. Analysis of phenazepam and 3-hydroxyphenazepam in post-mortem fluids and tissues. Drug Test Anal, 2015. [DOI | PubMed]
- V Crunelli, Z Emri, N Leresche. Unravelling the brain targets of γ-hydroxybutyric acid. Curr Opin Pharmacol, 2006. [DOI | PubMed]
- G Cunningham. Diethylpropion in the treatment of obesity. Br J Gen Pract, 1963
- M Cunningham. Ecstasy-induced rhabdomyolysis and its role in the development of acute renal failure. Intensive Crit Care Nurs, 1997. [DOI | PubMed]
- SM Cunningham, NA Haikal, JC Kraner. Fatal intoxication with acetyl fentanyl. J Forensic Sci, 2016. [DOI | PubMed]
- B Curtis, P Kemp, L Harty, C Choi, D Christensen. Postmortem identification and quantitation of 2,5-dimethoxy-4-n-propylthiophenethylamine using GC-MSD and GC-NPD. J Anal Toxicol, 2003. [DOI | PubMed]
- RJP Custodio, LV Sayson, CJ Botanas, A Abiero, KY You, M Kim, HJ Lee, SY Yoo, KW Lee, YS Lee, JW Seo, IS Ryu, HJ Kim, JH Cheong. 25B-NBOMe, a novel N-2-methoxybenzyl-phenethylamine (NBOMe) derivative, may induce rewarding and reinforcing effects via a dopaminergic mechanism: evidence of abuse potential. Addict Biol, 2019. [DOI | PubMed]
- TA Dal Cason, R Young, RA Glennon. Cathinone: an investigation of several N-alkyl and methylenedioxy-substituted analogs. Pharmacol Biochem Behav, 1997. [DOI | PubMed]
- R Daniulaityte, MP Juhascik, KE Strayer, IE Sizemore, KE Harshbarger, HM Antonides, RR Carlson. Overdose deaths related to fentanyl and its analogs—Ohio, January–February 2017. MMWR Morb Mortal Wkly Rep, 2017. [DOI | PubMed]
- PI Dargan, HC Tang, W Liang, DM Wood, DT Yew. Three months of methoxetamine administration is associated with significant bladder and renal toxicity in mice. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- S Darke, J Duflou, M Farrell, A Peacock, J Lappin. Characteristics and circumstances of synthetic cannabinoid-related death. Clin Toxicol (Phila), 2019. [DOI]
- A Daveluy, N Castaing, H Cherifi, C Richeval, L Humbert, I Faure, M Labadie, D Allorge, F Haramburu, M Molimard, K Titier. Acute methiopropamine intoxication after “synthacaine" consumption. J Anal Toxicol, 2016. [DOI | PubMed]
- C Davis, D Boddington. Teenage cardiac arrest following abuse of synthetic cannabis. Heart Lung Circ, 2015. [DOI | PubMed]
- FT Davis, ME Brewster. A fatality involving U4Euh, a cyclic derivative of phenylpropanolamine. J Forensic Sci, 1988. [DOI | PubMed]
- P Dawson, J Opacka-Juffry, JD Moffatt, Y Daniju, N Dutta, J Ramsey, C Davidson. The effects of benzofury (5-APB) on the dopamine transporter and 5-HT2-dependent vasoconstriction in the rat. Prog Neuropsychopharmacol Biol Psychiatry, 2014. [DOI | PubMed]
- L De Carlis, A De Gasperi, AO Slim, A Giacomoni, A Corti, E Mazza, F Di Benedetto, A Lauterio, K Arcieri, G Maione, GF Rondinara, D Forti. Liver transplantation for ecstasy-induced fulminant hepatic failure. Transplant Proc, 2001. [DOI | PubMed]
- A De Havenon, B Chin, KC Thomas, P Afra. The secret "spice": an undetectable toxic cause of seizure. Neurohospitalist, 2011. [DOI | PubMed]
- LAA De Jong, EJH Olyslager, W Duijst. The risk of emerging new psychoactive substances: the first fatal 3-MeO-PCP intoxication in The Netherlands. J Forensic Leg Med, 2019. [DOI | PubMed]
- BV Dean, SJ Stellpflug, AM Burnett, KM Engebretsen. 2C or not 2C: phenethylamine designer drug review. J Med Toxicol, 2013. [DOI | PubMed]
- H Deng, CD Verrico, TR Kosten, DA Nielsen. Psychosis and synthetic cannabinoids. Psychiatry Res, 2018. [DOI | PubMed]
- JS Denton, ER Donoghue, J McReynolds, MB Kalelkar. An epidemic of illicit fentanyl deaths in Cook County, Illinois: September 2005 through April 2007. J Forensic Sci, 2008. [DOI | PubMed]
- RW Derlet, P Rice, BZ Horowitz, RV Lord. Amphetamine toxicity: experience with 127 cases. J Emerg Med, 1989. [DOI | PubMed]
- SJ DeRoux, WA Dunn. "Bath Salts" the New York City medical examiner experience: a 3-year retrospective review. J Forensic Sci, 2017. [DOI | PubMed]
- A Derungs, AE Schwaninger, G Mansella, R Bingisser, T Kraemer, ME Liechti. Symptoms, toxicities, and analytical results for a patient after smoking herbs containing the novel synthetic cannabinoid MAM-2201. Forensic Toxicol, 2013. [DOI]
- HM Deutsch, Q Shi, E Gruszecka-Kowalik, MM Schweri. Synthesis and pharmacology of potential cocaine antagonists. 2. Structure-activity relationship studies of aromatic ring-substituted methylphenidate analogs. J Med Chem, 1996. [DOI | PubMed]
- JM Devgun, A Rasin, T Kim, MB Mycyk, SM Bryant, MS Wahl, C DesLauriers, L Navon, ED Moritz, TM Thompson, HD Swoboda, J Lu, SE Aks. An outbreak of severe coagulopathy from synthetic cannabinoids tainted with long-acting anticoagulant rodenticides. Clin Toxicol (Phila), 2019. [DOI]
- B Di Cara, R Maggio, G Aloisi, JM Rivet, EG Lundius, T Yoshitake, P Svenningsson, M Brocco, A Gobert, L De Groote, L Cistarelli, S Veiga, C De Montrion, M Rodriguez, JP Galizzi, BP Lockhart, F Coge, JA Boutin, P Vayer, PM Verdouw, L Groenink, MJ Millan. Genetic deletion of trace amine 1 receptors reveals their role in auto-inhibiting the actions of ecstasy (MDMA). J Neurosci, 2011. [DOI | PubMed]
- D Dias da Silva, MJ Silva, P Moreira, MJ Martins, MJ Valente, F Carvalho, ML Bastos, H Carmo. In vitro hepatotoxicity of ‘Legal X’: the combination of 1-benzylpiperazine (BZP) and 1-(m-trifluoromethylphenyl)piperazine (TFMPP) triggers oxidative stress, mitochondrial impairment and apoptosis. Arch Toxicol, 2017. [DOI | PubMed]
- D Dias da Silva, B Ferreira, R Roque Bravo, R Rebelo, T Duarte de Almeida, MJ Valente, JP Silva, F Carvalho, ML Bastos, H Carmo. The new psychoactive substance 3-methylmethcathinone (3-MMC or metaphedrone) induces oxidative stress, apoptosis, and autophagy in primary rat hepatocytes at human-relevant concentrations. Arch Toxicol, 2019. [DOI | PubMed]
- D Dias-da-Silva, MD Arbo, MJ Valente, ML Bastos, H Carmo. Hepatotoxicity of piperazine designer drugs: comparison of different in vitro models. Toxicol In Vitro, 2015. [DOI | PubMed]
- PC Dolder, Y Schmid, F Müller, S Borgwardt, ME Liechti. LSD acutely impairs fear recognition and enhances emotional empathy and sociality. Neuropsychopharmacology, 2016. [DOI | PubMed]
- PC Dolder, P Strajhar, P Vizeli, F Hammann, A Odermatt, ME Liechti. Pharmacokinetics and pharmacodynamics of lisdexamfetamine compared with D-amphetamine in healthy subjects. Front Pharmacol, 2017. [DOI | PubMed]
- K Domanski, KC Kleinschmidt, JM Schulte, S Fleming, C Frazee, A Menendez, K Tavakoli. Two cases of intoxication with new synthetic opioid, U-47700. Clin Toxicol (Phila), 2017. [DOI | PubMed]
- O Domingo, G Roider, A Stover, M Graw, F Musshoff, H Sachs, W Bicker. Mitragynine concentrations in two fatalities. Forensic Sci Int, 2017. [DOI | PubMed]
- EF Domino. History and pharmacology of PCP and PCP-related analogs. J Psychedelic Drugs, 1980. [DOI | PubMed]
- S Droogmans, B Cosyns, H D’Haenen, E Creeten, C Weytjens, PR Franken, B Scott, D Schoors, A Kemdem, L Close, JL Vandenbossche, S Bechet, G Van Camp. Possible association between 3,4-methylenedioxymethamphetamine abuse and valvular heart disease. Am J Cardiol, 2007. [DOI | PubMed]
- LC Dunlop, D Wood, J Archer, S Hudson, P Dargan. Severe toxicity to the new psychoactive substances 3-hydroxyphencyclidine and N-ethylhexedrone: an analytically confirmed case report. J Med Toxicol, 2019. [DOI | PubMed]
- D Durand, LL Delgado, DM De la Parra-Pellot, D Nichols-Vinueza. Psychosis and severe rhabdomyolysis associated with synthetic cannabinoid use: a case report. Clin Schizophr Relat Psychoses, 2015. [DOI | PubMed]
- FE Dussy, S Hangartner, C Hamberg, C Berchtold, U Scherer, G Schlotterbeck, D Wyler, TA Briellmann. An acute ocfentanil fatality: a case report with postmortem concentrations. J Anal Toxicol, 2016. [DOI | PubMed]
- JB Dwyer, J Janssen, TM Luckasevic, KE Williams. Report of increasing overdose deaths that include acetyl fentanyl in multiple counties of the southwestern region of the Commonwealth of Pennsylvania in 2015–2016. J Forensic Sci, 2018. [DOI | PubMed]
- C Eiden, O Mathieu, P Cathala, D Debruyne, E Baccino, P Petit, H Peyriere. Toxicity and death following recreational use of 2-pyrrolidino valerophenone. Clin Toxicol (Phila), 2013. [DOI | PubMed]
- S El Balkhi, C Monchaud, F Herault, H Geniaux, F Saint-Marcoux. Designer benzodiazepines’ pharmacological effects and potencies: how to find the information. J Psychopharmacol, 2020. [DOI]
- T El Zahran, R Gerona, BW Morgan, AC Pomerleau. A novel synthetic cannabinoid (cumyl-4-cyano-BINACA) resulting in hyperthermia, rhabdomyolysis, and renal failure in a 29-year-old patient: it’s not meningitis. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- CS Elangbam. Drug-induced valvulopathy: an update. Toxicol Pathol, 2010. [DOI | PubMed]
- CS Elangbam, LE Job, LM Zadrozny, JC Barton, LW Yoon, LD Gates, N Slocum. 5-Hydroxytryptamine (5-HT)-induced valvulopathy: compositional valvular alterations are associated with 5-HT2B receptor and 5-HT transporter transcript changes in Sprague-Dawley rats. Exp Toxicol Pathol, 2008. [DOI | PubMed]
- KN Ellefsen, EA Taylor, P Simmons, V Willoughby, BJ Hall. Multiple drug-toxicity involving novel psychoactive substances, 3-fluorophenmetrazine and U-47700. J Anal Toxicol, 2017. [DOI | PubMed]
- S Elliott, J Evans. A 3-year review of new psychoactive substances in casework. Forensic Sci Int, 2014. [DOI | PubMed]
- SP Elliott, SD Brandt, J Wallach, H Morris, PV Kavanagh. First reported fatalities associated with the ‘research chemical’ 2-methoxydiphenidine. J Anal Toxicol, 2015. [DOI | PubMed]
- SP Elliott, SD Brandt, C Smith. The first reported fatality associated with the synthetic opioid 3,4-dichloro-N-[2-(dimethylamino)cyclohexyl]-N-methylbenzamide (U-47700) and implications for forensic analysis. Drug Test Anal, 2016. [DOI | PubMed]
- AJ Ellis, JA Wendon, B Portmann, R Williams. Acute liver damage and ecstasy ingestion. Gut, 1996. [DOI | PubMed]
- JS Elmore, AM Decker, A Sulima, KC Rice, JS Partilla, BE Blough, MH Baumann. Comparative neuropharmacology of N-(2-methoxybenzyl)-2,5-dimethoxyphenethylamine (NBOMe) hallucinogens and their 2C counterparts in male rats. Neuropharmacology, 2018. [DOI | PubMed]
- AJ Eshleman, KM Wolfrum, MG Hatfield, RA Johnson, KV Murphy, A Janowsky. Substituted methcathinones differ in transporter and receptor interactions. Biochem Pharmacol, 2013. [DOI | PubMed]
- AJ Eshleman, MJ Forster, KM Wolfrum, RA Johnson, A Janowsky, MB Gatch. Behavioral and neurochemical pharmacology of six psychoactive substituted phenethylamines: mouse locomotion, rat drug discrimination and in vitro receptor and transporter binding and function. Psychopharmacology, 2014. [DOI | PubMed]
- AJ Eshleman, KM Wolfrum, JF Reed, SO Kim, T Swanson, RA Johnson, A Janowsky. Structure-activity relationships of substituted cathinones, with transporter binding, uptake, and release. J Pharmacol Exp Ther, 2017. [DOI | PubMed]
- AJ Eshleman, KM Wolfrum, JF Reed, SO Kim, RA Johnson, A Janowsky. Neurochemical pharmacology of psychoactive substituted N-benzylphenethylamines: high potency agonists at 5-HT2A receptors. Biochem Pharmacol, 2018. [DOI | PubMed]
- European Monitoring Centre for Drugs and Drug Addiction (2015) Report on the risk assessment of 4,4ʹ-DMAR. https://www.emcdda.europa.eu/system/files/publications/1864/TDAK14005ENN.pdf, Accessed 7 Jan 2020
- European Monitoring Centre for Drugs and Drug Addiction (2019) European drug report 2019. https://www.emcdda.europa.eu/system/files/publications/11364/20191724_TDAT19001ENN_PDF.pdf. Accessed 7 Jan 2020
- S Every-Palmer. Warning: legal synthetic cannabinoid-receptor agonists such as JWH-018 may precipitate psychosis in vulnerable individuals. Addiction, 2010. [DOI | PubMed]
- IH Fahal, DF Sallomi, M Yaqoob, GM Bell. Acute renal failure after ecstasy. BMJ, 1992. [DOI | PubMed]
- JK Fallon, D Shah, AT Kicman, AJ Hutt, JA Henry, DA Cowan, M Forsling. Action of MDMA (ecstasy) and its metabolites on arginine vasopressin release. Ann N Y Acad Sci, 2002. [DOI | PubMed]
- WE Fantegrossi, AW Harrington, JR Eckler, S Arshad, RA Rabin, JC Winter, A Coop, KC Rice, JH Woods. Hallucinogen-like actions of 2,5-dimethoxy-4-(n)-propylthiophenethylamine (2C-T-7) in mice and rats. Psychopharmacology, 2005. [DOI | PubMed]
- WE Fantegrossi, CJ Reissig, EB Katz, HL Yarosh, KC Rice, JC Winter. Hallucinogen-like effects of N, N-dipropyltryptamine (DPT): possible mediation by serotonin 5-HT1A and 5-HT2A receptors in rodents. Pharmacol Biochem Behav, 2008. [DOI | PubMed]
- R Farah, R Farah. Ecstasy (3,4-methylenedioxymethamphetamine)-induced inappropriate antidiuretic hormone secretion. Pediatr Emerg Care, 2008. [DOI | PubMed]
- R Faroqui, P Mena, AR Wolfe, J Bibawy, GA Visvikis, MT Mantello. Acute carotid thrombosis and ischemic stroke following overdose of the synthetic cannabinoid K2 in a previously healthy young adult male. Radiol Case Rep, 2018. [DOI | PubMed]
- M Fawzy, WS Wong-Morrow, A Beaumont, CKT Farmer. Acute kidney injury and critical limb ischaemia associated with the use of the so called "legal high" 3-fluorophenmetrazine. CEN Case Rep, 2017. [DOI | PubMed]
- H Fels, J Krueger, H Sachs, F Musshoff, M Graw, G Roider, A Stoever. Two fatalities associated with synthetic opioids: AH-7921 and MT-45. Forensic Sci Int, 2017. [DOI | PubMed]
- H Fels, S Lottner-Nau, T Sax, G Roider, M Graw, V Auwärter, F Musshoff. Postmortem concentrations of the synthetic opioid U-47700 in 26 fatalities associated with the drug. Forensic Sci Int, 2019. [DOI | PubMed]
- DB Finlay, JJ Manning, MS Ibsen, CE Macdonald, M Patel, JA Javitch, SD Banister, M Glass. Do toxic synthetic cannabinoid receptor agonists have signature in vitro activity profiles? A case study of AMB-FUBINACA. ACS Chem Neurosci, 2019. [DOI | PubMed]
- AE Fleckenstein, JW Gibb, GR Hanson. Differential effects of stimulants on monoaminergic transporters: pharmacological consequences and implications for neurotoxicity. Eur J Pharmacol, 2000. [DOI | PubMed]
- AE Fleckenstein, TJ Volz, EL Riddle, JW Gibb, GR Hanson. New insights into the mechanism of action of amphetamines. Annu Rev Pharmacol Toxicol, 2007. [DOI | PubMed]
- MB Forrester. Adolescent synthetic cannabinoid exposures reported to Texas poison centers. Pediatr Emerg Care, 2012. [DOI | PubMed]
- MB Forrester. Synthetic cathinone exposures reported to Texas poison centers. Am J Drug Alcohol Abuse, 2012. [DOI | PubMed]
- MB Forrester. 2C series phenethylamine derivative exposures in Texas. Subst Abus, 2013. [DOI | PubMed]
- MB Forrester. NBOMe designer drug exposures reported to Texas poison centers. J Addict Dis, 2014. [DOI | PubMed]
- MB Forrester, K Kleinschmidt, E Schwarz, A Young. Synthetic cannabinoid exposures reported to Texas poison centers. J Addict Dis, 2011. [DOI | PubMed]
- MB Forrester, K Kleinschmidt, E Schwarz, A Young. Synthetic cannabinoid and marijuana exposures reported to poison centers. Hum Exp Toxicol, 2012. [DOI | PubMed]
- M Forsling, JK Fallon, AT Kicman, AJ Hutt, DA Cowan, JA Henry. Arginine vasopressin release in response to the administration of 3,4-methylenedioxymethamphetamine ("ecstasy"): is metabolism a contributory factor?. J Pharm Pharmacol, 2001. [DOI | PubMed]
- ML Forsling, JK Fallon, D Shah, GS Tilbrook, DA Cowan, AT Kicman, AJ Hutt. The effect of 3,4-methylenedioxymethamphetamine (MDMA, ‘ecstasy’) and its metabolites on neurohypophysial hormone release from the isolated rat hypothalamus. Br J Pharmacol, 2002. [DOI | PubMed]
- C Fort, B Curtis, C Nichols, C Niblo. Acetyl fentanyl toxicity: two case reports. J Anal Toxicol, 2016. [DOI | PubMed]
- F Foti, M Marti, A Ossato, S Bilel, E Sangiorgi, F Botre, B Cerbelli, A Baldi, F De-Giorgio. Phenotypic effects of chronic and acute use of methiopropamine in a mouse model. Int J Legal Med, 2019. [DOI | PubMed]
- L Franzén, M Bäckberg, O Beck, A Helander. Acute intoxications involving α-pyrrolidinobutiophenone (α-PBP): results from the Swedish STRIDA project. J Med Toxicol, 2018. [DOI | PubMed]
- MJ Freeman, DZ Rose, MA Myers, CL Gooch, AC Bozeman, WS Burgin. Ischemic stroke after use of the synthetic marijuana "spice". Neurology, 2013. [DOI | PubMed]
- RW Freudenmann, F Oxler, S Bernschneider-Reif. The origin of MDMA (ecstasy) revisited: the true story reconstructed from the original documents. Addiction, 2006. [DOI | PubMed]
- P Frisoni, E Bacchio, S Bilel, A Talarico, RM Gaudio, M Barbieri, M Neri, M Marti. Novel synthetic opioids: the pathologist’s point of view. Brain Sci, 2018. [DOI]
- S Fröhlich, E Lambe, J O’Dea. Acute liver failure following recreational use of psychotropic "head shop" compounds. Ir J Med Sci, 2011. [DOI | PubMed]
- RW Fuller. Effects of p-chloroamphetamine on brain serotonin neurons. Neurochem Res, 1992. [DOI | PubMed]
- DE Fuller, CS Hornfeldt, JS Kelloway, PJ Stahl, TF Anderson. The Xyrem risk management program. Drug Saf, 2004. [DOI | PubMed]
- Y Fuse-Nagase, T Nishikawa. Prolonged delusional state triggered by repeated ingestion of aromatic liquid in a past 5-methoxy-NN-diisopropyltryptamine abuser. Addict Sci Clin Pract, 2013. [DOI | PubMed]
- SP Gaine, LJ Rubin, JJ Kmetzo, HI Palevsky, TA Traill. Recreational use of aminorex and pulmonary hypertension. Chest, 2000. [DOI | PubMed]
- TF Gamage, CE Farquhar, TW Lefever, JA Marusich, RC Kevin, IS McGregor, JL Wiley, BF Thomas. Molecular and behavioral pharmacological characterization of abused synthetic cannabinoids MMB- and MDMB-FUBINACA, MN-18, NNEI, CUMYL-PICA, and 5-fluoro-CUMYL-PICA. J Pharmacol Exp Ther, 2018. [DOI | PubMed]
- BM Gannon, KI Galindo, MP Mesmin, A Sulima, KC Rice, GT Collins. Relative reinforcing effects of second-generation synthetic cathinones: acquisition of self-administration and fixed ratio dose-response curves in rats. Neuropharmacology, 2018. [DOI | PubMed]
- J Garbino, JA Henry, G Mentha, JA Romand. Ecstasy ingestion and fulminant hepatic failure: liver transplantation to be considered as a last therapeutic option. Vet Hum Toxicol, 2001. [PubMed]
- G Gardos, JO Cole. Evaluation of pyrovalerone in chronically fatigued volunteers. Curr Ther Res Clin Exp, 1971. [PubMed]
- B Garneau, B Desharnais, A Beauchamp-Dore, C Lavallee, P Mireault, A Lajeunesse. Challenges related to three cases of fatal intoxication to multiple novel synthetic opioids. J Anal Toxicol, 2019. [DOI]
- F Gaunitz, S Lehmann, A Thomas, M Thevis, MA Rothschild, K Mercer-Chalmers-Bender. Post-mortem distribution of the synthetic cannabinoid MDMB-CHMICA and its metabolites in a case of combined drug intoxication. Int J Legal Med, 2018. [DOI | PubMed]
- P Gee, S Richardson, W Woltersdorf, G Moore. Toxic effects of BZP-based herbal party pills in humans: a prospective study in Christchurch. New Zealand N Z Med J, 2005. [PubMed]
- P Gee, M Gilbert, S Richardson, G Moore, S Paterson, P Graham. Toxicity from the recreational use of 1-benzylpiperazine. Clin Toxicol (Phila), 2008. [DOI | PubMed]
- P Gee, T Jerram, D Bowie. Multiorgan failure from 1-benzylpiperazine ingestion—legal high or lethal high?. Clin Toxicol (Phila), 2010. [DOI | PubMed]
- E Gerace, E Bovetto, DD Corcia, M Vincenti, A Salomone. A case of nonfatal intoxication associated with the recreational use of diphenidine. J Forensic Sci, 2017. [DOI | PubMed]
- MA Geyer, FX Vollenweider. Serotonin research: contributions to understanding psychoses. Trends Pharmacol Sci, 2008. [DOI | PubMed]
- A Ghatol, A Kazory. Ecstasy-associated acute severe hyponatremia and cerebral edema: a role for osmotic diuresis?. J Emerg Med, 2012. [DOI | PubMed]
- TJ Gillespie, AJ Gandolfi, TP Davis, RA Morano. Identification and quantification of alpha-methylfentanyl in post mortem specimens. J Anal Toxicol, 1982. [DOI | PubMed]
- MD Ginsberg, M Hertzman, WW Schmidt-Nowara. Amphetamine intoxication with coagulopathy, hyperthermia, and reversible renal failure: a syndrome resembling heatstroke. Ann Intern Med, 1970. [DOI | PubMed]
- RM Gladden, J O’Donnell, CL Mattson, P Seth. Changes in opioid-involved overdose deaths by opioid type and presence of benzodiazepines, cocaine, and methamphetamine—25 states, July–December 2017 to January–June 2018. MMWR Morb Mortal Wkly Rep, 2019. [DOI | PubMed]
- J Glanville, PI Dargan, DM Wood. 4-methyl-5-(4-methylphenyl)-4,5-dihydrooxazol-2-amine (4,4ʹ-DMAR, 4,4ʹ-dimethylaminorex): availability, prevalence of use, desired effects and acute toxicity. Hum Psychopharmacol, 2015. [DOI | PubMed]
- P Glue, S Al-Shaqsi, D Hancock, C Gale, B Strong, L Schep. Hospitalisation associated with use of the synthetic cannabinoid K2. N Z Med J, 2013. [PubMed]
- D González, M Torrens, M Farré. Acute effects of the novel psychoactive drug 2C-B on emotions. Biomed Res Int, 2015. [DOI | PubMed]
- MR Graham, P Ryan, JS Baker, B Davies, NE Thomas, SM Cooper, P Evans, S Easmon, CJ Walker, D Cowan, AT Kicman. Counterfeiting in performance- and image-enhancing drugs. Drug Test Anal, 2009. [DOI | PubMed]
- S Grautoff, J Kähler. Lebensgefährliche Intoxikation mit der neuen psychoaktiven Substanz 25C-NBOMe. Medizinische Klinik Intensivmedizin und Notfallmedizin, 2014. [DOI]
- AR Green, AO Mechan, JM Elliott, E Shea, MI Colado. The pharmacology and clinical pharmacology of 3,4-methylenedioxymethamphetamine (MDMA, “ecstasy”). Pharmacol Rev, 2003. [DOI | PubMed]
- SL Greene, PI Dargan, N O’Connor, AL Jones, M Kerins. Multiple toxicity from 3,4-methylenedioxymethamphetamine ("ecstasy"). Am J Emerg Med, 2003. [DOI | PubMed]
- C Grumann, K Henkel, A Stratford, M Hermanns-Clausen, T Passie, SD Brandt, V Auwärter. Validation of an LC–MS/MS method for the quantitative analysis of 1P-LSD and its tentative metabolite LSD in fortified urine and serum samples including stability tests for 1P-LSD under different storage conditions. J Pharm Biomed Anal, 2019. [DOI | PubMed]
- VS Gudsoorkar, JA Perez. A new differential diagnosis: synthetic cannabinoids-associated acute renal failure. Methodist Debakey Cardiovasc J, 2015. [DOI | PubMed]
- D Guerrieri, E Rapp, M Roman, H Druid, R Kronstrand. Postmortem and toxicological findings in a series of furanylfentanyl-related deaths. J Anal Toxicol, 2017. [DOI | PubMed]
- H Gugelmann, R Gerona, C Li, B Tsutaoka, KR Olson, D Lung. ‘Crazy Monkey’ poisons man and dog: human and canine seizures due to PB-22, a novel synthetic cannabinoid. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- V Halachanova, RA Sansone, S McDonald. Delayed rhabdomyolysis after ecstasy use. Mayo Clin Proc, 2001. [DOI | PubMed]
- AL Halberstadt. Behavioral and pharmacokinetic interactions between monoamine oxidase inhibitors and the hallucinogen 5-methoxy-N, N-dimethyltryptamine. Pharmacol Biochem Behav, 2016. [DOI | PubMed]
- AL Halberstadt. Pharmacology and toxicology of N-benzylphenethylamine ("NBOMe") hallucinogens. Curr Top Behav Neurosci, 2017. [DOI | PubMed]
- AL Halberstadt, MA Geyer. Multiple receptors contribute to the behavioral effects of indoleamine hallucinogens. Neuropharmacology, 2011. [DOI | PubMed]
- AL Halberstadt, MA Geyer. Effects of the hallucinogen 2,5-dimethoxy-4-iodophenethylamine (2C-I) and superpotent N-benzyl derivatives on the head twitch response. Neuropharmacology, 2014. [DOI | PubMed]
- AL Halberstadt, DE Nichols, MA Geyer. Behavioral effects of α, α, β, β-tetradeutero-5-MeO-DMT in rats: comparison with 5-MeO-DMT administered in combination with a monoamine oxidase inhibitor. Psychopharmacology, 2012. [DOI | PubMed]
- AL Halberstadt, M Chatha, A Stratford, M Grill, SD Brandt. Comparison of the behavioral responses induced by phenylalkylamine hallucinogens and their tetrahydrobenzodifuran ("FLY") and benzodifuran ("DragonFLY") analogs. Neuropharmacology, 2019. [DOI | PubMed]
- AL Halberstadt, M Chatha, AK Klein, J Wallach, SD Brandt. Correlation between the potency of hallucinogens in the mouse head-twitch response assay and their behavioral and subjective effects in other species. Neuropharmacology, 2020. [DOI]
- RJ Hamilton, V Keyfes, SS Banka. Synthetic cannabinoid abuse resulting in ST-segment elevation myocardial infarction requiring percutaneous coronary intervention. J Emerg Med, 2017. [DOI | PubMed]
- CR Harris, A Brown. Synthetic cannabinoid intoxication: a case series and review. J Emerg Med, 2013. [DOI | PubMed]
- TK Hartung, E Schofield, AI Short, MJ Parr, JA Henry. Hyponatraemic states following 3,4-methylenedioxymethamphetamine (MDMA, ‘ecstasy’) ingestion. QJM, 2002. [DOI | PubMed]
- K Hasegawa, A Wurita, K Minakata, K Gonmori, I Yamagishi, H Nozawa, K Watanabe, O Suzuki. Identification and quantitation of 5-fluoro-ADB, one of the most dangerous synthetic cannabinoids, in the stomach contents and solid tissues of a human cadaver and in some herbal products. Forensic Toxicol, 2015. [DOI]
- DJ Heal, SL Smith, J Gosden, DJ Nutt. Amphetamine, past and present—a pharmacological and clinical perspective. J Psychopharmacol, 2013. [DOI | PubMed]
- Heim R (2004) Synthese und Pharmakologie potenter 5-HT2A-Rezeptoragonisten mit N-2-Methoxybenzyl-Partialstruktur: Entwicklung eines neuen Struktur-Wirkungskonzepts. Dissertation, Freie Universität Berlin. https://refubium.fu-berlin.de/bitstream/handle/fub188/11995/0_RalfHeimTitelblatt.pdf?sequence=1&isAllowed=y. Accessed 7 Jan 2020
- A Helander, M Bäckberg, O Beck. MT-45, a new psychoactive substance associated with hearing loss and unconsciousness. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- A Helander, O Beck, M Bäckberg. Intoxications by the dissociative new psychoactive substances diphenidine and methoxphenidine. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- A Helander, M Bäckberg, O Beck. Intoxications involving the fentanyl analogs acetylfentanyl, 4-methoxybutyrfentanyl and furanylfentanyl: results from the Swedish STRIDA project. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- A Helander, M Bäckberg, P Signell, O Beck. Intoxications involving acrylfentanyl and other novel designer fentanyls – results from the Swedish STRIDA project. Clin Toxicol (Phila), 2017. [DOI | PubMed]
- A Helander, M Bradley, A Hasselblad, L Norlen, I Vassilaki, M Bäckberg, J Lapins. Acute skin and hair symptoms followed by severe, delayed eye complications in subjects using the synthetic opioid MT-45. Br J Dermatol, 2017. [DOI | PubMed]
- JA Henry, KJ Jeffreys, S Dawling. Toxicity and deaths from 3,4-methylenedioxymethamphetamine ("ecstasy"). Lancet, 1992. [DOI | PubMed]
- M Herian, A Wojtas, K Kaminska, P Swit, A Wach, K Golembiowska. Hallucinogen-like action of the novel designer drug 25I-NBOMe and its effect on cortical neurotransmitters in rats. Neurotox Res, 2019. [DOI | PubMed]
- M Hermanns-Clausen, S Kneisel, M Hutter, B Szabo, V Auwärter. Acute intoxication by synthetic cannabinoids—four case reports. Drug Test Anal, 2013. [DOI | PubMed]
- M Hermanns-Clausen, S Kneisel, B Szabo, V Auwärter. Acute toxicity due to the confirmed consumption of synthetic cannabinoids: clinical and laboratory findings. Addiction, 2013. [DOI | PubMed]
- M Hermanns-Clausen, V Angerer, J Kithinji, C Grumann, V Auwärter. Bad trip due to 25I-NBOMe: a case report from the EU project SPICE II plus. Clin Toxicol (Phila), 2017. [DOI | PubMed]
- T Herraiz, SD Brandt. 5-(2-Aminopropyl)indole (5-IT): a psychoactive substance used for recreational purposes is an inhibitor of human monoamine oxidase (MAO). Drug Test Anal, 2014. [DOI | PubMed]
- SL Hill, SH Thomas. Clinical toxicology of newer recreational drugs. Clin Toxicol (Phila), 2011. [DOI | PubMed]
- SL Hill, T Doris, S Gurung, S Katebe, A Lomas, M Dunn, P Blain, SH Thomas. Severe clinical toxicity associated with analytically confirmed recreational use of 25I-NBOMe: case series. Clin Toxicol (Phila), 2013. [DOI | PubMed]
- K Hirapara, R Aggarwal. Synthetic cannabis and myocardial infarction: a complication less known!. Psychosomatics, 2015. [DOI | PubMed]
- JH Ho, GP Bailey, JR Archer, PI Dargan, DM Wood. Ethylphenidate: availability, patterns of use, and acute effects of this novel psychoactive substance. Eur J Clin Pharmacol, 2015. [DOI | PubMed]
- M Hobbs, NJ Kalk, PD Morrison, JM Stone. Spicing it up—synthetic cannabinoid receptor agonists and psychosis—a systematic review. Eur Neuropsychopharmacol, 2018. [DOI | PubMed]
- KE Hofer, B Grager, DM Müller, C Rauber-Lüthy, H Kupferschmidt, KM Rentsch, A Ceschi. Ketamine-like effects after recreational use of methoxetamine. Ann Emerg Med, 2012. [DOI | PubMed]
- KE Hofer, C Degrandi, DM Müller, U Zürrer-Härdi, S Wahl, C Rauber-Lüthy, A Ceschi. Acute toxicity associated with the recreational use of the novel dissociative psychoactive substance methoxphenidine. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- Hofmann A, Troxler F (1962) Nouveaux dérivés de l’indole, procédé de préparation et médicaments les contenant. FR1344579
- L Hondebrink, JJ Nugteren-van Lonkhuyzen, SJ Rietjens, TM Brunt, B Venhuis, V Soerdjbalie-Maikoe, BE Smink, A Van Riel, I De Vries. Fatalities, cerebral hemorrhage, and severe cardiovascular toxicity after exposure to the new psychoactive substance 4-fluoroamphetamine: a prospective cohort study. Ann Emerg Med, 2018. [DOI | PubMed]
- CY Hopkins, BL Gilchrist. A case of cannabinoid hyperemesis syndrome caused by synthetic cannabinoids. J Emerg Med, 2013. [DOI | PubMed]
- CO Hoyte, J Jacob, AA Monte, M Al-Jumaan, AC Bronstein, KJ Heard. A characterization of synthetic cannabinoid exposures reported to the National Poison Data System in 2010. Ann Emerg Med, 2012. [DOI | PubMed]
- HH Huang, YM Bai. Persistent psychosis after ingestion of a single tablet of ‘2C-B’. Prog Neuropsychopharmacol Biol Psychiatry, 2011. [DOI | PubMed]
- XP Huang, V Setola, PN Yadav, JA Allen, SC Rogan, BJ Hanson, C Revankar, M Robers, C Doucette, BL Roth. Parallel functional activity profiling reveals valvulopathogens are potent 5-hydroxytryptamine2B receptor agonists: implications for drug safety assessment. Mol Pharmacol, 2009. [DOI | PubMed]
- D Hurst, G Loeffler, R McLay. Psychosis associated with synthetic cannabinoid agonists: a case series. Am J Psychiatry, 2011. [DOI | PubMed]
- S Ibrahim, F Al-Saffar, T Wannenburg. A unique case of cardiac arrest following K2 abuse. Case Rep Cardiol, 2014. [DOI | PubMed]
- A Ikeda, K Sekiguchi, K Fujita, H Yamadera, Y Koga. 5-methoxy-N, N-diisopropyltryptamine-induced flashbacks. Am J Psychiatry, 2005. [DOI | PubMed]
- L Imbert, A Boucher, G Delhome, T Cueto, M Boudinaud, J Maublanc, S Dulaurent, J Descotes, G Lachatre, JM Gaulier. Analytical findings of an acute intoxication after inhalation of methoxetamine. J Anal Toxicol, 2014. [DOI | PubMed]
- F Inan, TM Brunt, RR Contrucci, L Hondebrink, EJF Franssen. Novel phenethylamines and their potential interactions with prescription drugs: a systematic critical review. Ther Drug Monit, 2020. [DOI | PubMed]
- KZ Isoardi, S Kulawickrama, GK Isbister. Severe phenibut poisoning: an adolescent case cluster. J Paediatr Child Health, 2020. [DOI | PubMed]
- M Itokawa, K Iwata, M Takahashi, G Sugihara, T Sasaki, Y Abe, M Uno, M Hobo, D Jitoku, K Inoue, M Arai, I Yasuda, M Shintani. Acute confusional state after designer tryptamine abuse. Psychiatry Clin Neurosci, 2007. [DOI | PubMed]
- ID Ivanov, S Stoykova, E Ivanova, A Vlahova, N Burdzhiev, I Pantcheva, VN Atanasov. A case of 5F-ADB/FUB-AMB abuse: drug-induced or drug-related death?. Forensic Sci Int, 2019. [DOI | PubMed]
- L Iversen, S Gibbons, R Treble, V Setola, XP Huang, BL Roth. Neurochemical profiles of some novel psychoactive substances. Eur J Pharmacol, 2013. [DOI | PubMed]
- S Iwersen-Bergmann, S Lehmann, A Heinemann, C Schröder, A Müller, H Jungen, H Andresen-Streichert, K Pueschel, C Vidal, K Mercer-Chalmers-Bender. Mass poisoning with NPS: 2C-E and Bromo-DragonFly. Int J Legal Med, 2019. [DOI | PubMed]
- D James, RD Adams, R Spears, G Cooper, DJ Lupton, JP Thompson, SH Thomas. Clinical characteristics of mephedrone toxicity reported to the UK National Poisons Information Service. Emerg Med J, 2011. [DOI | PubMed]
- M Javadi-Paydar, JD Nguyen, SA Vandewater, TJ Dickerson, MA Taffe. Locomotor and reinforcing effects of pentedrone, pentylone and methylone in rats. Neuropharmacology, 2018. [DOI | PubMed]
- J Jebadurai, F Schifano, P Deluca. Recreational use of 1-(2-naphthyl)-2-(1-pyrrolidinyl)-1-pentanone hydrochloride (NRG-1), 6-(2-aminopropyl)benzofuran (benzofury/6-APB) and NRG-2 with review of available evidence-based literature. Hum Psychopharmacol, 2013. [DOI | PubMed]
- AA Jensen, JD McCorvy, S Leth-Petersen, C Bundgaard, G Liebscher, TP Kenakin, H Brauner-Osborne, J Kehler, JL Kristensen. Detailed characterization of the in vitro pharmacological and pharmacokinetic properties of N-(2-hydroxybenzyl)-2,5-dimethoxy-4-cyanophenylethylamine (25CN-NBOH), a highly selective and brain-penetrant 5-HT2A receptor agonist. J Pharmacol Exp Ther, 2017. [DOI | PubMed]
- DA Jerrard. "Designer drugs”—a current perspective. J Emerg Med, 1990. [DOI | PubMed]
- FN Jinwala, M Gupta. Synthetic cannabis and respiratory depression. J Child Adolesc Psychopharmacol, 2012. [DOI | PubMed]
- A Johansson, D Lindstedt, M Roman, G Thelander, EI Nielsen, U Lennborn, H Sandler, S Rubertsson, J Ahlner, R Kronstrand, FC Kugelberg. A non-fatal intoxication and seven deaths involving the dissociative drug 3-MeO-PCP. Forensic Sci Int, 2017. [DOI | PubMed]
- MP Johnson, XM Huang, R Oberlender, JF Nash, DE Nichols. Behavioral, biochemical and neurotoxicological actions of the α-ethyl homologue of p-chloroamphetamine. Eur J Pharmacol, 1990. [DOI | PubMed]
- LA Johnson, RL Johnson, C Alfonzo. Spice: a legal marijuana equivalent. Mil Med, 2011. [DOI | PubMed]
- AL Jones, DR Jarvie, G McDermid, AT Proudfoot. Hepatocellular damage following amphetamine intoxication. J Toxicol Clin Toxicol, 1994. [DOI | PubMed]
- JD Jones, S Mogali, SD Comer. Polydrug abuse: a review of opioid and benzodiazepine combination use. Drug Alcohol Depend, 2012. [DOI | PubMed]
- MJ Jones, BS Hernandez, GC Janis, SJ Stellpflug. A case of U-47700 overdose with laboratory confirmation and metabolite identification. Clin Toxicol (Phila), 2017. [DOI | PubMed]
- JF Joseph, MK Parr. Synthetic androgens as designer supplements. Curr Neuropharmacol, 2015. [DOI | PubMed]
- A Jovel, A Felthous, A Bhattacharyya. Delirium due to intoxication from the novel synthetic tryptamine 5-MeO-DALT. J Forensic Sci, 2014. [DOI | PubMed]
- M Kamel, B Thajudeen. A case of acute kidney injury and calcium oxalate deposition associated with synthetic cannabinoids. Saudi J Kidney Dis Transpl, 2015. [DOI | PubMed]
- Y Kamijo, K Soma, M Nishida, A Namera, T Ohwada. Acute liver failure following intravenous methamphetamine. Vet Hum Toxicol, 2002. [PubMed]
- M Kano, T Ohno-Shosaku, Y Hashimotodani, M Uchigashima, M Watanabe. Endocannabinoid-mediated control of synaptic transmission. Physiol Rev, 2009. [DOI | PubMed]
- V Kapil, JL Green, C Le Lait, DM Wood, PI Dargan. Misuse of benzodiazepines and Z-drugs in the UK. Br J Psychiatry, 2014. [DOI | PubMed]
- R Karinen, SS Tuv, S Rogde, MD Peres, U Johansen, J Frost, V Vindenes, AM Oiestad. Lethal poisonings with AH-7921 in combination with other substances. Forensic Sci Int, 2014. [DOI | PubMed]
- M Katselou, I Papoutsis, P Nikolaou, C Spiliopoulou, S Athanaselis. 5-(2-aminopropyl)indole: a new player in the drama of ‘legal highs’ alerts the community. Drug Alcohol Rev, 2015. [DOI | PubMed]
- DP Katz, J Deruiter, D Bhattacharya, M Ahuja, S Bhattacharya, CR Clark, V Suppiramaniam, M Dhanasekaran. Benzylpiperazine: “a messy drug". Drug Alcohol Depend, 2016. [DOI | PubMed]
- KD Katz, AL Leonetti, BC Bailey, RM Surmaitis, ER Eustice, S Kacinko, SM Wheatley. Case series of synthetic cannabinoid intoxication from one toxicology center. West J Emerg Med, 2016. [DOI | PubMed]
- A Kazory, R Aiyer. Synthetic marijuana and acute kidney injury: an unforeseen association. Clin Kidney J, 2013. [DOI | PubMed]
- AH Kelkar, NA Smith, A Martial, H Moole, MD Tarantino, JC Roberts. An outbreak of synthetic cannabinoid-associated coagulopathy in Illinois. N Engl J Med, 2018. [DOI | PubMed]
- WC Kendrick, AR Hull, JP Knochel. Rhabdomyolysis and shock after intravenous amphetamine administration. Ann Intern Med, 1977. [DOI | PubMed]
- K Kesha, CL Boggs, MG Ripple, CH Allan, B Levine, R Jufer-Phipps, S Doyon, P Chi, DR Fowler. Methylenedioxypyrovalerone ("bath salts"), related death: case report and review of the literature. J Forensic Sci, 2013. [DOI | PubMed]
- M Khan, L Pace, A Truong, M Gordon, N Moukaddam. Catatonia secondary to synthetic cannabinoid use in two patients with no previous psychosis. Am J Addict, 2016. [DOI | PubMed]
- AT Kicman. Pharmacology of anabolic steroids. Br J Pharmacol, 2008. [DOI | PubMed]
- BL Kieffer. Opioids: first lessons from knockout mice. Trends Pharmacol Sci, 1999. [DOI | PubMed]
- HK Kim, LS Nelson. Reducing the harm of opioid overdose with the safe use of naloxone: a pharmacologic review. Expert Opin Drug Saf, 2015. [DOI | PubMed]
- LM Klein, NV Cozzi, PF Daley, SD Brandt, AL Halberstadt. Receptor binding profiles and behavioral pharmacology of ring-substituted N, N-diallyltryptamine analogs. Neuropharmacology, 2018. [DOI | PubMed]
- K Knudsen, U Jonsson, J Abrahamsson. Twenty-three deaths with γ-hydroxybutyrate overdose in western Sweden between 2000 and 2007. Acta Anaesthesiol Scand, 2010. [DOI | PubMed]
- K Koch, V Auwärter, M Hermanns-Clausen, M Wilde, MA Neukamm. Mixed intoxication by the synthetic opioid U-47700 and the benzodiazepine flubromazepam with lethal outcome: pharmacokinetic data. Drug Test Anal, 2018. [DOI | PubMed]
- KE Kolaczynska, D Luethi, D Trachsel, MC Hoener, ME Liechti. Receptor interaction profiles of 4-alkoxy-substituted 2,5-dimethoxyphenethylamines and related amphetamines. Front Pharmacol, 2019. [DOI | PubMed]
- K Kovacs, E Kereszty, R Berkecz, L Tiszlavicz, E Sija, T Kormoczi, N Jenei, H Revesz-Schmehl, L Institoris. Fatal intoxication of a regular drug user following N-ethyl-hexedrone and ADB-FUBINACA consumption. J Forensic Leg Med, 2019. [DOI | PubMed]
- J Kovaleva, E Devuyst, P De Paepe, A Verstraete. Acute chlorophenylpiperazine overdose: a case report and review of the literature. Ther Drug Monit, 2008. [DOI | PubMed]
- R Kraehenmann, D Pokorny, L Vollenweider, KH Preller, T Pokorny, E Seifritz, FX Vollenweider. Dreamlike effects of LSD on waking imagery in humans depend on serotonin 2A receptor activation. Psychopharmacology, 2017. [DOI | PubMed]
- M Kraemer, H Fels, T Dame, F Musshoff, S Halter, L Mogler, C Hess, B Madea, A Maas. Mono-/polyintoxication with 5F-ADB: a case series. Forensic Sci Int, 2019. [DOI | PubMed]
- P Kriikku, A Pelander, I Rasanen, I Ojanpera. Toxic lifespan of the synthetic opioid U-47,700 in Finland verified by re-analysis of UPLC–TOF–MS data. Forensic Sci Int, 2019. [DOI | PubMed]
- R Kronstrand, M Roman, M Dahlgren, G Thelander, M Wikström, H Druid. A cluster of deaths involving 5-(2-aminopropyl)indole (5-IT). J Anal Toxicol, 2013. [DOI | PubMed]
- R Kronstrand, G Thelander, D Lindstedt, M Roman, FC Kugelberg. Fatal intoxications associated with the designer opioid AH-7921. J Anal Toxicol, 2014. [DOI | PubMed]
- AJ Krotulski, DM Papsun, M Friscia, JL Swartz, BD Holsey, BK Logan. Fatality following ingestion of tetrahydrofuranylfentanyl, U-49900 and methoxy-phencyclidine. J Anal Toxicol, 2018. [DOI | PubMed]
- J Krueger, H Sachs, F Musshoff, T Dame, J Schaeper, M Schwerer, M Graw, G Roider. First detection of ethylphenidate in human fatalities after ethylphenidate intake. Forensic Sci Int, 2014. [DOI | PubMed]
- K Kudo, Y Usumoto, R Kikura-Hanajiri, N Sameshima, A Tsuji, N Ikeda. A fatal case of poisoning related to new cathinone designer drugs, 4-methoxy PV8, PV9, and 4-methoxy PV9, and a dissociative agent, diphenidine. Leg Med (Tokyo), 2015. [DOI | PubMed]
- VB Kueppers, CT Cooke. 25I-NBOMe related death in Australia: a case report. Forensic Sci Int, 2015. [DOI | PubMed]
- MJ Kuhar, MC Ritz, JW Boja. The dopamine hypothesis of the reinforcing properties of cocaine. Trends Neurosci, 1991. [DOI | PubMed]
- M Kusano, K Zaitsu, K Taki, K Hisatsune, J Nakajima, T Moriyasu, T Asano, Y Hayashi, H Tsuchihashi, A Ishii. Fatal intoxication by 5F-ADB and diphenidine: detection, quantification, and investigation of their main metabolic pathways in humans by LC/MS/MS and LC/Q–TOFMS. Drug Test Anal, 2018. [DOI | PubMed]
- LM Labay, JL Caruso, TP Gilson, RJ Phipps, LD Knight, NP Lemos, IM McIntyre, R Stoppacher, LM Tormos, AL Wiens, E Williams, BK Logan. Synthetic cannabinoid drug use as a cause or contributory cause of death. Forensic Sci Int, 2016. [DOI | PubMed]
- C Lafferty, L Smith, A Coull, J Shanley. The experience of an increase in the injection of ethylphenidate in Lothian April 2014–March 2015. Scott Med J, 2016. [DOI | PubMed]
- RP Lam, WL Yip, MS Tsui, SW Ng, CK Ching, TW Mak. Severe rhabdomyolysis and acute kidney injury associated with methoxphenidine. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- I Lapin. Phenibut (β-phenyl-GABA): a tranquilizer and nootropic drug. CNS Drug Rev, 2001. [DOI | PubMed]
- J Lapoint, LP James, CL Moran, LS Nelson, RS Hoffman, JH Moran. Severe toxicity following synthetic cannabinoid ingestion. Clin Toxicol (Phila), 2011. [DOI | PubMed]
- R Law, J Schier, C Martin, A Chang, A Wolkin. Notes from the field: increase in reported adverse health effects related to synthetic cannabinoid use—United States, January–May 2015. MMWR Morb Mortal Wkly Rep, 2015. [PubMed]
- R Le Boisselier, J Alexandre, V Lelong-Boulouard, D Debruyne. Focus on cannabinoids and synthetic cannabinoids. Clin Pharmacol Ther, 2017. [DOI | PubMed]
- W Lawn, R Borschmann, A Cottrell, A Winstock. Methoxetamine: prevalence of use in the USA and UK and associated urinary problems. J Subst Use, 2016. [DOI]
- HM Lee, DM Wood, S Hudson, JR Archer, PI Dargan. Acute toxicity associated with analytically confirmed recreational use of methiopropamine (1-(thiophen-2-yl)-2-methylaminopropane). J Med Toxicol, 2014. [DOI | PubMed]
- D Lee, CW Chronister, J Hoyer, BA Goldberger. Ethylone-related deaths: toxicological findings. J Anal Toxicol, 2015. [DOI | PubMed]
- E Leibu, A Garakani, DP McGonigle, LS Liebman, D Loh, EO Bryson, CH Kellner. Electroconvulsive therapy (ECT) for catatonia in a patient with schizophrenia and synthetic cannabinoid abuse: a case report. J ECT, 2013. [DOI | PubMed]
- L Li, PE Vlisides. Ketamine: 50 years of modulating the mind. Front Hum Neurosci, 2016. [DOI | PubMed]
- E Liakoni, F Walther, CH Nickel, ME Liechti. Presentations to an urban emergency department in Switzerland due to acute γ-hydroxybutyrate toxicity. Scand J Trauma Resusc Emerg Med, 2016. [DOI | PubMed]
- ME Liechti. Modern clinical research on LSD. Neuropsychopharmacology, 2017. [DOI | PubMed]
- JC Lin, RK Jan, H Lee, MA Jensen, RR Kydd, BR Russell. Determining the subjective and physiological effects of BZP combined with TFMPP in human males. Psychopharmacology, 2011. [DOI | PubMed]
- K Liveri, MA Constantinou, M Afxentiou, P Kanari. A fatal intoxication related to MDPV and pentedrone combined with antipsychotic and antidepressant substances in Cyprus. Forensic Sci Int, 2016. [DOI | PubMed]
- B Loi, M Zloh, MA De Luca, N Pintori, J Corkery, F Schifano. 4,4ʹ-Dimethylaminorex (“4,4ʹ-DMAR”; “Serotoni”) misuse: a Web-based study. Hum Psychopharmacol, 2017. [DOI]
- LP Longo, B Johnson. Addiction. Part I Benzodiazepines–side effects, abuse risk and alternatives. Am Fam Physician, 2000. [PubMed]
- M Longworth, M Connor, SD Banister, M Kassiou. Synthesis and pharmacological profiling of the metabolites of synthetic cannabinoid drugs APICA, STS-135, ADB-PINACA, and 5F-ADB-PINACA. ACS Chem Neurosci, 2017. [DOI | PubMed]
- SN Lucyk, LS Nelson. Novel synthetic opioids: an opioid epidemic within an opioid epidemic. Ann Emerg Med, 2017. [DOI | PubMed]
- D Luethi, ME Liechti. Monoamine transporter and receptor interaction profiles in vitro predict reported human doses of novel psychoactive stimulants and psychedelics. Int J Neuropsychopharmacol, 2018. [DOI | PubMed]
- D Luethi, ME Liechti, S Krähenbühl. Mechanisms of hepatocellular toxicity associated with new psychoactive synthetic cathinones. Toxicology, 2017. [DOI | PubMed]
- D Luethi, MC Hoener, ME Liechti. Effects of the new psychoactive substances diclofensine, diphenidine, and methoxphenidine on monoaminergic systems. Eur J Pharmacol, 2018. [DOI | PubMed]
- D Luethi, PJ Kaeser, SD Brandt, S Krähenbühl, MC Hoener, ME Liechti. Pharmacological profile of methylphenidate-based designer drugs. Neuropharmacology, 2018. [DOI | PubMed]
- D Luethi, KE Kolaczynska, L Docci, S Krähenbühl, MC Hoener, ME Liechti. Pharmacological profile of mephedrone analogs and related new psychoactive substances. Neuropharmacology, 2018. [DOI | PubMed]
- D Luethi, D Trachsel, MC Hoener, ME Liechti. Monoamine receptor interaction profiles of 4-thio-substituted phenethylamines (2C-T drugs). Neuropharmacology, 2018. [DOI | PubMed]
- D Luethi, KE Kolaczynska, M Walter, M Suzuki, KC Rice, BE Blough, MC Hoener, MH Baumann, ME Liechti. Metabolites of the ring-substituted stimulants MDMA, methylone and MDPV differentially affect human monoaminergic systems. J Psychopharmacol, 2019. [DOI | PubMed]
- D Luethi, M Walter, X Zhou, D Rudin, S Krähenbühl, ME Liechti. Para-halogenation affects monoamine transporter inhibition properties and hepatocellular toxicity of amphetamines and methcathinones. Front Pharmacol, 2019. [DOI | PubMed]
- D Luethi, R Widmer, D Trachsel, MC Hoener, ME Liechti. Monoamine receptor interaction profiles of 4-aryl-substituted 2,5-dimethoxyphenethylamines (2C-BI derivatives). Eur J Pharmacol, 2019. [DOI | PubMed]
- D Lüthi, ME Liechti. Clinical aspects related to methylphenidate-based NPS. Handbook of novel psychoactive substances: what clinicians should know about NPS, 2019
- A Maas, C Wippich, B Madea, C Hess. Driving under the influence of synthetic phenethylamines: a case series. Int J Legal Med, 2015. [DOI | PubMed]
- MK Madsen, PM Fisher, D Burmester, A Dyssegaard, DS Stenbaek, S Kristiansen, SS Johansen, S Lehel, K Linnet, C Svarer, D Erritzoe, B Ozenne, GM Knudsen. Psychedelic effects of psilocybin correlate with serotonin 2A receptor occupancy and plasma psilocin levels. Neuropsychopharmacology, 2019. [DOI | PubMed]
- H Maeda, R Kikura-Hanajiri, M Kawamura, E Nagashima, KI Yoshida. AB-CHMINACA-induced sudden death from non-cardiogenic pulmonary edema. Clin Toxicol (Phila), 2018. [DOI | PubMed]
- P Maguire, N Tsai, J Kamal, C Cometta-Morini, C Upton, G Loew. Pharmacological profiles of fentanyl analogs at μ, δ and κ opiate receptors. Eur J Pharmacol, 1992. [DOI | PubMed]
- J Maier, FP Mayer, SD Brandt, HH Sitte. DARK classics in chemical neuroscience: aminorex analogues. ACS Chem Neurosci, 2018. [DOI | PubMed]
- J Maier, FP Mayer, D Luethi, M Holy, K Jäntsch, H Reither, L Hirtler, MC Hoener, ME Liechti, C Pifl, SD Brandt, HH Sitte. The psychostimulant (±)-cis-4,4ʹ-dimethylaminorex (4,4ʹ-DMAR) interacts with human plasmalemmal and vesicular monoamine transporters. Neuropharmacology, 2018. [DOI | PubMed]
- M Majchrzak, R Celinski, T Kowalska, M Sajewicz. Fatal case of poisoning with a new cathinone derivative: α-propylaminopentiophenone (N-PP). Forensic Toxicol, 2018. [DOI | PubMed]
- M Majrashi, M Almaghrabi, M Fadan, A Fujihashi, W Lee, J Deruiter, C Randall Clark, M Dhanasekaran. Dopaminergic neurotoxic effects of 3-TFMPP derivatives. Life Sci, 2018. [DOI | PubMed]
- KR Manchester, EC Lomas, L Waters, FC Dempsey, PD Maskell. The emergence of new psychoactive substance (NPS) benzodiazepines: a review. Drug Test Anal, 2018. [DOI | PubMed]
- LJ Marinetti, HM Antonides. Analysis of synthetic cathinones commonly found in bath salts in human performance and postmortem toxicology: method development, drug distribution and interpretation of results. J Anal Toxicol, 2013. [DOI | PubMed]
- JS Markowitz, HJ Zhu, KS Patrick. Isopropylphenidate: an ester homolog of methylphenidate with sustained and selective dopaminergic activity and reduced drug interaction liability. J Child Adolesc Psychopharmacol, 2013. [DOI | PubMed]
- G Martinotti, R Santacroce, D Papanti, Y Elgharably, M Prilutskaya, O Corazza. Synthetic cannabinoids: psychopharmacology, clinical aspects, psychotic onset. CNS Neurol Disord Drug Targets, 2017. [DOI | PubMed]
- HFH Martucci, EA Ingle, MD Hunter, LN Rodda. Distribution of furanyl fentanyl and 4-ANPP in an accidental acute death: a case report. Forensic Sci Int, 2018. [DOI | PubMed]
- JA Marusich, KR Antonazzo, BE Blough, SD Brandt, PV Kavanagh, JS Partilla, MH Baumann. The new psychoactive substances 5-(2-aminopropyl)indole (5-IT) and 6-(2-aminopropyl)indole (6-IT) interact with monoamine transporters in brain tissue. Neuropharmacology, 2016. [DOI | PubMed]
- PD Maskell, G De Paoli, C Seneviratne, DJ Pounder. Mephedrone (4-methylmethcathinone)-related deaths. J Anal Toxicol, 2011. [DOI | PubMed]
- PD Maskell, GD Paoli, LN Seetohul, DJ Pounder. Phenazepam is currently being misused in the UK. BMJ, 2011. [DOI | PubMed]
- PD Maskell, PR Smith, R Cole, L Hikin, SR Morley. Seven fatalities associated with ethylphenidate. Forensic Sci Int, 2016. [DOI | PubMed]
- FP Mayer, L Wimmer, O Dillon-Carter, JS Partilla, NV Burchardt, MD Mihovilovic, MH Baumann, HH Sitte. Phase I metabolites of mephedrone display biological activity as substrates at monoamine transporters. Br J Pharmacol, 2016. [DOI | PubMed]
- FP Mayer, NV Burchardt, AM Decker, JS Partilla, Y Li, G McLaughlin, PV Kavanagh, W Sandtner, BE Blough, SD Brandt, MH Baumann, HH Sitte. Fluorinated phenmetrazine "legal highs" act as substrates for high-affinity monoamine transporters of the SLC6 family. Neuropharmacology, 2018. [DOI | PubMed]
- FP Mayer, D Cintulova, DA Pittrich, L Wimmer, D Luethi, M Holy, K Jaentsch, S Tischberger, G Gmeiner, MC Hoener, ME Liechti, MD Mihovilovic, HH Sitte. Stereochemistry of phase-1 metabolites of mephedrone determines their effectiveness as releasers at the serotonin transporter. Neuropharmacology, 2019. [DOI | PubMed]
- FP Mayer, D Schmid, M Holy, LC Daws, HH Sitte. "Polytox" synthetic cathinone abuse: a potential role for organic cation transporter 3 in combined cathinone-induced efflux. Neurochem Int, 2019. [DOI | PubMed]
- DJ McCabe, SA Bangh, AM Arens, JB Cole. Phenibut exposures and clinical effects reported to a regional poison center. Am J Emerg Med, 2019. [DOI | PubMed]
- G McIlroy, L Ford, JM Khan. Acute myocardial infarction, associated with the use of a synthetic adamantyl-cannabinoid: a case report. BMC Pharmacol Toxicol, 2016. [DOI | PubMed]
- IM McIntyre, RD Gary, A Trochta, S Stolberg, R Stabley. Acute 5-(2-aminopropyl)benzofuran (5-APB) intoxication and fatality: a case report with postmortem concentrations. J Anal Toxicol, 2015. [DOI | PubMed]
- IM McIntyre, A Trochta, RD Gary, M Malamatos, JR Lucas. An acute acetyl fentanyl fatality: a case report with postmortem concentrations. J Anal Toxicol, 2015. [DOI | PubMed]
- IM McIntyre, A Trochta, RD Gary, A Storey, J Corneal, B Schaber. A fatality related to two novel hallucinogenic compounds: 4-methoxyphencyclidine and 4-hydroxy-N-methyl-N-ethyltryptamine. J Anal Toxicol, 2015. [DOI | PubMed]
- IM McIntyre, A Trochta, RD Gary, J Wright, O Mena. An acute butyr-fentanyl fatality: a case report with postmortem concentrations. J Anal Toxicol, 2016. [DOI | PubMed]
- IM McIntyre, RD Gary, S Joseph, R Stabley. A fatality related to the synthetic opioid U-47700: postmortem concentration distribution. J Anal Toxicol, 2017. [DOI | PubMed]
- RG McKeever, D Vearrier, D Jacobs, G LaSala, J Okaneku, MI Greenberg. K2–not the spice of life; synthetic cannabinoids and ST elevation myocardial infarction: a case report. J Med Toxicol, 2015. [DOI | PubMed]
- G McLaughlin, N Morris, PV Kavanagh, JD Power, B Twamley, J O’Brien, B Talbot, G Dowling, O Mahony, SD Brandt, J Patrick, RP Archer, JS Partilla, MH Baumann. Synthesis, characterization, and monoamine transporter activity of the new psychoactive substance 3ʹ,4ʹ-methylenedioxy-4-methylaminorex (MDMAR). Drug Test Anal, 2015. [DOI | PubMed]
- G McLaughlin, MH Baumann, PV Kavanagh, N Morris, JD Power, G Dowling, B Twamley, J O’Brien, G Hessman, F Westphal, D Walther, SD Brandt. Synthesis, analytical characterization, and monoamine transporter activity of the new psychoactive substance 4-methylphenmetrazine (4-MPM), with differentiation from its ortho- and meta- positional isomers. Drug Test Anal, 2018. [DOI | PubMed]
- D McQuade, S Hudson, PI Dargan, DM Wood. First European case of convulsions related to analytically confirmed use of the synthetic cannabinoid receptor agonist AM-2201. Eur J Clin Pharmacol, 2013. [DOI | PubMed]
- R Meatherall, P Sharma. Foxy, a designer tryptamine hallucinogen. J Anal Toxicol, 2003. [DOI | PubMed]
- JJ Mehta, AK Mahendran, RK Bajaj, AR Doshi. Myocardial ischemia with cannabinoid use in an adolescent. Cureus, 2017. [DOI | PubMed]
- KA Meijer, RR Russo, DV Adhvaryu. Smoking synthetic marijuana leads to self-mutilation requiring bilateral amputations. Orthopedics, 2014. [DOI | PubMed]
- VT Mensen, A Vreeker, J Nordgren, A Atkinson, R De la Torre, M Farre, JG Ramaekers, TM Brunt. Psychopathological symptoms associated with synthetic cannabinoid use: a comparison with natural cannabis. Psychopharmacology, 2019. [DOI | PubMed]
- C Miliano, G Margiani, L Fattore, MA De Luca. Sales and advertising channels of new psychoactive substances (NPS): Internet, social networks, and smartphone apps. Brain Sci, 2018. [DOI]
- KJ Miller, DC Anderholm, MM Ames. Metabolic activation of the serotonergic neurotoxin para-chloroamphetamine to chemically reactive intermediates by hepatic and brain microsomal preparations. Biochem Pharmacol, 1986. [DOI | PubMed]
- EM Mills, ML Banks, JE Sprague, T Finkel. Pharmacology: uncoupling the agony from ecstasy. Nature, 2003. [DOI | PubMed]
- EM Mills, DE Rusyniak, JE Sprague. The role of the sympathetic nervous system and uncoupling proteins in the thermogenesis induced by 3,4-methylenedioxymethamphetamine. J Mol Med (Berl), 2004. [DOI | PubMed]
- B Mills, E Dishner, CE Velasco. Acute myocardial infarction triggered by use of synthetic cannabis. Proc (Bayl Univ Med Cent), 2018. [DOI | PubMed]
- A Mir, A Obafemi, A Young, C Kane. Myocardial infarction associated with use of the synthetic cannabinoid K2. Pediatrics, 2011. [DOI | PubMed]
- M Misra, Q Shi, X Ye, E Gruszecka-Kowalik, W Bu, Z Liu, MM Schweri, HM Deutsch, CA Venanzi. Quantitative structure-activity relationship studies of threo-methylphenidate analogs. Bioorg Med Chem, 2010. [DOI | PubMed]
- C Mitchell-Mata, B Thomas, B Peterson, F Couper. Two fatal intoxications involving 3-methoxyphencyclidine. J Anal Toxicol, 2017. [DOI | PubMed]
- MC Mithoefer, MT Wagner, AT Mithoefer, L Jerome, R Doblin. The safety and efficacy of ±3,4-methylenedioxymethamphetamine-assisted psychotherapy in subjects with chronic, treatment-resistant posttraumatic stress disorder: the first randomized controlled pilot study. J Psychopharmacol, 2011. [DOI | PubMed]
- MC Mithoefer, CS Grob, TD Brewerton. Novel psychopharmacological therapies for psychiatric disorders: psilocybin and MDMA. Lancet Psychiatry, 2016. [DOI | PubMed]
- M Miyajima, T Matsumoto, S Ito. 2C-T-4 intoxication: acute psychosis caused by a designer drug. Psychiatry Clin Neurosci, 2008. [DOI | PubMed]
- S Moeller, C Lücke, T Struffert, B Schwarze, ST Gerner, S Schwab, M Köhrmann, K Machold, A Philipsen, HH Müller. Ischemic stroke associated with the use of a synthetic cannabinoid (spice). Asian J Psychiatr, 2017. [DOI | PubMed]
- D Mohammed. Occurrence of takotsubo cardiomyopathy after synthetic cannabinoid consumption. Addict Health, 2019. [DOI | PubMed]
- AL Mohr, M Friscia, D Papsun, SL Kacinko, D Buzby, BK Logan. Analysis of novel synthetic opioids U-47700, U-50488 and furanyl fentanyl by LC–MS/MS in postmortem casework. J Anal Toxicol, 2016. [DOI | PubMed]
- AP Monte, D Marona-Lewicka, NV Cozzi, DE Nichols. Synthesis and pharmacological examination of benzofuran, indan, and tetralin analogues of 3,4-(methylenedioxy)amphetamine. J Med Chem, 1993. [DOI | PubMed]
- B Moosmann, V Auwärter. Designer benzodiazepines: another class of new psychoactive substances. Handb Exp Pharmacol, 2018. [DOI | PubMed]
- CJ Morgan, HV Curran. Acute and chronic effects of ketamine upon human memory: a review. Psychopharmacology, 2006. [DOI | PubMed]
- ML Moritz, K Kalantar-Zadeh, JC Ayus. Ecstacy-associated hyponatremia: why are women at risk?. Nephrol Dial Transplant, 2013. [DOI | PubMed]
- H Morris, J Wallach. From PCP to MXE: a comprehensive review of the non-medical use of dissociative drugs. Drug Test Anal, 2014. [DOI | PubMed]
- BL Morse, N Vijay, ME Morris. γ-Hydroxybutyrate (GHB)-induced respiratory depression: combined receptor-transporter inhibition therapy for treatment in GHB overdose. Mol Pharmacol, 2012. [DOI | PubMed]
- PR Moya, KA Berg, MA Gutierrez-Hernandez, P Saez-Briones, M Reyes-Parada, BK Cassels, WP Clarke. Functional selectivity of hallucinogenic phenethylamine and phenylisopropylamine derivatives at human 5-hydroxytryptamine (5-HT)2A and 5-HT2C receptors. J Pharmacol Exp Ther, 2007. [DOI | PubMed]
- AA Muller. New drugs of abuse update: Foxy Methoxy. J Emerg Nurs, 2004. [DOI | PubMed]
- H Müller, W Sperling, M Köhrmann, HB Huttner, J Kornhuber, JM Maler. The synthetic cannabinoid Spice as a trigger for an acute exacerbation of cannabis induced recurrent psychotic episodes. Schizophr Res, 2010. [DOI | PubMed]
- D Müller, H Neurath, MA Neukamm, M Wilde, C Despicht, S Blaschke, M Grapp. New synthetic opioid cyclopropylfentanyl together with other novel synthetic opioids in respiratory insufficient comatose patients detected by toxicological analysis. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- F Musshoff, B Madea, G Kernbach-Wighton, W Bicker, S Kneisel, M Hutter, V Auwärter. Driving under the influence of synthetic cannabinoids ("Spice"): a case series. Int J Legal Med, 2014. [DOI | PubMed]
- S Muttoni, M Ardissino, C John. Classical psychedelics for the treatment of depression and anxiety: a systematic review. J Affect Disord, 2019. [DOI | PubMed]
- N Nacca, D Vatti, R Sullivan, P Sud, M Su, J Marraffa. The synthetic cannabinoid withdrawal syndrome. J Addict Med, 2013. [DOI | PubMed]
- H Nagai, K Saka, M Nakajima, H Maeda, R Kuroda, A Igarashi, T Tsujimura-Ito, A Nara, M Komori, K Yoshida. Sudden death after sustained restraint following self-administration of the designer drug α-pyrrolidinovalerophenone. Int J Cardiol, 2014. [DOI | PubMed]
- C Nash, D Butzbach, P Stockham, T Scott, G Abroe, B Painter, J Gilbert, C Kostakis. A fatality involving furanylfentanyl and MMMP, with presumptive identification of three MMMP metabolites in urine. J Anal Toxicol, 2019. [DOI | PubMed]
- PT Nguyen, DK Dang, HQ Tran, EJ Shin, JH Jeong, SY Nah, MC Cho, YS Lee, CG Jang, HC Kim. Methiopropamine, a methamphetamine analogue, produces neurotoxicity via dopamine receptors. Chem Biol Interact, 2019. [DOI | PubMed]
- DE Nichols. Hallucinogens. Pharmacol Ther, 2004. [DOI | PubMed]
- DE Nichols. Psychedelics. Pharmacol Rev, 2016. [DOI | PubMed]
- DE Nichols, CS Grob. Is LSD toxic?. Forensic Sci Int, 2018. [DOI | PubMed]
- DE Nichols, MP Johnson, R Oberlender. 5-Iodo-2-aminoindan, a nonneurotoxic analogue of p-iodoamphetamine. Pharmacol Biochem Behav, 1991. [DOI | PubMed]
- M Niello, D Cintulova, E Hellsberg, K Jäntsch, M Holy, LH Ayatollahi, NV Cozzi, M Freissmuth, W Sandtner, GF Ecker, MD Mihovilovic, HH Sitte. para-Trifluoromethyl-methcathinone is an allosteric modulator of the serotonin transporter. Neuropharmacology, 2019. [DOI | PubMed]
- C Noble, NB Holm, M Mardal, K Linnet. Bromo-dragonfly, a psychoactive benzodifuran, is resistant to hepatic metabolism and potently inhibits monoamine oxidase A. Toxicol Lett, 2018. [DOI | PubMed]
- JJ Nugteren-van Lonkhuyzen, AJ Van Riel, TM Brunt, L Hondebrink. Pharmacokinetics, pharmacodynamics and toxicology of new psychoactive substances (NPS): 2C-B, 4-fluoroamphetamine and benzofurans. Drug Alcohol Depend, 2015. [DOI | PubMed]
- N Öcal, D Dogan, AF Cicek, O Yücel, E Tozkoparan. Acute eosinophilic pneumonia with respiratory failure induced by synthetic cannabinoid inhalation. Balkan Med J, 2016. [DOI | PubMed]
- I Ojanperä, M Gergov, I Rasanen, P Lunetta, S Toivonen, E Tiainen, E Vuori. Blood levels of 3-methylfentanyl in 3 fatal poisoning cases. Am J Forensic Med Pathol, 2006. [DOI | PubMed]
- P Oliveira, ASF Morais, N Madeira. Synthetic cannabis analogues and suicidal behavior: case report. J Addict Med, 2017. [DOI | PubMed]
- OO Oluwabusi, L Lobach, U Akhtar, B Youngman, PJ Ambrosini. Synthetic cannabinoid-induced psychosis: two adolescent cases. J Child Adolesc Psychopharmacol, 2012. [DOI | PubMed]
- L Orsolini, GD Papanti, D De Berardis, A Guirguis, JM Corkery, F Schifano. The "endless trip" among the NPS users: psychopathology and psychopharmacology in the hallucinogen-persisting perception disorder. A systematic review. Front Psychiatry, 2017. [DOI | PubMed]
- J Ott. Pharmahuasca: human pharmacology of oral DMT plus harmine. J Psychoact Drugs, 1999. [DOI]
- J Ott. Pharmepena-psychonautics: human intranasal, sublingual and oral pharmacology of 5-methoxy-NN-dimethyl-tryptamine. J Psychoact Drugs, 2001. [DOI]
- DR Owen, DM Wood, JR Archer, PI Dargan. Phenibut (4-amino-3-phenyl-butyric acid): availability, prevalence of use, desired effects and acute toxicity. Drug Alcohol Rev, 2016. [DOI | PubMed]
- HM Ozturk, E Yetkin, S Ozturk. Synthetic cannabinoids and cardiac arrhythmia risk: review of the literature. Cardiovasc Toxicol, 2019. [DOI | PubMed]
- T Palenicek, E Lhotkova, M Zidkova, M Balikova, M Kuchar, M Himl, P Miksatkova, M Cegan, K Vales, F Tyls, RR Horsley. Emerging toxicity of 5,6-methylenedioxy-2-aminoindane (MDAI): pharmacokinetics, behaviour, thermoregulation and LD50 in rats. Prog Neuropsychopharmacol Biol Psychiatry, 2016. [DOI | PubMed]
- F Palhano-Fontes, D Barreto, H Onias, KC Andrade, MM Novaes, JA Pessoa, SA Mota-Rolim, FL Osório, R Sanches, RG Dos Santos, LF Tófoli, SG de Oliveira, M Yonamine, J Riba, FR Santos, AA Silva-Junior, JC Alchieri, NL Galvão-Coelho, B Lobão-Soares, JEC Hallak, E Arcoverde, JP Maia-de-Oliveira, DB Aráujo. Rapid antidepressant effects of the psychedelic ayahuasca in treatment-resistant depression: a randomized placebo-controlled trial. Psychol Med, 2019. [DOI | PubMed]
- S Pant, A Deshmukh, B Dholaria, V Kaur, S Ramavaram, M Ukor, GA Teran. Spicy seizure. Am J Med Sci, 2012. [DOI | PubMed]
- D Papanti, F Schifano, G Botteon, F Bertossi, J Mannix, D Vidoni, M Impagnatiello, E Pascolo-Fabrici, T Bonavigo. "Spiceophrenia": a systematic overview of "spice"-related psychopathological issues and a case report. Hum Psychopharmacol, 2013. [DOI | PubMed]
- D Papsun, A Krywanczyk, JC Vose, EA Bundock, BK Logan. Analysis of MT-45, a novel synthetic opioid, in human whole blood by LC–MS–MS and its identification in a drug-related death. J Anal Toxicol, 2016. [DOI | PubMed]
- C Parks, D McKeown, HJ Torrance. A review of ethylphenidate in deaths in east and west Scotland. Forensic Sci Int, 2015. [DOI | PubMed]
- JS Partilla, AG Dempsey, AS Nagpal, BE Blough, MH Baumann, RB Rothman. Interaction of amphetamines and related compounds at the vesicular monoamine transporter. J Pharmacol Exp Ther, 2006. [DOI | PubMed]
- E Partridge, S Trobbiani, P Stockham, C Charlwood, C Kostakis. A case study involving U-47700, diclazepam and flubromazepam-application of retrospective analysis of HRMS data. J Anal Toxicol, 2018. [DOI | PubMed]
- AL Patton, KC Chimalakonda, CL Moran, KR McCain, A Radominska-Pandya, LP James, C Kokes, JH Moran. K2 toxicity: fatal case of psychiatric complications following AM2201 exposure. J Forensic Sci, 2013. [DOI | PubMed]
- ABM Paul, L Simms, S Amini, AE Paul. Teens and spice: a review of adolescent fatalities associated with synthetic cannabinoid use. J Forensic Sci, 2018. [DOI | PubMed]
- JM Pearson, TL Hargraves, LS Hair, CJ Massucci, CC Frazee, U Garg, BR Pietak. Three fatal intoxications due to methylone. J Anal Toxicol, 2012. [DOI | PubMed]
- S Peglow, J Buchner, G Briscoe. Synthetic cannabinoid induced psychosis in a previously nonpsychotic patient. Am J Addict, 2012. [DOI | PubMed]
- TM Penders, RE Gestring, DA Vilensky. Excited delirium following use of synthetic cathinones (bath salts). Gen Hosp Psychiatry, 2012. [DOI | PubMed]
- AB Peterson, RM Gladden, C Delcher, E Spies, A Garcia-Williams, Y Wang, J Halpin, J Zibbell, CL McCarty, J DeFiore-Hyrmer, M DiOrio, BA Goldberger. Increasses in fentanyl-related overdose deaths—Florida and Ohio, 2013–2015. MMWR Morb Mortal Wkly Rep, 2016. [DOI | PubMed]
- E Pieprzyca, R Skowronek, M Korczynska, J Kulikowska, M Chowaniec. A two fatal cases of poisoning involving new cathinone derivative PV8. Leg Med (Tokyo), 2018. [DOI | PubMed]
- N Pinterova, RR Horsley, T Palenicek. Synthetic aminoindanes: a summary of existing knowledge. Front Psychiatry, 2017. [DOI | PubMed]
- JL Poklis, CR Nanco, MM Troendle, CE Wolf, A Poklis. Determination of 4-bromo-2,5-dimethoxy-N-[(2-methoxyphenyl)methyl]-benzeneethanamine (25B-NBOMe) in serum and urine by high performance liquid chromatography with tandem mass spectrometry in a case of severe intoxication. Drug Test Anal, 2014. [DOI | PubMed]
- J Poklis, A Poklis, C Wolf, C Hathaway, E Arbefeville, L Chrostowski, K Devers, L Hair, M Mainland, M Merves, J Pearson. Two fatal intoxications involving butyryl fentanyl. J Anal Toxicol, 2016. [DOI | PubMed]
- M Poplawska, A Blazewicz. Identification of a novel growth hormone releasing peptide (a glycine analogue of GHRP-2) in a seized injection vial. Drug Test Anal, 2019. [DOI | PubMed]
- B Potocka-Banas, T Janus, S Majdanik, T Banas, T Dembinska, K Borowiak. Fatal intoxication with α-PVP, a synthetic cathinone derivative. J Forensic Sci, 2017. [DOI | PubMed]
- MP Prekupec, PA Mansky, MH Baumann. Misuse of novel synthetic opioids: a deadly new trend. J Addict Med, 2017. [DOI | PubMed]
- KH Preller, M Herdener, T Pokorny, A Planzer, R Kraehenmann, P Stämpfli, ME Liechti, E Seifritz, FX Vollenweider. The fabric of meaning and subjective effects in LSD-induced states depend on serotonin 2A receptor activation. Curr Biol, 2017. [DOI | PubMed]
- KH Preller, JB Burt, JL Ji, CH Schleifer, BD Adkinson, P Stämpfli, E Seifritz, G Repovs, JH Krystal, JD Murray, FX Vollenweider, A Anticevic. Changes in global and thalamic brain connectivity in LSD-induced altered states of consciousness are attributable to the 5-HT2A receptor. Elife, 2018. [DOI | PubMed]
- A Raheemullah, TN Laurence. Repeated thrombosis after synthetic cannabinoid use. J Emerg Med, 2016. [DOI | PubMed]
- CD Rahnema, LE Crosnoe, ED Kim. Designer steroids—over-the-counter supplements and their androgenic component: review of an increasing problem. Andrology, 2015. [DOI | PubMed]
- J Riba, EH McIlhenny, JC Bouso, SA Barker. Metabolism and urinary disposition of N,N-dimethyltryptamine after oral and smoked administration: a comparative study. Drug Test Anal, 2015. [DOI | PubMed]
- JR Richards, EB Johnson, RW Stark, RW Derlet. Methamphetamine abuse and rhabdomyolysis in the ED: a 5-year study. Am J Emerg Med, 1999. [DOI | PubMed]
- C Richeval, JM Gaulier, L Romeuf, D Allorge, Y Gaillard. Case report: relevance of metabolite identification to detect new synthetic opioid intoxications illustrated by U-47700. Int J Legal Med, 2019. [DOI | PubMed]
- A Rickli, MC Hoener, ME Liechti. Monoamine transporter and receptor interaction profiles of novel psychoactive substances: para-halogenated amphetamines and pyrovalerone cathinones. Eur Neuropsychopharmacol, 2015. [DOI | PubMed]
- A Rickli, S Kopf, MC Hoener, ME Liechti. Pharmacological profile of novel psychoactive benzofurans. Br J Pharmacol, 2015. [DOI | PubMed]
- A Rickli, D Luethi, J Reinisch, D Buchy, MC Hoener, ME Liechti. Receptor interaction profiles of novel N-2-methoxybenzyl (NBOMe) derivatives of 2,5-dimethoxy-substituted phenethylamines (2C drugs). Neuropharmacology, 2015. [DOI | PubMed]
- A Rickli, OD Moning, MC Hoener, ME Liechti. Receptor interaction profiles of novel psychoactive tryptamines compared with classic hallucinogens. Eur Neuropsychopharmacol, 2016. [DOI | PubMed]
- A Rickli, E Liakoni, MC Hoener, ME Liechti. Opioid-induced inhibition of the human 5-HT and noradrenaline transporters in vitro: link to clinical reports of serotonin syndrome. Br J Pharmacol, 2018. [DOI | PubMed]
- A Rickli, K Kolaczynska, MC Hoener, ME Liechti. Pharmacological characterization of the aminorex analogs 4-MAR, 4,4ʹ-DMAR, and 3,4-DMAR. Neurotoxicology, 2019. [DOI | PubMed]
- MC Ritz, RJ Lamb, SR Goldberg, MJ Kuhar. Cocaine receptors on dopamine transporters are related to self-administration of cocaine. Science, 1987. [DOI | PubMed]
- AJ Roberto, A Lorenzo, KJ Li, J Young, A Mohan, S Pinnaka, KA Lapidus. First-episode of synthetic cannabinoid-induced psychosis in a young adult, successfully managed with hospitalization and risperidone. Case Rep Psychiatry, 2016. [DOI | PubMed]
- R Roque Bravo, H Carmo, JP Silva, MJ Valente, F Carvalho, ML Bastos, D Dias da Silva. Emerging club drugs: 5-(2-aminopropyl)benzofuran (5-APB) is more toxic than its isomer 6-(2-aminopropyl)benzofuran (6-APB) in hepatocyte cellular models. Arch Toxicol, 2019. [DOI | PubMed]
- SR Rose, JL Poklis, A Poklis. A case of 25I-NBOMe (25-I) intoxication: a new potent 5-HT2A agonist designer drug. Clin Toxicol (Phila), 2013. [DOI | PubMed]
- DZ Rose, WR Guerrero, MV Mokin, CL Gooch, AC Bozeman, JM Pearson, WS Burgin. Hemorrhagic stroke following use of the synthetic marijuana "spice". Neurology, 2015. [DOI | PubMed]
- L Roseman, DJ Nutt, RL Carhart-Harris. Quality of acute psychedelic experience predicts therapeutic efficacy of psilocybin for treatment-resistant depression. Front Pharmacol, 2017. [DOI | PubMed]
- J Rosenson, C Smollin, KA Sporer, P Blanc, KR Olson. Patterns of ecstasy-associated hyponatremia in California. Ann Emerg Med, 2007. [DOI | PubMed]
- EA Ross, M Watson, B Goldberger. "Bath salts" intoxication. N Engl J Med, 2011. [DOI | PubMed]
- EA Ross, GM Reisfield, MC Watson, CW Chronister, BA Goldberger. Psychoactive "bath salts" intoxication with methylenedioxypyrovalerone. Am J Med, 2012. [DOI | PubMed]
- BL Roth. Drugs and valvular heart disease. N Engl J Med, 2007. [DOI | PubMed]
- BL Roth, S Gibbons, W Arunotayanun, XP Huang, V Setola, R Treble, L Iversen. The ketamine analogue methoxetamine and 3- and 4-methoxy analogues of phencyclidine are high affinity and selective ligands for the glutamate NMDA receptor. PLoS ONE, 2013. [DOI | PubMed]
- RB Rothman, MH Baumann. Monoamine transporters and psychostimulant drugs. Eur J Pharmacol, 2003. [DOI | PubMed]
- RB Rothman, MH Baumann, CM Dersch, DV Romero, KC Rice, FI Carroll, JS Partilla. Amphetamine-type central nervous system stimulants release norepinephrine more potently than they release dopamine and serotonin. Synapse, 2001. [DOI | PubMed]
- RB Rothman, M Katsnelson, N Vu, JS Partilla, CM Dersch, BE Blough, MH Baumann. Interaction of the anorectic medication, phendimetrazine, and its metabolites with monoamine transporters in rat brain. Eur J Pharmacol, 2002. [DOI | PubMed]
- X Ruan, S Chiravuri, AD Kaye. Comparing fatal cases involving U-47700. Forensic Sci Med Pathol, 2016. [DOI | PubMed]
- RA Rudd, P Seth, F David, L Scholl. Increases in drug and opioid-involved overdose deaths—United States, 2010–2015. MMWR Morb Mortal Wkly Rep, 2016. [DOI | PubMed]
- S Sachdev, K Vemuri, SD Banister, M Longworth, M Kassiou, M Santiago, A Makriyannis, M Connor. In vitro determination of the CB1 efficacy of illicit synthetic cannabinoids. Br J Pharmacol, 2019. [DOI | PubMed]
- PD Sainsbury, AT Kicman, RP Archer, LA King, RA Braithwaite. Aminoindanes—the next wave of ‘legal highs’?. Drug Test Anal, 2011. [DOI | PubMed]
- T Saito, A Namera, N Miura, S Ohta, S Miyazaki, M Osawa, S Inokuchi. A fatal case of MAM-2201 poisoning. Forensic Toxicol, 2013. [DOI]
- CS Sampson, SM Bedy, T Carlisle. Withdrawal seizures seen in the setting of synthetic cannabinoid abuse. Am J Emerg Med, 2015. [DOI | PubMed]
- S Sanchez. Sur un homologue de l’éphédrine. Bull Soc Chim Fr, 1929
- LJ Schep, RJ Slaughter, JA Vale, DM Beasley, P Gee. The clinical toxicology of the designer "party pills" benzylpiperazine and trifluoromethylphenylpiperazine. Clin Toxicol (Phila), 2011. [DOI | PubMed]
- LJ Schep, K Knudsen, RJ Slaughter, JA Vale, B Mégarbane. The clinical toxicology of gamma-hydroxybutyrate, gamma-butyrolactone and 1,4-butanediol. Clin Toxicol (Phila), 2012. [DOI | PubMed]
- LJ Schep, RJ Slaughter, S Hudson, R Place, M Watts. Delayed seizure-like activity following analytically confirmed use of previously unreported synthetic cannabinoid analogues. Hum Exp Toxicol, 2015. [DOI | PubMed]
- F Schifano, J Corkery, AH Ghodse. Suspected and confirmed fatalities associated with mephedrone (4-methylmethcathinone, "meow meow") in the United Kingdom. J Clin Psychopharmacol, 2012. [DOI | PubMed]
- Y Schmid, F Enzler, P Gasser, E Grouzmann, KH Preller, FX Vollenweider, R Brenneisen, F Müller, S Borgwardt, ME Liechti. Acute effects of lysergic acid diethylamide in healthy subjects. Biol Psychiatry, 2015. [DOI | PubMed]
- AB Schneir, T Baumbacher. Convulsions associated with the use of a synthetic cannabinoid product. J Med Toxicol, 2012. [DOI | PubMed]
- A Schneir, IG Metushi, C Sloane, DJ Benaron, RL Fitzgerald. Near death from a novel synthetic opioid labeled U-47700: emergence of a new opioid class. Clin Toxicol (Phila), 2017. [DOI | PubMed]
- L Scholl, P Seth, M Kariisa, N Wilson, G Baldwin. Drug and opioid-involved overdose deaths—United States, 2013–2017. MMWR Morb Mortal Wkly Rep, 2018. [DOI | PubMed]
- MD Schwartz, J Trecki, LA Edison, AR Steck, JK Arnold, RR Gerona. A common source outbreak of severe delirium associated with exposure to the novel synthetic cannabinoid ADB-PINACA. J Emerg Med, 2015. [DOI | PubMed]
- GR Screaton, M Singer, HS Cairns, A Thrasher, M Sarner, SL Cohen. Hyperpyrexia and rhabdomyolysis after MDMA ("ecstasy") abuse. Lancet, 1992. [DOI | PubMed]
- DA Seaton, LJ Duncan, K Rose, AM Scott. Diethyl-propion in the treatment of “refractory” obesity. Br Med J, 1961. [DOI | PubMed]
- LN Seetohul, DJ Pounder. Four fatalities involving 5-IT. J Anal Toxicol, 2013. [DOI | PubMed]
- JZ Seither, LJ Reidy, DM Boland. Identification and quantification of 5-fluoro ADB and the 5-fluoro ADB ester hydrolysis metabolite in postmortem blood samples by LC–MS/MS. J Anal Toxicol, 2019. [DOI | PubMed]
- K Sellors, A Jones, B Chan. Death due to intravenous use of α-pyrrolidinopentiophenone. Med J Aust, 2014. [DOI | PubMed]
- JY Seo, KH Hur, YH Ko, K Kim, BR Lee, YJ Kim, SK Kim, SE Kim, YS Lee, HC Kim, SY Lee, CG Jang. A novel designer drug, 25N-NBOMe, exhibits abuse potential via the dopaminergic system in rodents. Brain Res Bull, 2019. [DOI | PubMed]
- P Seth, L Scholl, RA Rudd, S Bacon. Overdose deaths involving opioids, cocaine, and psychostimulants—United States, 2015–2016. MMWR Morb Mortal Wkly Rep, 2018. [DOI | PubMed]
- V Setola, SJ Hufeisen, KJ Grande-Allen, I Vesely, RA Glennon, B Blough, RB Rothman, BL Roth. 3,4-methylenedioxymethamphetamine (MDMA, "Ecstasy") induces fenfluramine-like proliferative actions on human cardiac valvular interstitial cells in vitro. Mol Pharmacol, 2003. [DOI | PubMed]
- M Shah, J Garg, B Patel, J Guthier, RS Freudenberger. Can your heart handle the spice: a case of acute myocardial infarction and left ventricular apical thrombus. Int J Cardiol, 2016. [DOI | PubMed]
- A Shahbaz, REE Gaviria, MF Shahid, MA Yasin, A Ashraf, MA Zaman. Acute liver injury induced by synthetic cannabinoid abuse. Cureus, 2018. [DOI | PubMed]
- KG Shanks, GS Behonick. Death after use of the synthetic cannabinoid 5F-AMB. Forensic Sci Int, 2016. [DOI | PubMed]
- KG Shanks, T Dahn, AR Terrell. Detection of JWH-018 and JWH-073 by UPLC–MS–MS in postmortem whole blood casework. J Anal Toxicol, 2012. [DOI | PubMed]
- KG Shanks, T Sozio, GS Behonick. Fatal intoxications with 25B-NBOMe and 25I-NBOMe in Indiana during 2014. J Anal Toxicol, 2015. [DOI | PubMed]
- KG Shanks, D Winston, J Heidingsfelder, G Behonick. Case reports of synthetic cannabinoid XLR-11 associated fatalities. Forensic Sci Int, 2015. [DOI | PubMed]
- KG Shanks, W Clark, G Behonick. Death associated with the use of the synthetic cannabinoid ADB-FUBINACA. J Anal Toxicol, 2016. [DOI | PubMed]
- A Sharma, J Couture. A review of the pathophysiology, etiology, and treatment of attention-deficit hyperactivity disorder (ADHD). Ann Pharmacother, 2014. [DOI | PubMed]
- K Shearer, C Bryce, M Parsons, H Torrance. Phenazepam: a review of medico-legal deaths in South Scotland between 2010 and 2014. Forensic Sci Int, 2015. [DOI | PubMed]
- J Sheridan, R Butler, C Wilkins, B Russell. Legal piperazine-containing party pills—a new trend in substance misuse. Drug Alcohol Rev, 2007. [DOI | PubMed]
- D Sherpa, BM Paudel, BH Subedi, RD Chow. Synthetic cannabinoids: the multi-organ failure and metabolic derangements associated with getting high. J Community Hosp Intern Med Perspect, 2015. [DOI | PubMed]
- JE Shields, PI Dargan, DM Wood, M Puchnarewicz, S Davies, WS Waring. Methoxetamine associated reversible cerebellar toxicity: three cases with analytical confirmation. Clin Toxicol (Phila), 2012. [DOI | PubMed]
- EN Shoff, JH Kahl, GW Hime, M Coburn, DM Boland. 4-Fluoromethylphenidate: fatal intoxication involving a previously unreported novel psychoactive substance in the USA. J Anal Toxicol, 2019. [DOI | PubMed]
- A Shulgin, A Shulgin. PIHKAL: a chemical love story, 1995
- A Shulgin, A Shulgin. TIHKAL: the continuation, 1997
- S Siddiqi, C Verney, P Dargan, DM Wood. Understanding the availability, prevalence of use, desired effects, acute toxicity and dependence potential of the novel opioid MT-45. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- JP Silva, H Carmo, F Carvalho. The synthetic cannabinoid XLR-11 induces in vitro nephrotoxicity by impairment of endocannabinoid-mediated regulation of mitochondrial function homeostasis and triggering of apoptosis. Toxicol Lett, 2018. [DOI | PubMed]
- JP Silva, AM Araújo, PG De Pinho, H Carmo, F Carvalho. Synthetic cannabinoids JWH-122 and THJ-2201 disrupt endocannabinoid-regulated mitochondrial function and activate apoptotic pathways as a primary mechanism of in vitro nephrotoxicity at in vivo relevant concentrations. Toxicol Sci, 2019. [DOI | PubMed]
- LD Simmler, CM Hysek, ME Liechti. Sex differences in the effects of MDMA (ecstasy) on plasma copeptin in healthy subjects. J Clin Endocrinol Metab, 2011. [DOI | PubMed]
- LD Simmler, TA Buser, M Donzelli, Y Schramm, LH Dieu, J Huwyler, S Chaboz, MC Hoener, ME Liechti. Pharmacological characterization of designer cathinones in vitro. Br J Pharmacol, 2013. [DOI | PubMed]
- LD Simmler, A Rickli, MC Hoener, ME Liechti. Monoamine transporter and receptor interaction profiles of a new series of designer cathinones. Neuropharmacology, 2014. [DOI | PubMed]
- LD Simmler, A Rickli, Y Schramm, MC Hoener, ME Liechti. Pharmacological profiles of aminoindanes, piperazines, and pipradrol derivatives. Biochem Pharmacol, 2014. [DOI | PubMed]
- LD Simmler, D Buchy, S Chaboz, MC Hoener, ME Liechti. In vitro characterization of psychoactive substances at rat, mouse, and human trace amine-associated receptor 1. J Pharmacol Exp Ther, 2016. [DOI | PubMed]
- HH Sitte, M Freissmuth. Amphetamines, new psychoactive drugs and the monoamine transporter cycle. Trends Pharmacol Sci, 2015. [DOI | PubMed]
- J Sklerov, B Levine, KA Moore, T King, D Fowler. A fatal intoxication following the ingestion of 5-methoxy-N,N-dimethyltryptamine in an ayahuasca preparation. J Anal Toxicol, 2005. [DOI | PubMed]
- VY Skryabin, MA Vinnikova. Clinical characteristics of synthetic cannabinoid-induced psychotic disorders: a single-center analysis of hospitalized patients. J Addict Dis, 2019. [DOI]
- VY Skryabin, M Vinnikova, A Nenastieva, V Alekseyuk. Hallucinogen persisting perception disorder: a literature review and three case reports. J Addict Dis, 2019. [DOI]
- DL Smith, C Roberts. Synthetic marijuana use and development of catatonia in a 17-year-old male. Minn Med, 2014. [PubMed]
- SC Smolinske, R Rastogi, S Schenkel. Foxy methoxy: a new drug of abuse. J Med Toxicol, 2005. [DOI | PubMed]
- S Sofalvi, HE Schueler, ES Lavins, CK Kaspar, IT Brooker, CD Mazzola, D Dolinak, TP Gilson, S Perch. An LC–MS-MS method for the analysis of carfentanil, 3-methylfentanyl, 2-furanyl fentanyl, acetyl fentanyl, fentanyl and norfentanyl in postmortem and impaired-driving cases. J Anal Toxicol, 2017. [DOI | PubMed]
- E Solomons, J Sam. 2-Aminoindans of pharmacological interest. J Med Chem, 1973. [DOI | PubMed]
- FE Soroko, NB Mehta, RA Maxwell, RM Ferris, DH Schroeder. Bupropion hydrochloride ((±) α-t-butylamino-3-chloropropiophenone HCl): a novel antidepressant agent. J Pharm Pharmacol, 1977. [DOI | PubMed]
- S Srisuma, AC Bronstein, CO Hoyte. NBOMe and 2C substitute phenylethylamine exposures reported to the National Poison Data System. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- W Srisung, F Jamal, S Prabhakar. Synthetic cannabinoids and acute kidney injury. Proc (Bayl Univ Med Cent), 2015. [DOI | PubMed]
- SN Staeheli, MR Baumgartner, S Gauthier, D Gascho, J Jarmer, T Kraemer, AE Steuer. Time-dependent postmortem redistribution of butyrfentanyl and its metabolites in blood and alternative matrices in a case of butyrfentanyl intoxication. Forensic Sci Int, 2016. [DOI | PubMed]
- TH Stanley. The fentanyl story. J Pain, 2014. [DOI | PubMed]
- SJ Stellpflug, SE Kealey, CB Hegarty, GC Janis. 2-(4-Iodo-2,5-dimethoxyphenyl)-N-[(2-methoxyphenyl)methyl]ethanamine (25I-NBOMe): clinical case with unique confirmatory testing. J Med Toxicol, 2014. [DOI | PubMed]
- LH Sternbach. The benzodiazepine story. J Med Chem, 1979. [DOI | PubMed]
- A Stoller, PC Dolder, M Bodmer, F Hammann, KM Rentsch, AK Exadaktylos, ME Liechti, E Liakoni. Mistaking 2C-P for 2C-B: what a difference a letter makes. J Anal Toxicol, 2017. [DOI | PubMed]
- JA Suyama, ML Banks, SS Negus. Effects of repeated treatment with methcathinone, mephedrone, and fenfluramine on intracranial self-stimulation in rats. Psychopharmacology, 2019. [DOI | PubMed]
- J Suzuki, S El-Haddad. A review: fentanyl and non-pharmaceutical fentanyls. Drug Alcohol Depend, 2017. [DOI | PubMed]
- DM Swanson, LS Hair, SR Strauch Rivers, BC Smyth, SC Brogan, AD Ventoso, SL Vaccaro, JM Pearson. Fatalities involving carfentanil and furanyl fentanyl: two case reports. J Anal Toxicol, 2017. [DOI | PubMed]
- B Sweeney, S Talebi, D Toro, K Gonzalez, JP Menoscal, R Shaw, GW Hassen. Hyperthermia and severe rhabdomyolysis from synthetic cannabinoids. Am J Emerg Med, 2016. [DOI]
- G Sweet, S Kim, S Martin, NB Washington, N Brahm. Psychiatric symptoms and synthetic cannabinoid use: information for clinicians. Ment Health Clin, 2017. [DOI | PubMed]
- RJ Tait, D Caldicott, D Mountain, SL Hill, S Lenton. A systematic review of adverse events arising from the use of synthetic cannabinoids and their associated treatment. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- I Takase, T Koizumi, I Fujimoto, A Yanai, T Fujimiya. An autopsy case of acetyl fentanyl intoxication caused by insufflation of ‘designer drugs’. Leg Med (Tokyo), 2016. [DOI | PubMed]
- M Takematsu, RS Hoffman, LS Nelson, JM Schechter, JH Moran, SW Wiener. A case of acute cerebral ischemia following inhalation of a synthetic cannabinoid. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- J Taljemark, BA Johansson. Drug-induced acute psychosis in an adolescent first-time user of 4-HO-MET. Eur Child Adolesc Psychiatry, 2012. [DOI | PubMed]
- E Tanaka, T Kamata, M Katagi, H Tsuchihashi, K Honda. A fatal poisoning with 5-methoxy-N,N-diisopropyltryptamine. Foxy Forensic Sci Int, 2006. [DOI | PubMed]
- N Tanaka, H Kinoshita, M Jamal, E Ohkubo, M Kumihashi, K Ameno. A case of drowning whilst under the influence of brotizolam, flunitrazepam and ethanol. Soud Lek, 2011. [PubMed]
- N Tanaka, H Kinoshita, M Nishiguchi, M Jamal, M Kumihashi, M Takahashi, H Nishio, K Ameno. An autopsy case of multiple psychotropic drug poisoning. Soud Lek, 2011. [PubMed]
- MH Tang, CK Ching, MS Tsui, FK Chu, TW Mak. Two cases of severe intoxication associated with analytically confirmed use of the novel psychoactive substances 25B-NBOMe and 25C-NBOMe. Clin Toxicol (Phila), 2014. [DOI | PubMed]
- P Thirakul, LS Hair, KL Bergen, JM Pearson. Clinical presentation, autopsy results and toxicology findings in an acute N-ethylpentylone fatality. J Anal Toxicol, 2017. [DOI | PubMed]
- S Thomas, S Bliss, M Malik. Suicidal ideation and self-harm following K2 use. J Okla State Med Assoc, 2012. [PubMed]
- Thorlacius K, Borna C, Personne M (2008) Bromo-dragonfly–livsfarlig missbruksdrog. Kan ge vävnadsnekros, visar det första beskrivna fallet. Lakartidningen 105(16):1199–200
- SL Thornton, C Wood, MW Friesen, RR Gerona. Synthetic cannabinoid use associated with acute kidney injury. Clin Toxicol (Phila), 2013. [DOI | PubMed]
- S Thornton, D Lisbon, T Lin, R Gerona. Beyond ketamine and phencyclidine: analytically confirmed use of multiple novel arylcyclohexylamines. J Psychoactive Drugs, 2017. [DOI | PubMed]
- B Tofighi, JD Lee. Internet highs–seizures after consumption of synthetic cannabinoids purchased online. J Addict Med, 2012. [DOI | PubMed]
- J Topeff, H Ellsworth, L Willhite, S Bangh, E Edwards, J Cole. A case series of symptomatic patients, including one fatality, following 2C-E exposure. Clin Toxicol (Phila), 2011
- D Trachsel, D Lehmann, C Enzensperger. Phenethylamine: von der Struktur zur Funktion, 2013
- J Trecki, RR Gerona, MD Schwartz. Synthetic cannabinoid-related illnesses and deaths. N Engl J Med, 2015. [DOI | PubMed]
- F Troxler, A Hofmann. Substitutionen am Ringsystem der Lysergsäure. I Substitutionen am Indol-Stickstoff. 43. Mitteilung über Mutterkornalkaloide. Helv Chim Acta, 1957. [DOI]
- TH Tsai, TL Cha, CM Lin, CW Tsao, SH Tang, FP Chuang, ST Wu, GH Sun, DS Yu, SY Chang. Ketamine-associated bladder dysfunction. Int J Urol, 2009. [DOI | PubMed]
- R Tse, S Kodur, B Squires, N Collins. Sudden cardiac death complicating acute myocardial infarction following synthetic cannabinoid use. Intern Med J, 2014. [DOI | PubMed]
- JA Tyndall, R Gerona, G De Portu, J Trecki, MC Elie, J Lucas, J Slish, K Rand, L Bazydlo, M Holder, MF Ryan, P Myers, N Iovine, M Plourde, E Weeks, JR Hanley, G Endres, D St Germaine, PJ Dobrowolski, M Schwartz. An outbreak of acute delirium from exposure to the synthetic cannabinoid AB-CHMINACA. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- A Ukaigwe, P Karmacharya, A Donato. A gut gone to pot: a case of cannabinoid hyperemesis syndrome due to K2, a synthetic cannabinoid. Case Rep Emerg Med, 2014. [DOI | PubMed]
- R Umebachi, H Aoki, M Sugita, T Taira, S Wakai, T Saito, S Inokuchi. Clinical characteristics of α-pyrrolidinovalerophenone (α-PVP) poisoning. Clin Toxicol (Phila), 2016. [DOI | PubMed]
- K Usui, Y Fujita, Y Kamijo, T Kokaji, M Funayama. Identification of 5-fluoro ADB in human whole blood in four death cases. J Anal Toxicol, 2018. [DOI | PubMed]
- MJ Valente, P Guedes de Pinho, BM De Lourdes, F Carvalho, M Carvalho. Khat and synthetic cathinones: a review. Arch Toxicol, 2014. [DOI | PubMed]
- MJ Valente, AM Aráujo, L Bastos Mde, E Fernandes, F Carvalho, P Guedes de Pinho, M Carvalho. characterization of hepatotoxicity mechanisms triggered by designer cathinone drugs (β-keto amphetamines). Toxicol Sci, 2016. [DOI | PubMed]
- MJ Valente, AM Aráujo, R Silva, L Bastos Mde, F Carvalho, P Guedes de Pinho, M Carvalho. 3,4-Methylenedioxypyrovalerone (MDPV): in vitro mechanisms of hepatotoxicity under normothermic and hyperthermic conditions. Arch Toxicol, 2016. [DOI | PubMed]
- MJ Valente, C Amaral, G Correia-da-Silva, JA Duarte, ML Bastos, F Carvalho, P Guedes de Pinho, M Carvalho. Methylone and MDPV activate autophagy in human dopaminergic SH-SY5Y cells: a new insight into the context of β-keto amphetamines-related neurotoxicity. Arch Toxicol, 2017. [DOI | PubMed]
- MJ Valente, ML Bastos, E Fernandes, F Carvalho, P Guedes de Pinho, M Carvalho. Neurotoxicity of β-keto amphetamines: deathly mechanisms elicited by methylone and MDPV in human dopaminergic SH-SY5Y cells. ACS Chem Neurosci, 2017. [DOI | PubMed]
- J Van Amsterdam, T Brunt, W Van den Brink. The adverse health effects of synthetic cannabinoids with emphasis on psychosis-like effects. J Psychopharmacol, 2015. [DOI | PubMed]
- High incidence of mild hyponatraemia in females using ecstasy at a rave party. Nephrol Dial Transplant, 2013. [DOI | PubMed]
- H Vanden Eede, LJ Montenij, DJ Touw, EM Norris. Rhabdomyolysis in MDMA intoxication: a rapid and underestimated killer. “Clean" ecstasy, a safe party drug?. J Emerg Med, 2012. [DOI | PubMed]
- SA Vandewater, KM Creehan, MA Taffe. Intravenous self-administration of entactogen-class stimulants in male rats. Neuropharmacology, 2015. [DOI | PubMed]
- N Van der Veer, J Friday. Persistent psychosis following the use of Spice. Schizophr Res, 2011. [DOI | PubMed]
- BJ Venhuis, L Blok-Tip, D De Kaste. Designer drugs in herbal aphrodisiacs. Forensic Sci Int, 2008. [DOI | PubMed]
- P Vizeli, ME Liechti. Safety pharmacology of acute MDMA administration in healthy subjects. J Psychopharmacol, 2017. [DOI | PubMed]
- M Vogel, B Knöpfli, O Schmid, M Prica, J Strasser, L Prieto, GA Wiesbeck, KM Dursteler-Macfarland. Treatment or "high": benzodiazepine use in patients on injectable heroin or oral opioids. Addict Behav, 2013. [DOI | PubMed]
- M Vogel, P Bucher, J Strasser, ME Liechti, S Krähenbühl, KM Dürsteler. Similar and different? Subjective effects of methylphenidate and cocaine in opioid-maintained patients. J Psychoactive Drugs, 2016. [DOI | PubMed]
- FX Vollenweider, MF Vollenweider-Scherpenhuyzen, A Bäbler, H Vogel, D Hell. Psilocybin induces schizophrenia-like psychosis in humans via a serotonin-2 agonist action. NeuroReport, 1998. [DOI | PubMed]
- TJ Volz, GR Hanson, AE Fleckenstein. The role of the plasmalemmal dopamine and vesicular monoamine transporters in methamphetamine-induced dopaminergic deficits. J Neurochem, 2007. [DOI | PubMed]
- SP Vorce, JL Knittel, JM Holler, J Magluilo, B Levine, P Berran, TZ Bosy. A fatality involving AH-7921. J Anal Toxicol, 2014. [DOI | PubMed]
- L Wagmann, SD Brandt, A Stratford, HH Maurer, MR Meyer. Interactions of phenethylamine-derived psychoactive substances of the 2C-series with human monoamine oxidases. Drug Test Anal, 2019. [DOI | PubMed]
- L Wagmann, LHJ Richter, T Kehl, F Wack, MP Bergstrand, SD Brandt, A Stratford, HH Maurer, MR Meyer. In vitro metabolic fate of nine LSD-based new psychoactive substances and their analytical detectability in different urinary screening procedures. Anal Bioanal Chem, 2019. [DOI | PubMed]
- J Wallach, SD Brandt. 1,2-diarylethylamine- and ketamine-based new psychoactive substances. Handb Exp Pharmacol, 2018. [DOI | PubMed]
- J Wallach, SD Brandt. Phencyclidine-based new psychoactive substances. Handb Exp Pharmacol, 2018. [DOI | PubMed]
- J Wallach, H Kang, T Colestock, H Morris, ZA Bortolotto, GL Collingridge, D Lodge, AL Halberstadt, SD Brandt, A Adejare. Pharmacological investigations of the dissociative ‘legal highs’ diphenidine, methoxphenidine and analogues. PLoS ONE, 2016. [DOI | PubMed]
- JP Walterscheid, GT Phillips, AE Lopez, ML Gonsoulin, HH Chen, LA Sanchez. Pathological findings in 2 cases of fatal 25I-NBOMe toxicity. Am J Forensic Med Pathol, 2014. [DOI | PubMed]
- Q Wang, Q Wu, J Wang, Y Chen, G Zhang, J Chen, J Zhao, P Wu. Ketamine analog methoxetamine induced inflammation and dysfunction of bladder in rats. Int J Mol Sci, 2017. [DOI]
- J Ward, S Rhyee, J Plansky, E Boyer. Methoxetamine: a novel ketamine analog and growing health-care concern. Clin Toxicol (Phila), 2011. [DOI | PubMed]
- L Waters, KR Manchester, PD Maskell, C Haegeman, S Haider. The use of a quantitative structure-activity relationship (QSAR) model to predict GABA-A receptor binding of newly emerging benzodiazepines. Sci Justice, 2018. [DOI | PubMed]
- C Weber, O Krug, M Kamber, M Thevis. Qualitative and semiquantitative analysis of doping products seized at the Swiss border. Subst Use Misuse, 2017. [DOI | PubMed]
- S Wee, WL Woolverton. Self-administration of mixtures of fenfluramine and amphetamine by rhesus monkeys. Pharmacol Biochem Behav, 2006. [DOI | PubMed]
- S Wee, KG Anderson, MH Baumann, RB Rothman, BE Blough, WL Woolverton. Relationship between the serotonergic activity and reinforcing effects of a series of amphetamine analogs. J Pharmacol Exp Ther, 2005. [DOI | PubMed]
- S Welter, C Lücke, AP Lam, C Custal, S Moeller, P Sörös, CM Thiel, A Philipsen, HHO Müller. Synthetic cannabinoid use in a psychiatric patient population: a pilot study. Eur Addict Res, 2017. [DOI | PubMed]
- AA Westin, J Frost, WR Brede, PO Gundersen, S Einvik, H Aarset, L Slordal. Sudden cardiac death following use of the synthetic cannabinoid MDMB-CHMICA. J Anal Toxicol, 2016. [DOI | PubMed]
- JC White, DM Wood, SL Hill, M Eddleston, J Officer, PI Dargan, M Dunn, SHL Thomas. Acute toxicity following analytically confirmed use of the novel psychoactive substance (NPS) methiopropamine. A report from the Identification of Novel psychoActive substances (IONA) study. Clin Toxicol (Phila), 2019. [DOI | PubMed]
- M Wiergowski, JS Anand, M Krzyzanowski, Z Jankowski. Acute methoxetamine and amphetamine poisoning with fatal outcome: a case report. Int J Occup Med Environ Health, 2014. [DOI | PubMed]
- CH Wijers, RT Van Litsenburg, L Hondebrink, RJ Niesink, EA Croes. Acute toxic effects related to 4-fluoroamphetamine. Lancet, 2017. [DOI | PubMed]
- M Wikström, G Thelander, M Dahlgren, R Kronstrand. An accidental fatal intoxication with methoxetamine. J Anal Toxicol, 2013. [DOI | PubMed]
- M Wilde, MJ Sommer, V Auwärter, M Hermanns-Clausen. Acute severe intoxication with cyclopropylfentanyl, a novel synthetic opioid. Toxicol Lett, 2020. [DOI | PubMed]
- JL Wiley, TW Lefever, JA Marusich, M Grabenauer, KN Moore, JW Huffman, BF Thomas. Evaluation of first generation synthetic cannabinoids on binding at non-cannabinoid receptors and in a battery of in vivo assays in mice. Neuropharmacology, 2016. [DOI | PubMed]
- C Wilkins, P Sweetsur, M Girling. Patterns of benzylpiperazine/trifluoromethylphenylpiperazine party pill use and adverse effects in a population sample in New Zealand. Drug Alcohol Rev, 2008. [DOI | PubMed]
- AR Winstock, MJ Barratt. Synthetic cannabis: a comparison of patterns of use and effect profile with natural cannabis in a large global sample. Drug Alcohol Depend, 2013. [DOI | PubMed]
- JC Winter, RA Filipink, D Timineri, SE Helsley, RA Rabin. The paradox of 5-methoxy-N, N-dimethyltryptamine: an indoleamine hallucinogen that induces stimulus control via 5-HT1A receptors. Pharmacol Biochem Behav, 2000. [DOI | PubMed]
- V Wolff, E Jouanjus. Strokes are possible complications of cannabinoids use. Epilepsy Behav, 2017. [DOI | PubMed]
- DM Wood, J Button, S Lidder, J Ramsey, DW Holt, PI Dargan. Dissociative and sympathomimetic toxicity associated with recreational use of 1-(3-trifluoromethylphenyl) piperazine (TFMPP) and 1-benzylpiperzine (BZP). J Med Toxicol, 2008. [DOI | PubMed]
- DM Wood, JJ Looker, L Shaikh, J Button, M Puchnarewicz, S Davies, S Lidder, J Ramsey, DW Holt, PI Dargan. Delayed onset of seizures and toxicity associated with recreational use of Bromo-dragonFLY. J Med Toxicol, 2009. [DOI | PubMed]
- DM Wood, S Davies, SL Greene, J Button, DW Holt, J Ramsey, PI Dargan. Case series of individuals with analytically confirmed acute mephedrone toxicity. Clin Toxicol (Phila), 2010. [DOI | PubMed]
- DM Wood, AD Brailsford, PI Dargan. Acute toxicity and withdrawal syndromes related to gamma-hydroxybutyrate (GHB) and its analogues gamma-butyrolactone (GBL) and 1,4-butanediol (1,4-BD). Drug Test Anal, 2011. [DOI | PubMed]
- DM Wood, S Davies, M Puchnarewicz, A Johnston, PI Dargan. Acute toxicity associated with the recreational use of the ketamine derivative methoxetamine. Eur J Clin Pharmacol, 2012. [DOI | PubMed]
- DM Wood, R Sedefov, A Cunningham, PI Dargan. Prevalence of use and acute toxicity associated with the use of NBOMe drugs. Clin Toxicol (Phila), 2015. [DOI | PubMed]
- TH Wright, K Cline-Parhamovich, D Lajoie, L Parsons, M Dunn, KE Ferslew. Deaths involving methylenedioxypyrovalerone (MDPV) in Upper East Tennessee. J Forensic Sci, 2013. [DOI | PubMed]
- JF Wyman, ES Lavins, D Engelhart, EJ Armstrong, KD Snell, PD Boggs, SM Taylor, RN Norris, FP Miller. Postmortem tissue distribution of MDPV following lethal intoxication by "bath salts". J Anal Toxicol, 2013. [DOI | PubMed]
- AB Yazici, E Yazici, A Erol. Delirium and high creatine kinase and myoglobin levels related to synthetic cannabinoid withdrawal. Case Rep Med, 2017. [DOI | PubMed]
- RR Yeruva, HM Mekala, M Sidhu, S Lippmann. Synthetic cannabinoids–“Spice" can induce a psychosis: a brief review. Innov Clin Neurosci, 2019. [PubMed]
- G Yirgin, I Ates, B Katipoglu, BF Demir, N Yilmaz. Pulmonary embolism due to synthetic cannabinoid use: case report. Turk Kardiyol Dern Ars, 2018. [DOI | PubMed]
- K Yonemitsu, A Sasao, S Mishima, Y Ohtsu, Y Nishitani. A fatal poisoning case by intravenous injection of "bath salts" containing acetyl fentanyl and 4-methoxy PV8. Forensic Sci Int, 2016. [DOI | PubMed]
- AC Young, E Schwarz, G Medina, A Obafemi, SY Feng, C Kane, K Kleinschmidt. Cardiotoxicity associated with the synthetic cannabinoid, K9, with laboratory confirmation. Am J Emerg Med, 2012. [DOI]
- S Zaami, R Giorgetti, S Pichini, F Pantano, E Marinelli, FP Busardo. Synthetic cathinones related fatalities: an update. Eur Rev Med Pharmacol Sci, 2018. [DOI | PubMed]
- P Zanos, TD Gould. Mechanisms of ketamine action as an antidepressant. Mol Psychiatry, 2018. [DOI | PubMed]
- C Zarifi, S Vyas. Spice-y kidney failure: a case report and systematic review of acute kidney injury attributable to the use of synthetic cannabis. Perm J, 2017. [DOI | PubMed]
- JB Zawilska. Methoxetamine—a novel recreational drug with potent hallucinogenic properties. Toxicol Lett, 2014. [DOI | PubMed]
- JB Zawilska, J Wojcieszak. An expanding world of new psychoactive substances-designer benzodiazepines. Neurotoxicology, 2019. [DOI | PubMed]
- A Zhao, M Tan, A Maung, M Salifu, M Mallappallil. Rhabdomyolysis and acute kidney injury requiring dialysis as a result of concomitant use of atypical neuroleptics and synthetic cannabinoids. Case Rep Nephrol, 2015. [DOI | PubMed]
- X Zhou, D Luethi, GM Sanvee, J Bouitbir, ME Liechti, S Krähenbühl. Molecular toxicological mechanisms of synthetic cathinones on C2C12 myoblasts. Int J Mol Sci, 2019. [DOI]
- M Zidkova, T Hlozek, M Balik, O Kopecky, P Tesinsky, J Svanda, MA Balikova. Two cases of non-fatal intoxication with a novel street hallucinogen: 3-methoxy-phencyclidine. J Anal Toxicol, 2017. [DOI | PubMed]
- US Zimmermann, PR Winkelmann, M Pilhatsch, JA Nees, R Spanagel, K Schulz. Withdrawal phenomena and dependence syndrome after the consumption of "spice gold". Dtsch Arztebl Int, 2009. [DOI | PubMed]
- DL Zvosec, SW Smith. Agitation is common in γ-hydroxybutyrate toxicity. Am J Emerg Med, 2005. [DOI | PubMed]
- DL Zvosec, SW Smith, T Porrata, AQ Strobl, JE Dyer. Case series of 226 γ-hydroxybutyrate-associated deaths: lethal toxicity and trauma. Am J Emerg Med, 2011. [DOI | PubMed]
